Primer for doctors and researchers
Editors: Edits to this Primer may require the same edits to the other Primers. |
Chronic fatigue syndrome (CFS) is also known as myalgic encephalomyelitis (ME) or ME/CFS. There are many clinical and research definitions, which creates confusion for doctors, researchers, and patients.
It is worth noting that chronic fatigue (without the "syndrome") is not a disease in and of itself, but a symptom of many diseases and drug therapies. This term is not interchangeable with CFS, ME, or ME/CFS.
The core ME/CFS symptoms are: chronic fatigue (CF); post-exertional malaise (PEM); unrefreshing sleep/sleep problems; and cognitive impairment/brain fog and/or orthostatic intolerance (OI).[1][2] A person with ME is likely to have other symptoms as well.[3] Systemic Exertion Intolerance Disease (SEID), an ME/CFS criteria, allows for a patient to be diagnosed with the minimum core symptoms [4][2]. The Canadian Consensus Criteria (CCC) requires the core symptoms along with additional neurological, autonomic, neuroendocrine, and immune symptoms.[5] The International Consensus Criteria (ICC) is used to diagnose myalgic encephalomyelitis (ME) which requires the core symptoms and neurological, immune/gastrointestinal/genitourinary impairment, and energy metabolism/ion transport impairment symptoms for a diagnosis.[6]
Although the Fukuda[7] and the Oxford Criteria[8] have been used for diagnosing CFS, they are broader criteria, making misdiagnosis a concern.[9][10][7][11][12] There have been media reports of athletes diagnosed with myalgic encephalomyelitis (ME) or chronic fatigue syndrome (CFS) who have recovered in a relatively short period of time after rest, supplementation, and diet changes;[13][14][15][16] these athletes may have had overtraining syndrome (which has the symptom of CF) and not ME or CFS.[17] Some people with anemia, allergies, idiopathic chronic fatigue or other fatiguing illnesses are erroneously diagnosed with CFS.[5]
The acronym ME/CFS is widely used in research, by clinicians, patient organizations, and patients.
"The most common overlapping condition with ME/CFS is fibromyalgia."[18][19] While some have posited ME/CFS and fibromyalgia are variants of the same illness, Benjamin Natelson, MD summoned considerable amounts of data that suggest the two illnesses differ with different pathophysiologic processes leading to different treatments.[20]
Unfortunately, a psychiatric approach has been taken with ME/CFS, but this is changing. At this time there are no approved drug treatments. Graded exercise therapy (GET) and cognitive behavioral therapy (CBT) are used in the UK inappropriately for treating ME/CFS. As of 2021 the GET has been scrapped in the UK [1].
The Centers for Disease Control and Prevention (CDC) website states "ME/CFS is a biological illness, not a psychologic disorder" and impacts multiple body systems.[21] The CDC recognizes the hallmark symptom of PEM which is a worsening of symptoms after physical or mental activity[1] and says ME/CFS is a "disabling and complex disease."[22]
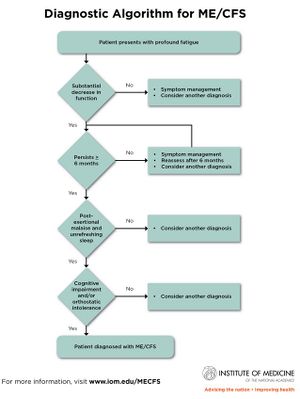
Disease onset and course of illness[edit | edit source]
ME/CFS can begin from many acute/sudden[23] events: usually viral or bacterial infections, but also trauma, surgery or childbirth, allergic reaction, and stress.[24] There is also a gradual onset in some people,[23][25] that is not attributed to any one event. Occasionally, ME/CFS has been triggered by environmental toxins or the receipt of an immunizing injection.[26] Some say that the disease ME always has an acute/sudden infectious onset.[27]
The disease ME/CFS is often diagnosed when a person does not recover from a flu-like illness, mononucleosis or another herpesvirus, Q fever, an unidentified virus, or other infection, and meets one or more diagnostic criteria for either ME, CFS, or ME/CFS.[28][29] Patients experience numerous symptoms and disease severity which fluctuate from day to day, week to week, month to month, year to year, and even decade to decade. Furthermore, symptoms and disease severity vary among patients.[30][31][32]
The CDC recognizes that there can be different causes and it is possible that two or more things could cause the illness. Areas of research include infections, immune system changes, stress affecting body chemistry, changes in energy production, and a possible genetic link.[33][21] The CDC notes there are abnormalities with the immune system, cellular metabolism, neuroendocrine disturbances, and blood pressure or heart rate regulation.[21]
Not a mental health disorder[edit | edit source]
In the past, CFS was believed to be a mental health disorder. This is why the CDC now states: "ME/CFS is a biological illness, not a psychologic disorder. Patients with ME/CFS are neither malingering nor seeking secondary gain. These patients have multiple pathophysiological changes that affect multiple systems."[21]
No clear evidence that ME/CFS is contagious[edit | edit source]
Infectious episodes have led to outbreaks over the years and 72% of ME/CFS patients report an onset of a viral or bacterial infection.[34] Nowadays, the vast majority of ME/CFS cases are sporadic rather than epidemic, and although some outbreaks have been caused by known viruses - such as the SARS pandemic and COVID-19 - there is no clear evidence that sporadic ME/CFS cases are contagious.[35]
Families, partners, and friends do not report contracting ME/CFS from someone with the disease nor do patients report passing it on to others.[36] However, Underhill and O'Gorman (2006) researched 219 patients with ME/CFS, and concluded that close household contact and genetics were both risk factors for CFS, finding 3.2% of spouses/partners of those with CFS also had the illness.[37] This was a higher prevalence than all genetic relatives except children of patients. Because ME/CFS can run in families, a genetic link is a line of research recommended by the CDC.[38]
Michael Sikora and collaborators at the Open Medicine Foundation hope that their research on the role of T cells and immune-related genes will help address "whether ME/CFS is an autoimmune or infectious disease, or simply an activation of the immune system".[39]
Blood donation and organ transplant[edit | edit source]
Patients with ME/CFS are banned from donating blood or tissues in the UK by the UK's National Health Service, including patients who have recovered.[40][41] In the United States a temporary ban on donations from ME/CFS patients was put in place due to the research of XMRV as being the infectious trigger of CFS[42][43] and that patients carried the virus.[42] Two papers on XMRV were retracted as it was a laboratory contamination.[44][45] Currently the US American Red Cross no longer have statements barring transfusions or transplants from ME/CFS patients, but patients are expected to be in "good health" which would exclude most.[46] Patient charities discouraged ME/CFS patients from donating blood,[47] but the American Association of Blood Banks advises to either accept or defer donors based on "clinical judgment of the donor's health status".[48]
New Zealand bans blood donation from anyone with ME/CFS.[49] Australia has a prohibition on blood donation as a precaution because it has not been established if ME/CFS could be caused by a transmissible infection.[50]
Mini-Docs[edit | edit source]
What happens when you have a disease doctors can't diagnose By Jen Brea/TED
Five years ago, TED Fellow Jen Brea became progressively ill with myalgic encephalomyelitis, commonly known as chronic fatigue syndrome, a debilitating illness that severely impairs normal activities and on bad days makes even the rustling of bed sheets unbearable. In this poignant talk, Brea describes the obstacles she's encountered in seeking treatment for her illness, whose root causes and physical effects we don't fully understand, as well as her mission to document through film the lives of patients that medicine struggles to treat.[51][52]
Invisible Illness - Stories of Chronic Fatigue Syndrome By Veronica Weber/Palo Alto Online
This mini documentary reveals 3 stories of people who have been impacted by Chronic Fatigue Syndrome - a little known disease that affects roughly 836,000-2.5 million people in the U.S. and receives little research funding. They share emotions of treating loved ones with the disease, their frustrations of being ignored by members of society and the healthcare industry and express hopes of treatment and research. Video by Veronica Weber/Palo Alto Online[53]
Diagnosis and Management of Myalgic Encephalomyelitis and Chronic Fatigue Syndrome By Dr. David Kaufman/Unrest
This video on the diagnosis and management of myalgic encephalomyelitis and chronic fatigue syndrome is part of the Unrest Continuing Education module, made available through the American Medical Women’s Association and Indiana University School of Medicine, and in partnership with #MEAction. US medical providers can visit: https://www.unrest.film/cme to register to watch Unrest online for free and receive Continuing Education credit.[54]
Epidemiology[edit | edit source]
In the United States, 836,000 - 2.5 million people suffer from ME/CFS. "The total economic costs of ME/CFS are estimated at $17 to $24 billion annually."[2] Some CFS patients can work with job accommodations but 1/3 to 1/2 become unemployed and many rely on SSDI/SSI.[55][56][57]
- All races and cultures are afflicted with ME/CFS.[58][59] Children and adolescents are also diagnosed.[60][61]
- Like many autoimmune and neuro-immune diseases where mostly women are afflicted,[62] the ME/CFS female/male patient ratio per Capelli et al. is 6:1[63] while the CDC states 4:1.[59]
- Pediatric ME/CFS is defined by the CDC[64] and the National Academy of Medicine (NAM)[65] although it is usually diagnosed in adults. [22] "Children below the age of 8 or 9 do not have the symptom pattern of adolescents past puberty. If the onset of the disease occurs during adolescence, the most common time of onset, the pattern is similar to that of adults."[66] The prognosis in adolescents is considered to be better than in adults.[67][35] Children are diagnosed with ME/CFS at three months of illness under SEID and CCC and ME is diagnosed immediately under ICC.[68][2][5][6]
- "Worldwide, there may be as many as 17 – 24 million people with ME/CFS."[69] 25% of ME/CFS patients are housebound or bedbound at some point in their illness.[70][71] 90% of patients are undiagnosed.[22]
- The prognosis for a patient diagnosed with ME/CFS is considered to be poor with only a minority (a median estimate of 5%) returning to pre-morbid levels of functioning.[72] The majority of patients remains significantly impaired. A substantial improvement however is noted in an estimated 40% of patients.[72][73]
Evidence of a disease[edit | edit source]
Symptoms[edit | edit source]
Symptom presentation varies enormously between individuals. Symptom presentation also varies within individuals, as individuals often report that symptoms change over time (increasing or decreasing) and new symptoms may appear while others disappear.[74] There are many symptoms which people with ME/CFS experience, though those listed below are the core symptoms found in all patients.

.[1]




- Post-exertional malaise (PEM) is the hallmark symptom of ME/CFS. After physical or mental exertion (which for some patients can be a shower or making out a to-do list, others grocery shopping, socializing or reading a news article, while some just walking to the mailbox, getting to the doctor or mentally following a T.V. program)[3][78][79] there is a payback of worsening ME/CFS symptoms which can be delayed 24-72 hours or more[80][81][82] and can last 24 hours and even days, weeks, or months.[83][84] The patient will experience even greater fatigue as well as exasperate the flu-like symptoms and body pain. Every patient experiences different symptoms and symptom severity from different activities and exertion output according to how sick he or she is with the disease.[3][78][79] Regarding PEM the CFIDS Association of America states:
This is a term which describes a symptom in which exercise or exertion can bring on malaise (illness). In the case of people with ME/CFS, malaise often occurs during a period some 24-72 hours after exertion. For example, in some cases, a short walk can worsen ME/CFS symptoms two days later. This lack of understanding about the delayed onset of symptoms has, in the past, made it harder to test for ME/CFS. Follow up tests, taken less than 24 hours after an initial exercise test, may show that the patient can still perform activities at the same level (before post exertional malaise has a chance to take hold).[85]
- chronic fatigue
- cognitive dysfunction
- orthostatic intolerance (OI) such as postural orthostatic tachycardia syndrome (POTS) or neurally mediated hypotension (NMH)
- unrefreshing sleep See also: sleep disturbance [4][2]
Other possible symptoms[edit | edit source]
- chronic pain
- immune system
- neurological signs and symptoms See also: neuroinflammation.
- List of symptoms in ME/CFS
Comorbids[edit | edit source]
- fibromyalgia (FMS)
- irritable bowel syndrome (IBS)
- multiple chemical sensitivity (MCS)
- temporomandibular joint disorder (TMJ) [86]
Government guides on symptoms[edit | edit source]
US Government guides on symptoms
Canada guides on symptoms
Biological abnormalities[edit | edit source]
Because there is currently no biomedical test for ME/CFS, many have incorrectly assumed that there are no medical abnormalities found in people with the disease. As a result, ME/CFS symptoms are often considered to be medically unexplained, and therefore psychological in origin. While it is true that the disease is poorly understood, many biological abnormalities have been found in a range of different body systems, particularly in the central nervous system, autonomic nervous system, immune system, and energy metabolism.[87] Unfortunately, none have yet proved to be specific enough to ME/CFS as to be useful as a biomarker of the illness, and many were identified in small studies, which need replication. Whilst there have been abnormalities identified to be associated with the illness, it cannot yet be determined whether these are a cause or consequence of the illness.
Notable studies[edit | edit source]
- Cytokine ("Notable studies")
- Immune findings by Mady Hornig & Ian Lipkin[88]
- List of enterovirus infection studies
- 2014, Neuroinflammation Japanese Neuroinflammation study,[89] Younger's Leptin study[90]
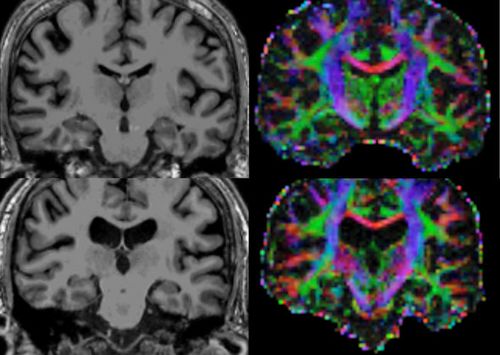
- 2014, Right Arcuate Fasciculus Abnormality in Chronic Fatigue Syndrome[91]
Bilateral white matter atrophy is present in CFS. No differences in perfusion were noted. Right hemispheric increased FA may reflect degeneration of crossing fibers or strengthening of short-range fibers. Right anterior arcuate FA may serve as a biomarker for CFS.
- 2015, Daily cytokine fluctuations, driven by leptin, are associated with fatigue severity in chronic fatigue syndrome: Evidence of inflammatory pathology[90] - (Full text)
- 2016, Metabolic features of chronic fatigue syndrome
- 2019, Evidence of widespread metabolite abnormalities in Myalgic encephalomyelitis/chronic fatigue syndrome: assessment with whole-brain magnetic resonance spectroscopy
- 2018, ME/CFS Involves Brain Inflammation: Results from a Ramsay Pilot Study[92] (TALK)
Causes & triggers[edit | edit source]
- Outbreaks - see List of outbreaks
- Possible infectious triggers: Enteroviruses, Herpesviruses including Epstein-Barr virus[93] Q fever[93], Ross River virus,[93] potentially Ebola,[93]
- Non-viral triggers - physical or psychological trauma, chemical exposure
Epidemiology[edit | edit source]
Prevalence estimates for ME/CFS range between 0.2-2.5%, depending on the definition of the illness used.[6] In the US, estimates range between 836,000 and 2.5 million people with the illness, though true numbers are under-reported. It is estimated that 84-91% of people with the illness remain undiagnosed.[87]
- Level of disability (eg, Norwegian study HRQoL by Hvidberg, 2015) suggests quality of life is LOWER than for many cancers, heart diseases, brain stroke, diabetes I & II, rheumatoid arthritis, chronic renal failure, sclerosis, schizophrenia, COPD, etc)[94]
Severely ill patients[edit | edit source]
Considerable variation exists in the severity of the illness. The International Consensus Criteria lists the following severity levels (it should be noted that even "mild" ME/CFS consists of significant debility):
- Mild = 50% reduction in pre-illness activity levels
- Moderate = mostly housebound
- Severe = mostly bedridden
- Very Severe = totally bedridden, and needing help with basic functions.
At least 25% of people with ME/CFS are bed-bound or housebound, often for years or even decades, so are largely an invisible population.[87] So invisible in fact, that they have rarely been included as part of research because their level of debility precludes them from traveling to laboratories for required testing. The Open Medicine Foundation's ME/CFS Severely Ill, Big Data Study will be the first in-depth study of people with a severe form of ME/CFS.
Notable patients with severe ME/CFS include Whitney Dafoe, Karina Hansen (had been sanctioned), Laura Hillenbrand, Tom Kindlon, Doctor Speedy, Naomi Whittingham, Jen Brea, and Emma Shorter.
Though uncommon, there have been instances of deaths which have been attributed to the disease. (See: Sophia Mirza and Merryn Crofts.) Also, see Vanessa Li and Lynn Gilderdale.
Centers for Disease Control and Prevention (CDC)[edit | edit source]
- Jul 3, 2017, the CDC's Chronic Fatigue Syndrome page has been changed to Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS) and graded exercise therapy (GET) and cognitive behavioral therapy (CBT) recommendations have been removed.[95][96]
- Jul 12, 2018, the "Information for Healthcare Providers" tab and its sub-tabs were updated.[97][98]
- Feb 25, 2019, Dr. Elizabeth Unger, Chief of CDC's Chronic Viral Disease Branch (CVDB), that houses the ME/CFS program, in collaboration between Medscape and the CDC put out brief video and commentary page with links to the CDC's July 12th, 2018 updates for medical professionals: Chronic Fatigue Syndrome: It's Real, and We Can Do Better.[99]
MEAction input
- Jul 29, 2018, CDC Revises its Information on ME The MEAction Network report on the CDC July 2017 and July 2018 website updates. Recommendations for the CDC's ME/CFS page have been created from patient feedback on the updates as well as asking for further patient input.
Tests[edit | edit source]
- Natural killer cell (NKC) Blood Test
- Sleep study for sleep apnea, restless leg syndrome, and other sleep disturbances.
- Tilt table test for OI or POTS.
Treatments[edit | edit source]
There are currently no FDA approved treatments for ME/CFS. Treatments consist mostly of symptom management, rather than treatment of the underlying cause of the condition, which is not yet understood.[100] There are many potential treatments, though their evidence-base is limited, as most research into treatments has gone into psychological approaches to treatment.
Drugs[edit | edit source]
Two treatments that have garnered much attention are Ampligen, produced by AIM ImmunoTech, and Rituximab. Many people have reported benefit from Ampligen;[101]
Attempts to obtain FDA approval for Ampligen in the United States have failed so it is unavailable to many.[102] Argentina approved the use of Ampligen for severe ME/CFS in 2016.[103][104] Also in 2016, it was made available on a limited basis in Europe.[105] In July of 2018, AIM ImmunoTech announced the expansion of its Treatment Protocol/Expanded Access Programs (compassionate use) for ME/CFS in the United States, known as AMP-511, to new patients.[106] AMP-511 "will allow treatment of up to 100 ME/CFS patients at any one time at approved clinical infusion therapy sites."[107] The most recent Ampligen trial was published in 2020.[108]
Rituximab, a lymphoma drug, had shown promising results in initial trials in Norway,[109] and there were groups crowdsourcing funding for further trials in other countries. In 2017, Drs. Øystein Fluge and Olav Mella announced that their Rituximab trial had failed. They stated that they would focus their efforts on attempting to identify a subgroup of ME/CFS patients with an immune profile that would be responsive to Rituximab.[110] A phase III trial published in 2019 showed Rituximab did not improve ME/CFS.[111]
Jarred Younger announced he will be undertaking a trial of low dose naltrexone (LDN) in ME/CFS.[112]
Treating other conditions[edit | edit source]
Different forms of OI are treated with beta-blockers (Metopropol), Fludrocortisone (Florinef), and Pyridostigmine.[113] When treating other diseases, illnesses, and conditions, and ME/CFS comorbidities or overlapping conditions such as sleep difficulties, cognitive problems, pain, and other symptoms it is important to remember that patients are sensitive to medications.[114] The CDC advice to health care practitioners is to be aware that because all drugs can cause side effects, ME/CFS patient symptoms can worsen. "This is particularly true of any medication that acts on the central nervous system, such as sedating medications: therapeutic benefits can often be achieved at lower-than-standard doses. Patients with ME/CFS might tolerate or need only a fraction of the usual recommended doses for medications. After initial management with lower dosing, one or more gradual increases may be considered as necessary and as tolerated by the patient."[114] For instance, tricyclic drugs can improve mood and help with sleep and pain. However, in some in can worsen OI.[114][5]
Exercise as treatment[edit | edit source]

Two common treatment recommendations for ME/CFS are GET and CBT. These treatments are based on the disproven hypothesis that the illness might have begun with a viral infection but has been perpetuated by deconditioning from lack of activity, and fear and avoidance of activity. GET and CBT are aimed at addressing these hypothesized causes by challenging the unhelpful thoughts that are claimed to result in avoidance of activity, and by increasing fitness through a gradual increase in exercise. These treatments are controversial and are at odds with much of the research literature, which provides evidence that exercise is harmful to people with ME/CFS. A large patient survey of treatment responses found that 74% of people who had tried GET, reported that their symptoms subsequently worsened,[115] which is consistent with other patient surveys.[116]
The PACE trial, published in 2011, is the largest GET trial ever conducted. It has received much publicity as a result of its recovery rate claims, though it has come under strong criticism from within both the scientific and patient community for significant flaws in its design, and for overstating (and in some cases misrepresenting) outcomes in both the initial trial, and follow-up studies.[117] The study was the subject of a series of investigative pieces by journalist David Tuller in late 2015, that were highly critical of the trial.[118] A petition signed by almost 12,000 ME/CFS patients and allies,[119] and an open letter signed by 42 ME/CFS experts from around the world,[120] were sent to The Lancet, both calling for the data to be reanalyzed. Twenty-four ME/CFS organizations from 14 different countries have written to Queen Mary University London requesting that the trial data be released for reanalysis.[121] To date, the authors of the trial and editor of The Lancet have refused such requests. Despite such criticism, the PACE trial continues to influence both government and the medical profession's approach to the treatment of ME/CFS in many countries.
One of the reasons that exercise may be harmful to people with ME/CFS, is the presence of post-exertional malaise (PEM), which is an exacerbation of symptoms following physical, mental or even emotional exertion. Studies have revealed immunological, muscular, neurological, autonomic and cardiovascular abnormalities in response to exercise in people with ME/CFS. As these results are not also found in healthy sedentary people, the adverse effects of exercise cannot be said to be due to deconditioning.[122][citation needed][citation needed]
People with ME/CFS should approach exercise with caution, as there is much potential for harm.
Anaerobic threshold, use of heart rate monitors for activity and pacing. Analeptic, not aerobic. Energy envelope/pacing - people do better if stay within their envelope than to push to increase activity
Graded exercise therapy & Cognitive behavioral therapy[edit | edit source]

GET and CBT are usually employed in the UK, Ireland and some parts of Europe through ME Clinics. They are highly controversial and not recommended by patients, most patient advocates, and research organizations nor by many doctors or researchers outside of the UK. Based on the disproven biopsychosocial model of ME/CFS, backed up by the flawed PACE trial which used the flawed Oxford criteria to diagnose and recruit patients, GET and CBT found its way into treating people with ME/CFS.
Exercise, especially GET, can harm an ME/CFS patient further.
- Jennifer Brea walked home from her Neurologist's office and became wheelchair-bound.
- This is an experience of serious injury due to GET shared by K. Miles, via Tom Kindlon on Twitter.
- Emma Shorter was able to walk a few minutes a day until GET put her in a wheelchair.
- Dr Maik Speedy was also seriously injured by GET and has been bedbound since.
- British MP Brynmor John collapsed outside the House of Commons gym in 1998 and died, as a result of following his doctor's advice to exercise back to health.
Claims of recovery and cures[edit | edit source]
Charlatans claim they can cure CFS (per the CDC "there is no cure"[123]) when in reality they may be able to treat chronic fatigue (CF) which is not the result of the neurological illness CFS. Some people misdiagnosed and "recovered" from CFS most likely had CF which can be caused by many illnesses, diseases, and drug therapies or a bad year or two perhaps with mononucleosis followed by a bout or two of influenza. These individuals were experiencing a proper immune response whereas ME/CFS patients experience an ongoing improper immune response and other abnormalities for at least 6 months straight with a reduction in activity with a specific symptom set for at least 50% of the time.[21][124][125]
Additionally, there have been media reports of some professional or amateur athletes diagnosed with CFS that recovered in a relatively short period of time after rest, supplementation, and diet changes [13][14][15][16] that may have had overtraining syndrome,[17] while some people with Addison's disease (adrenal failure) are erroneously diagnosed with CFS.[113][5]
Notable studies[edit | edit source]
- Pathways to prevention report (P2P)
- Institute of Medicine report
- PACE trial is a highly criticized UK trial designed by psychiatrists to promote GET and CBT as therapy which is deemed harmful and useless for ME/CFS patients by many clinicians, researchers, patients, and advocates.
Continuing education (CME and CE)[edit | edit source]
- Update on Chronic Fatigue Syndrome Part 1: Clinical Diagnostic Criteria for Chronic Fatigue Syndrome/CFS now called Myalgic Encephalomyelitis or ME/CFS[126] (CME)
- Update on Chronic Fatigue Syndrome Part 2: Uniting Compassion, Attention and Innovation to treat ME/CFS.[127] (CME)
- Diagnosing Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: The Experts Weigh In[128] (CME/CE)
- Watch Unrest and Receive Continuing Medical Education (CME /CE) Credit[129]
History[edit | edit source]
- Osler's Web is a book by Hillary Johnson on the early history of CFS.
- Thirty Years of Disdain by Mary Dimmock and Matthew Lazell-Fairman picks up on the ME/CFS history where Osler's Web leaves off.
Deaths of ME/CFS patients[edit | edit source]
Death certificates with ME or CFS
- Merryn Crofts' death is attributed to ME.
- Sophia Mirza's death is attributed to CFS.
In the UK, United States, and Australia there are further reports of loved ones who have died due to ME/CFS.[130] See Editor's Note[131]
See also[edit | edit source]
- List of systematic reviews about ME/CFS/SEID
- International Consensus Criteria - with primer for clinicians
- misdiagnosis of myalgic encephalomyelitis and chronic fatigue syndrome
- Fibromyalgia
- PACE trial
- Primer for patients
- Primer for the public (Disease names and acronyms around the world section)
Learn more[edit | edit source]
Films
- Forgotten Plague is a US documentary about Ryan Prior, an afflicted journalist who investigates the disease and its history and why the CDC has left millions sidelined from life; available for streaming and DVD purchase. (2015)

- Unrest is a US documentary film that aired on PBS's Independent Lens in 2018 and is available for streaming and DVD purchase. Jennifer Brea, a person with ME, directs. (2017)

ME/CFS organization's and researcher's material
- Beyond the Data – Chronic Fatigue Syndrome: Advancing Research and Clinical Education[132]
- Caring for People with Myalgic Encephalomyelitis[133]
- IACFS/ME Primer for Clinical Practitioners - 2014 Edition[100]
- ME Association clinical guidance[134]
- ME/CFS Diagnosis and Name with Dr Nancy Klimas (video)[135]
- ME/CFS Treatment Resource Guide for Practitioners by A Martin Lerner, MD[136]
- Myalgic Encephalomyelitis - Adult & Pediatric - International Consensus Criteria Primer for Medical Practitioners[113]
- What is ME/CFS?[3]
- Patients who were deemed as suffering from mental health rather than a biological illness:
- Karina Hansen is a young Danish woman taken from her family for 3 1/2 years due to Per Fink's insistence her ME was due to mental health issues.
- Sophia Mirza was taken forcibly from her home to a mental hospital only to be returned shortly after; she then died of ME.
- Ean Proctor was taken from his parents as a young boy and he was told his "parents were letting him die." He had become paralyzed and mute and was let go in the deep end of a pool to make him swim, and put on a scary theme park ride to scare him into moving.
More mental health information
- ME/CFS is not depression. It causes a lack of energy, not a lack of desire to do activities.[137][138][139]
Research
- 2015, Institute of Medicine report (IOM Report)
- 2016, The biological challenge of myalgic encephalomyelitis/chronic fatigue syndrome: a solvable problem[140]
- 2018, The CDC based it's updated ME/CFS page based on the IOM Report.
- Notable studies
Articles and blogs
- Feb 21, 2019 Are surgeons missing the major differential diagnosis that is more common than multiple sclerosis and HIV combined?[141]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 "Symptoms of ME/CFS | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)". Centers for Disease Control and Prevention. January 18, 2019. Retrieved January 22, 2019.
- ↑ 2.0 2.1 2.2 2.3 2.4 "Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome - Redefining an Illness | Clinicians' Guide" (PDF). National Academies. 2015. pp. 9–10.
- ↑ 3.0 3.1 3.2 3.3 "What is ME/CFS?". Open Medicine Foundation. Retrieved August 23, 2018.
- ↑ 4.0 4.1 "Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Redefining an Illness - Diagnostic Algorithm". nationalacademies.org. 2015.
- ↑ 5.0 5.1 5.2 5.3 5.4 Carruthers, Bruce M.; Jain, Anil Kumar; De Meirleir, Kenny L.; Peterson, Daniel L.; Klimas, Nancy G.; Lerner, A. Martin; Bested, Alison C.; Flor-Henry, Pierre; Joshi, Pradip; Powles, AC Peter; Sherkey, Jeffrey A.; van de Sande, Marjorie I. (2003). "Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Clinical Working Case Definition, Diagnostic and Treatment Protocols" (PDF). Journal of Chronic Fatigue Syndrome. 11 (2): 7–115. doi:10.1300/J092v11n01_02.
- ↑ 6.0 6.1 6.2 Carruthers, Bruce M.; van de Sande, Marjorie I.; De Meirleir, Kenny L.; Klimas, Nancy G.; Broderick, Gordon; Mitchell, Terry; Staines, Donald; Powles, A.C. Peter; Speight, Nigel; Vallings, Rosamund; Bateman, Lucinda; Baumgarten-Austrheim, Barbara; Bell, David; Carlo-Stella, Nicoletta; Chia, John; Darragh, Austin; Jo, Daehyun; Lewis, Donald; Light, Alan; Marshall-Gradisnik, Sonya; Mena, Ismael; Mikovits, Judy; Miwa, Kunihisa; Murovska, Modra; Pall, Martin; Stevens, Staci (August 22, 2011). "Myalgic encephalomyelitis: International Consensus Criteria". Journal of Internal Medicine. 270 (4): 327–338. doi:10.1111/j.1365-2796.2011.02428.x. ISSN 0954-6820. PMC 3427890. PMID 21777306.
- ↑ 7.0 7.1 Fukuda, K.; Straus, S.E.; Hickie, I.; Sharpe, M.C.; Dobbins, J.G.; Komaroff, A. (December 15, 1994). "The chronic fatigue syndrome: a comprehensive approach to its definition and study. International Chronic Fatigue Syndrome Study Group" (PDF). Annals of Internal Medicine. American College of Physicians. 121 (12): 953–959. doi:10.7326/0003-4819-121-12-199412150-00009. ISSN 0003-4819. PMID 7978722.
- ↑ Sharpe, M C; Archard, L C; Banatvala, J E; Borysiewicz, L K; Clare, A W; David, A; Edwards, RH; Hawton, KE; Lambert, HP (February 1991). "A report--chronic fatigue syndrome: guidelines for research". Journal of the Royal Society of Medicine. 84 (2): 118–121. ISSN 0141-0768. PMC 1293107. PMID 1999813.
- ↑ Chronic Fatigue Versus Chronic Fatigue Syndrome - About.com Health - By: Carol Eustice
- ↑ "What Does a True ME Definition Look Like?". MEadvocacy.org. Retrieved January 25, 2019.
- ↑ US NIH Report Calls for UK Definition of ME/CFS to be Scrapped - The Argus Report By: Penny Swift
- ↑ Spotila, Jennie; Dimmock, Mary (August 16, 2016). "AHRQ Evidence Review Changes Its Conclusions". occupyme.net. Retrieved January 25, 2019.
- ↑ 13.0 13.1 Tanner, Claudia (2018). "Marathon runner forced to quit work after developing ME claims diet change gave him his life back". iNews.
- ↑ 14.0 14.1 Broadbent, Rick (December 2, 2017). "Muslim fighter with ME who left an arranged marriage to win world". The Times. ISSN 0140-0460. Retrieved February 28, 2019.
- ↑ 15.0 15.1 Park, Andy; O'Halloran, Clare. "Committee reviews 'potentially harmful and old fashioned' chronic fatigue treatments". ABC News. 6mins 18s.
- ↑ 16.0 16.1 Broadbent, Rick (February 27, 2019). "Nathan Douglas: London 2012 was the darkest period of my life". The Times. ISSN 0140-0460. Retrieved February 28, 2019.
- ↑ 17.0 17.1 Spence, Vance. "Snippets | A presentation by MERGE Chairman Dr Vance Spence on 12 November 2005 at the Oak Tree Court Conference Centre, Coventry, at the invitation of the Warwickshire Network for ME". Irish M.E. Association.
- ↑ "Overlapping Conditions - American Myalgic Encephalomyelitis and Chronic Fatigue Syndrome Society". American Myalgic Encephalomyelitis and Chronic Fatigue Syndrome Society. Retrieved August 12, 2018.
- ↑ Jason, Leonard; Taylor, R.R.; Kennedy, C.L.; Song, S; Johnson, D; Torres, S.R. (January 1, 2001). "Chronic fatigue syndrome: Comorbidity with fibromyalgia and psychiatric illness". Medicine and Psychiatry. 4: 29–34.
- ↑ Natelson, Benjamin H. (February 19, 2019). "Myalgic Encephalomyelitis/Chronic Fatigue Syndrome and Fibromyalgia: Definitions, Similarities, and Differences". Clinical Therapeutics. 41 (4): 612. doi:10.1016/j.clinthera.2018.12.016. ISSN 0149-2918. PMID 30795933.
- ↑ 21.0 21.1 21.2 21.3 21.4 "Etiology and Pathophysiology | Presentation and Clinical Course | Healthcare Providers | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Centers for Disease Control and Prevention. July 10, 2018. Retrieved September 7, 2018.
- ↑ 22.0 22.1 22.2 "What is ME/CFS? | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)". Centers for Disease Control and Prevention. January 18, 2019. Retrieved April 12, 2019.
- ↑ 23.0 23.1 Chu, Lily; Valencia, Ian J.; Garvert, Donn W.; Montoya, Jose G. (January 14, 2019). "Onset patterns and course of myalgic encephalomyelitis/chronic fatigue syndrome". Frontiers in Pediatrics. doi:10.3389/fped.2019.00012.
- ↑ "CDC Public Health Grand Rounds - Chronic Fatigue Syndrome - Advancing Research and Clinical Education" (PDF). cdc.gov. p. 6.
- ↑ "Presentation and Clinical Course of ME/CFS | Information for Healthcare Providers | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome ME/CFS". Centers for Disease Control and Prevention. December 12, 2018. Retrieved February 7, 2019.
- ↑ Chronic Fatigue Syndrome Myalgic Encephalomyelitis - Primer for Clinical Practitioners - 2014 Edition - Massachusettes CFIDS/FM Assoc
- ↑ Evans, Meredyth; Jason, Leonard (2018). "Onset patterns of chronic fatigue syndrome and myalgic encephalomyelitis" (PDF). Research on Chronic Diseases: 2.
- ↑ IOM Report - INFECTION
- ↑ The Lipkin Study, The Vagus Nerve Infection Hypothesis and HHV-6: Kristin Loomis of the HHV-6 Foundation Talks – Pt. I - Health Rising - By: Cort Johnson - June 2014
- ↑ Symptoms and diagnosis of ME/CFS - ME Association
- ↑ Chronic Fatigue Syndrome - Symptoms - Web MD
- ↑ Facts (ME/CFS) Severity
- ↑ "Possible Causes | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)". Centers for Disease Control and Prevention. January 18, 2019. Retrieved January 27, 2019.
- ↑ "CDC Public Health Grand Rounds - Chronic Fatigue Syndrome - Advancing Research and Clinical Education" (PDF). CDC. p. 6.
- ↑ 35.0 35.1 Rowe, Katherine S.; Vallings, Rosamund; Stewart, Julian M.; Speight, Nigel; Schwartz, Malcolm S.; Medow, Marvin S.; Gurwitt, Alan; Friedman, Kenneth J.; Underhill, Rosemary A. (2017). "Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Diagnosis and Management in Young People: A Primer". Frontiers in Pediatrics. 5. doi:10.3389/fped.2017.00121. ISSN 2296-2360.
- ↑ "Is CFS contagious? | ProHealth Fibromyalgia, ME/CFS and Lyme Disease Forums". forums.prohealth.com. Retrieved February 13, 2019.
- ↑ Underhill, Rosemary A.; O'Gorman, Ruth (January 1, 2006). "Prevalence of Chronic Fatigue Syndrome and Chronic Fatigue Within Families of CFS Patients". Journal of Chronic Fatigue Syndrome. 13 (1): 3–13. doi:10.1300/J092v13n01_02. ISSN 1057-3321.
- ↑ "Possible Causes | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Centers for Disease Control and Prevention. January 18, 2019. Retrieved February 13, 2019.
- ↑ "OMF funded research". Open Medicine Foundation. June 4, 2018.
- ↑ "My Donor Record - Health, Eligibility & Travel". my.blood.co.uk. Retrieved April 1, 2021.
- ↑ Target Information Systems Ltd. "Joint United Kingdom (UK) Blood Transfusion and Tissue Transplantation Services Professional Advisory Committee - Transfusion Guidelines". transfusionguidelines.org.uk. Retrieved April 1, 2021.
- ↑ 42.0 42.1 Stein, Rob (December 3, 2010). "Red Cross bars chronic fatigue patients from donating blood". Washington Post.
- ↑ "XMRV testing in the UK". ME Association. 2010. Retrieved February 13, 2019.
- ↑ "Redaction, retraction and reaction". Nature Reviews Microbiology. 10 (12): 799. December 2012. doi:10.1038/nrmicro2928. ISSN 1740-1534.
- ↑ "Multicenter Study Finds No Correlation between Chronic Fatigue Syndrome and XMRV". transfusionnews.com. Retrieved February 13, 2019.
- ↑ "Frequently Asked Questions". American Red Cross. Retrieved February 13, 2019.
Your search for "Chronic fatigue syndrome" returned no results.
- ↑ "AABB's recommendation on ME/CFS and blood donation". Massachusetts ME/CFS & FM Association. November 25, 2015.
- ↑ American Association of Blood Banks (October 2012). "Xenotropic Murine Leukemia Virus-Related Virus (XMRV) and other Polytropic Murine Leukemia Viruses (pMLV)" (PDF). p. 3.
An updated AABB Association Bulletin #12-05 (November 2012) states that individual collectors of blood and cellular therapy products should accept or defer donors with a history of CFS based on their clinical judgment of the donor's health status.
- ↑ "Detailed Eligibility Criteria". NZ Blood. Retrieved May 25, 2022.
People with a diagnosis of Chronic Fatigue Syndrome are permanently ineligible from donating blood in New Zealand
- ↑ https://www.lifeblood.com.au/faq/eligibility/medical-conditions-and-procedures/chronic-fatigue-syndrome
- ↑ Brea, Jennifer (January 17, 2017). "What happens when you have a disease doctors can't diagnose". YouTube. TED.
- ↑ Brea, Jennifer (June 2016). "What happens when you have a disease doctors can't diagnose". TED.
- ↑ Weber, Veronica (July 10, 2015). "Invisible Illness - Stories of Chronic Fatigue Syndrome". YouTube. Palo Alto Online.
- ↑ "Diagnosis and Management of Myalgic Encephalomyelitis and Chronic Fatigue Syndrome". YouTube. Unrest Film. October 16, 2018.
- ↑ Disability for CFS - Phoenix Rising
- ↑ CFS - Womenshealth.gov
- ↑ Job Accommodations - MASS CFIDS
- ↑ Prevalence of myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) in three regions of England: a repeated cross-sectional study in primary care - Bio-Med Central - July 2011
- ↑ 59.0 59.1 "Epidemiology | Presentation and Clinical Course | Healthcare Providers | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Centers for Disease Control and Prevention. November 8, 2018. Retrieved January 29, 2019.
- ↑ "ME/CFS in Children | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Centers for Disease Control and Prevention. January 18, 2019. Retrieved January 29, 2019.
- ↑ "Pediatric ME/CFS Home Page". massmecfs.org. Retrieved January 29, 2019.
- ↑ Fact Sheet Autoimmune Disease in Women: NWHIC - Right Diagnosis - Aug 2015
- ↑ Capelli, E.; Zola, R.; Lorusso, L.; Venturini, L.; Sardi, F.; Ricevuti, G. (October 2010). "Chronic fatigue syndrome/myalgic encephalomyelitis: an update". International Journal of Immunopathology and Pharmacology. 23 (4): 981–989. doi:10.1177/039463201002300402. ISSN 0394-6320. PMID 21244747.
- ↑ "Pediatric ME/CFS: Fact Sheet for Healthcare Professionals | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Centers for Disease Control and Prevention. October 10, 2017. Retrieved October 13, 2018.
- ↑ "Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome | Pediatric ME/CFS". The National Academies Press: 181. March 16, 2015. doi:10.17226/19012.
- ↑ Bell, David S. (June 25, 2016). "ME/CFS in Children". Open Medicine Foundation. Retrieved August 11, 2018.
- ↑ "Prognosis | Presentation and Clinical Course | Healthcare Providers | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Centers for Disease Control and Prevention. July 10, 2018. Retrieved October 28, 2018.
- ↑ "Pediatric ME/CFS links". Massachusetts ME/CFS & FM Association. Retrieved August 11, 2018.
- ↑ "How Many People Have ME/CFS?". American Myalgic Encephalomyelitis and Chronic Fatigue Syndrome Society. Retrieved January 31, 2019.
- ↑ "Myalgic Encelphalomyelitis/Chronic Fatigue Syndrome (ME/CFS) Key Facts" (PDF). National Academies. 2015.
- ↑ "Chapter 4". Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Redefining an Illness. National Academies of Medicine. 2015. p. 32.
- ↑ 72.0 72.1 Cairns, R.; Hotopf, M. (January 2005). "A systematic review describing the prognosis of chronic fatigue syndrome". Occupational Medicine (Oxford, England). 55 (1): 20–31. doi:10.1093/occmed/kqi013. ISSN 0962-7480. PMID 15699087.
- ↑ Joyce, J.; Hotopf, M.; Wessely, S. (March 1997). "The prognosis of chronic fatigue and chronic fatigue syndrome: a systematic review". QJM: monthly journal of the Association of Physicians. 90 (3): 223–233. ISSN 1460-2725. PMID 9093600.
- ↑ "Symptoms and Diagnosis of ME/CFS | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS) | CDC". Centers for Disease Control and Prevention. January 18, 2019. Retrieved February 1, 2019.
- ↑ Croxall, Jack (January 17, 2019). "I think #TwoFacesofME is a really important hashtag. We're only out and about at our best, and our (more frequent) worst often remains hidden. I'm convinced it's why #MEcfs research funding is so low - the problem isn't visible enough. I'm seriously ill in both these photos.pic.twitter.com/hNjK5140kv". @JackCroxall. Retrieved January 17, 2019.
- ↑ Karen (January 17, 2019). "First photo, me in my wheelchair on a rare trip out. Second photo, the inevitable crash. Eye half closed, slurred speech, dizzy, weak, etc. #TwoFacesofMEpic.twitter.com/P2OPnnpQvF". @hopeforMEyet. Retrieved January 17, 2019.
- ↑ Köhler, Henry (January 17, 2019). "#TwoFacesofME First photo from the morning, the other one from the afternoon ( when I failed to nap 30-60 minutes). I am Not severely ill, and my life is ok, even do I wish that one day science will help me & all the #MeCfs sufferers around the globe.pic.twitter.com/wmhfHcfP0p". @Authorportrait. Retrieved January 17, 2019.
- ↑ 78.0 78.1 Spotlia, Jenny (August 6, 2010). "Unraveling Post-exertional Malaise By Jennifer M. Spotila, J.D." Phoenix Rising. Phoenix Rising. Retrieved October 16, 2018.
- ↑ 79.0 79.1 Chronic Fatigue Syndrome - Symptoms - Web MD
- ↑ Hartley, Simon. "International CFS/ME Awareness Day - 12th May 2019". whathealth.com. Retrieved October 16, 2018.
- ↑ Lindheimer, Jacob B.; Meyer, Jacob D.; Stegner, Aaron J.; Dougherty, Ryan J.; Van Riper, Stephanie M.; Shields, Morgan; Reisner, Amanda; Shukla, Sanjay K.; Light, Alan R. (April 3, 2017). "Symptom variability following acute exercise in myalgic encephalomyelitis/chronic fatigue syndrome: a perspective on measuring post-exertion malaise". Fatigue: Biomedicine, Health & Behavior. 5 (2): 69–88. doi:10.1080/21641846.2017.1321166. ISSN 2164-1846.
- ↑ Yoshiuchi, Kazuhiro; Cook, Dane B.; Ohashi, Kyoko; Kumano, Hiroaki; Kuboki, Tomifusa; Yamamoto, Yoshiharu; Natelson, Benjamin H. (December 5, 2007). "A real-time assessment of the effect of exercise in chronic fatigue syndrome". Physiology & Behavior. 92 (5): 963–968. doi:10.1016/j.physbeh.2007.07.001. ISSN 0031-9384. PMC 2170105. PMID 17655887.
- ↑ VanNess, J. Mark; Stevens, Staci R.; Bateman, Lucinda; Stiles, Travis L.; Snell, Christopher R. (February 2010). "Postexertional malaise in women with chronic fatigue syndrome". Journal of Women's Health (2002). 19 (2): 239–244. doi:10.1089/jwh.2009.1507. ISSN 1931-843X. PMID 20095909.
- ↑ The Voice of the Patient. A series of reports from the U.S. Food and Drug Administration's (FDA) Patient-Focused Drug Development Initiative. September 2013
- ↑ What Health - International CFS/ME Awareness Day 2017 - CFIDS Association of America
- ↑ What is ME/CFS? - Solve ME/CFS Initiative
- ↑ 87.0 87.1 87.2 Institute of Medicine (US) (February 10, 2015). Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Redefining an Illness. Washington, DC, US: The National Academies Press. ISBN 978-0-309-31689-7.
- ↑ Hornig, Mady; Montoya, José G; Klimas, Nancy G; Levine, Susan; Felsenstein, Donna; Bateman, Lucinda; Peterson, Daniel L; Gottschalk, C Gunnar; Schultz, Andrew F; Che, Xiaoyu; Eddy, Meredith L; Komaroff, Anthony L; Lipkin, W Ian (February 1, 2015). "Distinct plasma immune signatures in ME/CFS are present early in the course of illness". Science Advances. 1 (1).
- ↑ Nakatomi, Yasuhito; Mizuno, Kei; Ishii, Ishii; Yasuhiro, Wada; Masaaki, Tanaka; Shusaku, Tazawa; Kayo, Onoe; Sanae, Fukuda; Joji, Kawabe; Kazuhiro, Takahashi; Yosky, Kataoka; Susumu, Shiomi; Kouzi, Yamaguti; Masaaki, Inaba; Hirohiko, Kuratsune; Yasuyoshi, Watanabe (March 24, 2014). "Neuroinflammation in Patients with Chronic Fatigue Syndrome/Myalgic Encephalomyelitis: An ¹¹C-(R)-PK11195 PET Study". Journal of Nuclear Medicine. 55 (6): 945-50. doi:10.2967/jnumed.113.131045. PMID 24665088.
- ↑ 90.0 90.1 Stringer, EA; Baker, KS; Carrol, IR; Montoya, JG; Chu, L; Maeker, HT; Younger, JW (April 9, 2013). "Daily cytokine fluctuations, driven by leptin, are associated with fatigue severity in chronic fatigue syndrome: Evidence of inflammatory pathology". J Transl Med. doi:10.1186/1479-5876-11-93. PMC 3637529. PMID 23570606.
- ↑ Zeineh, Michael M.; Kang, James; Atlas, Scott W.; Raman, Mira M.; Reiss, Allan L.; Norris, Jane L.; Valencia, Ian; Montoya, Jose G. (February 2015). "Right Arcuate Fasciculus Abnormality in Chronic Fatigue Syndrome". Radiology. 274 (2): 517–526. doi:10.1148/radiol.14141079. ISSN 0033-8419.
- ↑ Younger, Jarred (December 14, 2018). "ME/CFS Involves Brain Inflammation: Results from a Ramsay Pilot Study". YouTube. SolveCFS.
- ↑ 93.0 93.1 93.2 93.3 Hickie, Ian; Davenport, Tracey; Wakefield, Denis; Vollmer-Conna, Ute; Cameron, Barbara; Vernon, Suzanne D; Reeves, William C; Lloyd, Andrew; Dubbo Infection Outcomes Study Group (September 14, 2006). "Post-infective and chronic fatigue syndromes precipitated by viral and non-viral pathogens: prospective cohort study". BMJ. 333 (575). doi:10.1136/bmj.38933.585764.AE. PMID 16950834.
- ↑ Hvidberg, Michael Falk; Brinth, Louise Schouborg; Olesen, Anne V; Petersen, Karin D; Ehlers, Lars (July 6, 2015). "The Health-Related Quality of Life for Patients with Myalgic Encephalomyelitis / Chronic Fatigue Syndrome (ME/CFS)". PLoS One. doi:10.1371/journal.pone.0132421.
- ↑ Tuller, David (July 10, 2017). "Trial By Error: The CDC Drops CBT/GET". Virology blog. Retrieved August 23, 2018.
- ↑ "Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS) | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)". Centers for Disease Control and Prevention. July 3, 2018. Retrieved August 23, 2018.
- ↑ Information for Healthcare Providers - ME/CFS - CDC.gov
- ↑ "New ME/CFS Web Content for Healthcare Providers | CDC Online Newsroom | CDC". Centers for Disease Control and Prevention. July 12, 2018. Retrieved August 23, 2018.
- ↑ Unger, Elizabeth; Medscape (February 25, 2019). "Chronic Fatigue Syndrome: It's Real, and We Can Do Better". Medscape. Retrieved February 25, 2019.
- ↑ 100.0 100.1 International Association for Chronic Fatigue Syndrome / Myalgic Encephalomyelitis (IACFS/ME); Friedberg, Fred; Bateman, Lucinda; Bested, Alison C; Davenport, Todd; Friedman, Kenneth J; Gurwitt, Alan R; Jason, Leonard A; Lapp, Charles W; Stevens, Staci R; Underhill, Rosemary A; Vallings, Rosamund (July 2014). "2014 Primer for Clinical Practitioners (CFS/ME)" (PDF). IACFS/ME.
- ↑ Mariani, Mike (September 3, 2019). "A Town for People with Chronic-Fatigue Syndrome". New Yorker. Retrieved April 13, 2022.
- ↑ "Experimental treatments". American Myalgic Encephalomyelitis and Chronic Fatigue Syndrome Society. Retrieved March 18, 2021.
- ↑ Hemispherx Biopharma Inc (August 23, 2016). "Hemispherx Biopharma Announces Major Breakthrough: Approval for Commercial Sale of Rintatolimod (U.S. Tradename: Ampligen®) to Treat Severe Cases of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS) in the Argentine Republic". GlobeNewswire News Room. Retrieved August 13, 2018.
- ↑ "Hemispherx Biopharma, Inc. Executive Informational Overview" (PDF). Crystal Research Associates. November 27, 2016.
- ↑ George, John (July 25, 2016). "Hemispherx ships Ampligen for European chronic fatigue syndrome program". bizjournals.com. Retrieved August 13, 2018.
- ↑ Hemispherx BioPharma : Opens FDA-Approved Reimbursement Based Expanded Access Treatment Program for ME/CFS to New Enrollees - 4 Traders
- ↑ "Hemispherx Biopharma Inc. Announces Advancement in Expanded Access Program for Ampligen in the Treatment of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". finance.yahoo.com. GlobeNewswire. January 2, 2019. Retrieved February 10, 2019.
- ↑ Strayer, David R.; Young, Diane; Mitchell, William M. (October 29, 2020). "Effect of disease duration in a randomized Phase III trial of rintatolimod, an immune modulator for Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". PLOS ONE. 15 (10): e0240403. doi:10.1371/journal.pone.0240403. ISSN 1932-6203. PMC 7595369. PMID 33119613.
- ↑ Fluge, Øystein; Risa, Kristin; Lunde, Sigrid; Alme, Kine; Rekeland, Ingrid Gurvin; Sapkota, Dipak; Kristoffersen, Einar Kleboe; Sørland, Kari; Bruland, Ove (July 1, 2015). van der Feltz-Cornelis, Christina (ed.). "B-Lymphocyte Depletion in Myalgic Encephalopathy/ Chronic Fatigue Syndrome. An Open-Label Phase II Study with Rituximab Maintenance Treatment". PLOS ONE. 10 (7): e0129898. doi:10.1371/journal.pone.0129898. ISSN 1932-6203. PMC 4488509. PMID 26132314.
- ↑ "Norwegian Rituximab Chronic Fatigue Syndrome (ME/CFS) Trial Fails". Simmaron Research. November 26, 2017. Retrieved April 23, 2019.
- ↑ Fluge, Øystein; Rekeland, Ingrid G.; Lien, Katarina; Thürmer, Hanne; Borchgrevink, Petter C.; Schäfer, Christoph; Sørland, Kari; Aßmus, Jörg; Ktoridou-Valen, Irini (April 2, 2019). "B-Lymphocyte Depletion in Patients With Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: A Randomized, Double-Blind, Placebo-Controlled Trial". Annals of Internal Medicine. doi:10.7326/M18-1451. ISSN 1539-3704. PMID 30934066.
- ↑ Younger, Jarred (December 12, 2016). "2017 Study -- Low Dose Naltrexone for Chronic Fatigue Syndrome". YouTube. Younger Lab.
- ↑ 113.0 113.1 113.2 Carruthers, BM; van de Sande, MI; De Meirleir, KL; Klimas, NG; Broderick, G; Mitchell, T; Staines, D; Powles, ACP; Speight, N; Vallings, R; Bateman, L; Bell, DS; Carlo-Stella, N; Chia, J; Darragh, A; Gerken, A; Jo, D; Lewis, DP; Light, AR; Light, KC; Marshall-Gradisnik, S; McLaren-Howard, J; Mena, I; Miwa, K; Murovska, M; Stevens, SR (2012), Myalgic encephalomyelitis: Adult & Paediatric: International Consensus Primer for Medical Practitioners (PDF), ISBN 978-0-9739335-3-6
- ↑ 114.0 114.1 114.2 "Monitoring the Use of All Medicines and Supplements | Clinical Care of Patients | Healthcare Providers | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS) | CDC". Centers for Disease Control and Prevention. November 8, 2018. Retrieved January 27, 2019.
- ↑ ME Association (UK) (May 29, 2015). "Our CBT, GET and Pacing Report calls for major changes to therapies offered for ME/CFS".
- ↑ "Norwegian patient survey: Experiences of therapeutic approaches (2012)", Phoenix Rising Forum, February 22, 2016
- ↑ Coyne, James Charles; Laws, Keith R (2016). "Results of the PACE follow-up study are uninterpretable". The Lancet Psychiatry. 3 (2): e6–e7. doi:10.1016/S2215-0366(15)00551-9. ISSN 2215-0366.
- ↑ "List of ME/CFS articles published at Virology Blog".
- ↑ #MEAction (October 2015). "Petition: Misleading Claims Should Be Retracted". #MEAction.
- ↑ Davis, Ronald W; Edwards, Jonathan C W; Jason, Leonard A; Levin, Bruce; Racaniello, Vincent R; Reingold, Arthur L; Ablashi, Dharam V; Baraniuk, James N; Barcellos, Lisa F; Bateman, Lucinda; Bell, David S; Bested, Alison C; Broderick, Gordon; Chia, John; Chu, Lily; Enlander, Derek; Fletcher, Mary Ann; Friedman, Kenneth; Kaufman, David L; Klimas, Nancy; Lapp, Charles W; Levine, Susan; Light, Alan R; Marshall-Gradisnik, Sonya; Medveczky, Peter G; Nahle, Zaher; Oleske, James M; Podell, Richard N; Shepherd, Charles; Snell, Christopher R; Speight, Nigel; Staines, Donald; Stark, Philip B; Stein, Eleanor; Swartzberg, John; Tompkins, Ronald G; Underhill, Rosemary; Vallings, Rosamund; VanElzakker, Michael; Weir, William; Zinn, Marcie L; Zinn, Mark A (February 10, 2016). "An open letter to the Lancet - again". Virology blog.
- ↑ #MEAction (March 13, 2016). "24 organisations in 14 countries tell QMUL: Release the PACE data".
- ↑ Twisk, Frank NM; Geraghty, Keith J (July 11, 2015). "Deviant Cellular and Physiological Responses to Exercise in Myalgic Encephalomyelitis and Chronic Fatigue Syndrome" (PDF). Jacobs Journal of Physiology. 1 (2): 007.
- ↑ "Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS) | Treatment". Centers for Disease Control and Prevention. July 3, 2018. Retrieved November 22, 2021.
- ↑ "IOM 2015 Diagnostic Criteria | Diagnosis | Healthcare Providers | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Centers for Disease Control and Prevention. July 10, 2018. Retrieved September 7, 2018.
- ↑ "Proposed Approach to ME/CFS Diagnosis in Children and Adults | Diagnosis | Healthcare Providers | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Centers for Disease Control and Prevention. July 12, 2018. Retrieved September 7, 2018.
- ↑ Bateman, Lucinda. "Update on Chronic Fatigue Syndrome Part 1: Clinical Diagnostic Criteria for Chronic Fatigue Syndrome/CFS now called Myalgic Encephalomyelitis or ME/CFS". Michigan State Medical Society. Retrieved February 25, 2019 – via On-Demand Webinars.
- ↑ Bateman, Lucinda. "Update on Chronic Fatigue Syndrome Part 2: Uniting Compassion, Attention and Innovation to treat ME/CFS". Michigan State Medical Society. Retrieved February 25, 2019 – via On Demand Webinars.
- ↑ Bateman, Lucinda; Azar, Natalie; Klimas, Nancy; Montoya, Jose. "Diagnosing Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: The Experts Weigh In". Medscape. Retrieved February 25, 2019.
- ↑ Indiana University School of Medicine; American Medical Women's Association. "Unrest Continuing Medical Education Program". UNREST. Retrieved February 25, 2019.
- ↑ "Not, sadly, the first". New Scientist. Retrieved August 23, 2018.
- ↑ Hooper, Rowan (June 16, 2006). "First official UK death from chronic fatigue syndrome". New Scientist. Retrieved August 23, 2018.
- ↑ Iskander, John; Komaroff, Anthony (February 17, 2016). "Beyond the Data – Chronic Fatigue Syndrome: Advancing Research and Clinical Education". YouTube. Centers for Disease Control and Prevention (CDC).
- ↑ "Caregivers Guide to ME". Google Docs (pdf). #MEAction. 2018. Retrieved August 23, 2018.
- ↑ Shepherd, C; Chaudhuri, A (2013). "ME/CFS/PVFS An Exploration of the Key Clinical Issues ('Purple Booklet')".
- ↑ Klimas, Nancy (June 21, 2014). "ME/CFS Diagnosis and Name with Dr. Nancy Klimas". YouTube. ME/CFS Community.
- ↑ Lerner, AM (2011). "ME/CFS Treatment Resource Guide for Practitioners" (PDF).
- ↑ Griffith, J.P.; Zarrouf, F.A. (2008). "A Systematic Review of Chronic Fatigue Syndrome: Don't Assume It's Depression". Primary Care Companion to The Journal of Clinical Psychiatry. 10 (2): 120–128. doi:10.4088/pcc.v10n0206. PMC 2292451. PMID 18458765.
- ↑ Hawk, C; Jason, L; Torres-Harding, S (2006). "Differential diagnosis of chronic fatigue syndrome and major depressive disorder" (PDF). International Journal of Behavioral Medicine. 13 (3): 244-51. doi:10.1207/s15327558ijbm1303_8. PMID 17078775.
- ↑ Myhill, Sarah. "CFS or depression - what are the differences - DoctorMyhill". DrMyhill. Retrieved August 23, 2018.
- ↑ Edwards, JCW; McGrath, S; Baldwin, A; Livingstone, M; Kewley, A (April 2, 2016). "The biological challenge of myalgic encephalomyelitis/chronic fatigue syndrome: a solvable problem". Fatigue: Biomedicine, Health & Behavior. 4 (2): 63–69. doi:10.1080/21641846.2016.1160598.
- ↑ Muirhead, Nina (February 21, 2019). "Are surgeons missing the major differential diagnosis that is more common than multiple sclerosis and HIV combined?". Royal College of Surgeons. Retrieved February 22, 2019.

