Severe and very severe ME

Severe and very severe ME affects about 25% of people with myalgic encephalomyelitis (ME), with patients being housebound or bedbound at some point in their illness,[1] typically needing to use a wheelchair, unable to do any kind of work or study, and often unable to do basic self-care activities unaided.[2] Some people have died of severe ME, including Emily Collingridge, Merryn Crofts, Sophia Mirza.[3][4][5]
What is Severe ME?[edit | edit source]
There is no generally agreed upon description of severe or very severe ME, but different clinical scales can be used to measure the degree of disability.[6][7] Very little research has described the symptoms and experiences of patients with severe ME or very severe ME, much of what is known comes from patient and advocacy groups.
A study of 19 bedbound patients with severe ME and orthostatic intolerance by van Campen et al (2020) found an average 27% decrease in blood flow to the brain during a 20 degree tilt table test that lasted just 15 minutes. Some patients could not tolerate the orthostatic symptoms for 15 mins and had to finish the test early. The patients average 35 years of age and had been ill on average 14 years. All the severely ill patients had abnormal drops in blood flow to the brain.[8]
Severe ME symptom scales[edit | edit source]
Substantial impairment and disability in adults can be measured using the following scales:
- Energy Index Point Score
- Fibromyalgia Impact Questionnaire Revised (FIQR)[7]
- Katz Index of Independence in Activities of Daily Living[9]
- The Lawton Instrumental Activities of Daily Living (IADL) Scale[10]
- Short-Form 36 Item Health Survey which is not specific to ME/CFS
- RAND-36 - available as a free version of SF-36[11]
Scales developed by patient organizations[edit | edit source]
Comparison[edit | edit source]
Some scales have a "ceiling effect" that means severe ME can not adequately be distinguished from very severe ME, or from moderate ME, including the Chalder fatigue scale.[13]
Some patients who are severely ill may not have enough concentration to complete a questionnaire, or may be too ill to communicate, these patients may need another person to complete the rating scale instead, for example a carer or health professional. A pilot study of patients with severe CFS/ME in North East England found that even when visiting patients at home, some were unable to complete a questionnaire or to even attempt to stand.[14]

Very severe ME[edit | edit source]
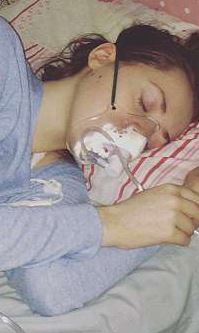
Merryn weighed six stone (84 lbs) and was just 21 years old when she died; her autopsy revealed ganglia inflammation. It is suspected that in the later years of her illness Merryn also suffered from EDS and MCAD. Her death certificate was reported to be the second in the UK to attribute a death to myalgic encephalomyelitis (M.E.).[4]
Doctors initially suggested that Merryn was having panic attacks, and her family were later told that she may have conversion disorder, a mental condition formerly known as hysteria.
"I knew it wasn't. I work with people who have panic attacks and I can talk them down," said Clare.
"Merryn was starting to think 'What if it is in my head?' It made her doubt herself, which is awful."
Eventually a private doctor diagnosed Merryn with ME and she began to receive treatment on the NHS.
Within six months of falling ill she was using a wheelchair, and within a year she was housebound.
A very severe ME patient's experience photo shows clear signs of muscle wasting and disability - but for the majority of patients it remains an invisible illness.

People with very severe ME are totally bedbound and unable to stand at all.[14][15]
Some people with very severe ME have improved over time, or after surgery from cervical spinal stenosis.[16][17]
Notable studies[edit | edit source]
- 2021, Back to the Future? Immunoglobulin Therapy for Myalgic Encephalomyelitis/Chronic Fatigue Syndrome[18] - (Full text)
- IV Immunoglobulin G may be effective for some with severe ME
- 2021, Life-Threatening Malnutrition in Very Severe ME/CFS[19] - (Full text)
- 2021, Caring for the Patient with Severe or Very Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome[20] - (Full text)
- 2021, Comprehensive Examination of Severely Ill ME/CFS Patients[21] - (Full text)
- 2021, The Impact of Severe ME/CFS on Student Learning and K–12 Educational Limitations[22] - (Full text)
- 2021, Elements of Suffering in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: The Experience of Loss, Grief, Stigma, and Trauma in the Severely and Very Severely Affected[23] - (Full text)
- 2021, CFS patients remain severely disabled after specialist treatment with CBT in the UK[24] - (Full text)
- 2021, Systematic Review of Sleep Characteristics in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome[25] - (Full text)
- 2021, Experiences of Living with Severe Chronic Fatigue Syndrome/Myalgic Encephalomyelitis[26] - (Full text)
- 2020, Two-Day Cardiopulmonary Exercise Testing in Females with a Severe Grade of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Comparison with Patients with Mild and Moderate Disease[27] - (Full text)
- 2020, Severe ME in children[28] - (Full text)
- 2020, Reductions in Cerebral Blood Flow Can Be Provoked by Sitting in Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients[29] - (Full text)
- 2020, Cardiac Dimensions and Function are Not Altered among Females with the Myalgic Encephalomyelitis/Chronic Fatigue Syndrome[30] - (Full text)
- 2020, The Lonely, Isolating, and Alienating Implications of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome[31] - (Full text)
- 2020, Validation of the Severity of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome by Other Measures than History: Activity Bracelet, Cardiopulmonary Exercise Testing and a Validated Activity Questionnaire: SF-36[32] - (Full text)
- 2021, Health Care Responsibility and Compassion-Visiting the Housebound Patient Severely Affected by ME/CFS[33] - (Full text)
- 2021, Homebound versus Homebound versus Bedridden Status among Those with Myalgic Encephalomyelitis/Chronic Fatigue Syndrome[34] - (Full text)
- 2021, Three Cases of Severe ME/CFS in Adults[35] - (Full text)
- 2021, Extremely Severe ME/CFS—A Personal Account[36] - (Full text)
- 2020, Cerebral Blood Flow Is Reduced in Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients During Mild Orthostatic Stress Testing: An Exploratory Study at 20 Degrees of Head-Up Tilt Testing[8] - (Full text)
- 2020, The effect of myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) severity on cellular bioenergetic function[38] - (Full text)
- 2018, Improvement of severe ME/CFS symptoms following surgical treatment of cervical spinal stenosis[17] - (Full text)
- 2018, Defining the prevalence and symptom burden of those with self-reported severe chronic fatigue syndrome/myalgic encephalomyelitis (CFS/ME): a two-phase community pilot study in the North East of England.[14] - (Full text)
- 2017, What is known about severe and very severe chronic fatigue syndrome: A scoping review[15] - (Full text)
- 2017, Understanding severely affected chronic fatigue syndrome: CFS the gravity of the situation[39] - (Full text)
- 2016, Housebound versus nonhousebound patients with myalgic encephalomyelitis and chronic fatigue syndrome[40] - (Full text)
- 2016, Caring for People with Severe Myalgic Encephalomyelitis: An Interpretative Phenomenological Analysis of Parents' Experiences[41] - (Full text)
- 2014, What is the current NHS service provision for patients severely affected by chronic fatigue syndrome/myalgic encephalomyelitis? A national scoping exercise[42] - (Full text)
- 2010, Being homebound with chronic fatigue syndrome: a multidimensional comparison with outpatients[43] - (Full text)
- 2009, Risk factors for severe ME/CFS[44] - (Full text)
- 2007, Severe Chronic Fatigue Syndrome: Recovery is possible[45] - (Full text)
- 2000, The course of severe chronic fatigue syndrome in childhood[46] - (Full text)
- 2000, Severe and Very Severe Patients with chronic fatigue syndrome: perceived outcome following an inpatient programme[47] - (Full text)
News articles and interviews[edit | edit source]
- 2022, Epstein-Barr derails NJ man's life; he's pushing for better care: "Trapped in the dark: How chronic fatigue syndrome derailed a NJ musician's life"
- 2021, ME has left me bedbound for eight years – I feel forgotten by the world, North Jersey
- 2020, Three ME patients reveal their daily struggle with the crippling condition, Daily Mail Online
- 2020, How it feels to have Very Severe M.E. by Ruth Braham, via The ME Association
- 2020, Kara Jane Spencer: Musicians help severely ill singer finish album, BBC News
- 2019, UK Teenager with Severe ME Threatened with Forced Institutionalization, #MEAction Network”
- 2019, Severe ME Day: Life in a Nursing Home, Light Sensitivity and Very Severe M.E. by Eira Stuart, via The ME Association
- 2018, Woman, 33, has been living in a dementia ward for FIVE years after falling ill with crippling condition, Daily Mail[48]
- 2018, "I can barely walk and I'm bed-bound 23 hours a day - M.E. nearly killed me" - positive story of partial recovery from very severe ME by Jessica Taylor-Bearman, Mirror Online
- 2017, Bed-bound singer living in silence opens up about how ME stripped her of her voice just weeks after her mum died, The Scottish Sun
- February 27, 2012, Tragic tale of woman with chronic fatigue syndrome 'too tired' to eat, Derby Telegraph
- 2012, ME is often dismissed – but sufferers like Emily Collingridge, The Guardian[3]
- 2010, I've seen patients paralysed, dying Aids victims, starving children... but I've never seen anyone as ill as Lynn, Daily Mail
Patient group surveys[edit | edit source]
- 2014, Severe M.E. Time to Deliver report by Action For ME[49] - (Full text)
See also[edit | edit source]
- HFME 3 Part M.E. Ability and Severity Scale
- List of deaths caused by myalgic encephalomyelitis or chronic fatigue syndrome
- Myalgic encephalomyelitis
- Rare and uncommon symptoms
- Symptom scales
- Stigma
- Causes of death
- Medical neglect and abuse
- Periodic paralysis
Severe ME patient groups[edit | edit source]
People with Severe or Very Severe ME[edit | edit source]
- Jodi Bassett (deceased)
- Olaf Bodden Former professional soccer player[50]
- Maeve Boothby-O'Neill (deceased)
- Emily Collingridge (deceased)
- Merryn Crofts (deceased)
- Linda Crowhurst
- Whitney Dafoe
- Lynn Gilderdale (deceased)
- Sophia Mirza (deceased)
- Jessica Taylor-Bearman
- Naomi Whittingham
- Andrew Williams (deceased)
Severe ME blogs and websites[edit | edit source]
Advocacy appeals[edit | edit source]
- Emily Collingridge severe ME Appeal 2011
- We are Failing People with Very Severe ME/CFS - Health Rising 2021
Learn more[edit | edit source]
- Comprehensive list of M.E.Symptoms[51] - Hummingbirds' Foundation for M.E.
- Knowledge in the Hope of Protecting M.E. Sufferers from Unnecessary Sectioning[52] - Preventing the unnecessary forced mental health sectioning of severely ill patients - The Grace Charity for M.E. with 25% ME Group
- My life stopped - Severe M.E. report[49] - Action for ME
- Severe M.E. symptoms[53] - 25% ME Group
- Supporting people with severe Myalgic Encephalomyelitis[54] - Greg Crowhurst
References[edit | edit source]
- ↑ Committee on the Diagnostic Criteria for Myalgic Encephalomyelitis/Chronic Fatigue Syndrome;Board on the Health of Select Populations; Institute of Medicine (U.S.) (2015). Beyond myalgic encephalomyelitis/chronic fatigue syndrome: redefining an illness. Washington, D.C.: National Academies Press. p. 32. ISBN 9780309316903. OCLC 906233426.
- ↑ "Severe M.E." 25% M.E. Group. Retrieved March 17, 2022.
- ↑ 3.0 3.1 Harris, Scott Jordan (March 30, 2012). "ME is often dismissed – but sufferers like Emily Collingridge are dying". The Guardian. Retrieved March 17, 2022.
- ↑ 4.0 4.1 Taylor, Jim (July 27, 2018). "'Vindication' for woman who wanted ME on death certificate". BBC Radio 5 Live.
- ↑ Chu, Lily; Elliott, Meghan; Stein, Eleanor; Jason, Leonard A. (2021). "Managing Suicidality in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Healthcare. 9 (6): 629. doi:10.3390/healthcare9060629. ISSN 2227-9032. PMC 8227525. PMID 34070367.
- ↑ Carruthers, Bruce M.; van de Sande, Marjorie I.; De Meirleir, Kenny L.; Klimas, Nancy G.; Broderick, Gordon; Mitchell, Terry; Staines, Donald; Powles, A.C. Peter; Speight, Nigel; Vallings, Rosamund; Bateman, Lucinda; Baumgarten-Austrheim, Barbara; Bell, David; Carlo-Stella, Nicoletta; Chia, John; Darragh, Austin; Jo, Daehyun; Lewis, Donald; Light, Alan; Marshall-Gradisnik, Sonya; Mena, Ismael; Mikovits, Judy; Miwa, Kunihisa; Murovska, Modra; Pall, Martin; Stevens, Staci (August 22, 2011). "Myalgic encephalomyelitis: International Consensus Criteria". Journal of Internal Medicine. 270 (4): 327–338. doi:10.1111/j.1365-2796.2011.02428.x. ISSN 0954-6820. PMC 3427890. PMID 21777306.
- ↑ 7.0 7.1 Committee on the Diagnostic Criteria for Myalgic Encephalomyelitis/Chronic Fatigue Syndrome;Board on the Health of Select Populations; Institute of Medicine (U.S.) (2015). "Questionnaires and Tools That May Be Useful for Assessing ME/CFS Symptoms". Beyond myalgic encephalomyelitis/chronic fatigue syndrome: redefining an illness. Washington, D.C.: National Academies Press. ISBN 9780309316903. OCLC 906233426.
- ↑ 8.0 8.1 van Campen, C. (Linda) M.C.; Rowe, Peter C.; Visser, Frans C. (June 2020). "Cerebral Blood Flow Is Reduced in Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients During Mild Orthostatic Stress Testing: An Exploratory Study at 20 Degrees of Head-Up Tilt Testing". Healthcare. 8 (2): 169. doi:10.3390/healthcare8020169. PMC 7349207. PMID 32545797.
- ↑ Shelkey, Mary; Wallace, Meredith (2012). "Katz Index of Independence in Activities of Daily Living (ADL)" (PDF).
- ↑ Graf, Carla (November 23, 2015). "The Lawton Instrumental Activities of Daily Living (IADL) Scale | ConsultGeri Assessment Tool". ConsultGeri. Retrieved October 13, 2018.
- ↑ "36-Item Short Form Survey from the RAND Medical Outcomes Study". rand.org. Retrieved October 13, 2018.
- ↑ "Work and Social Adjustment Scale" (PDF). serene.me.
- ↑ Jason, Leonard A.; Evans, Meredyth; Brown, Molly; Porter, Nicole; Brown, Abigail; Hunnell, Jessica; Anderson, Valerie; Lerch, Athena (2011). "Fatigue Scales and Chronic Fatigue Syndrome: Issues of Sensitivity and Specificity". Disability studies quarterly : DSQ. 31 (1). ISSN 1041-5718. PMC 3181109. PMID 21966179.
- ↑ 14.0 14.1 14.2 Strassheim, Victoria Jane; Sunquist, Madison; Jason, Leonard A; Newton, Julia (2018). "Defining the prevalence and symptom burden of those with self-reported severe chronic fatigue syndrome/myalgic encephalomyelitis (CFS/ME): a two-phase community pilot study in the North East of England" (PDF). BMJ open. 8 (9): e020775. doi:10.1136/bmjopen-2017-020775.
- ↑ 15.0 15.1 Strassheim, Victoria; Lambson, Rebecca; Hackett, Katie L.; Newton, Julia L. (June 19, 2017). "What is known about severe and very severe chronic fatigue syndrome? A scoping review". Fatigue: Biomedicine, Health & Behavior. 5 (3): 167–183. doi:10.1080/21641846.2017.1333185. ISSN 2164-1846.
- ↑ The Caged Bird (2016). "ME Awareness May 2016". YouTube. Let's Do It for ME. Retrieved January 28, 2019.
- ↑ 17.0 17.1 Rowe, Peter C.; Marden, Colleen L.; Heinlein, Scott; Edwards, Charles C. (February 2, 2018). "Improvement of severe myalgic encephalomyelitis/chronic fatigue syndrome symptoms following surgical treatment of cervical spinal stenosis". Journal of Translational Medicine. 16 (1): 21. doi:10.1186/s12967-018-1397-7. ISSN 1479-5876. PMC 5796598. PMID 29391028.
- ↑ Brownlie, Helen; Speight, Nigel (November 12, 2021). "Back to the Future? Immunoglobulin Therapy for Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Healthcare. 9 (11): 1546. doi:10.3390/healthcare9111546. ISSN 2227-9032. PMC 8623195. PMID 34828592.
- ↑ Baxter, Helen; Speight, Nigel; Weir, William (April 2021). "Life-Threatening Malnutrition in Very Severe ME/CFS". Healthcare. 9 (4): 459. doi:10.3390/healthcare9040459. PMC 8070213. PMID 33919671.
- ↑ Montoya, Jose; Dowell, Theresa; Mooney, Amy; Dimmock, Mary; Chu, Lily (October 6, 2021). "Caring for the Patient with Severe or Very Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Healthcare. 9 (10): 1331. doi:10.3390/healthcare9101331. ISSN 2227-9032. PMC 8544443. PMID 34683011.
- ↑ Chang, Chia-Jung; Hung, Li-Yuan; Kogelnik, Andreas M.; Kaufman, David; Aiyar, Raeka S.; Chu, Angela M.; Wilhelmy, Julie; Li, Peng; Tannenbaum, Linda (October 2021). "A Comprehensive Examination of Severely Ill ME/CFS Patients". Healthcare. 9 (10): 1290. doi:10.3390/healthcare9101290. PMC 8535418. PMID 34682970.
- ↑ Newton, Faith R. (June 2021). "The Impact of Severe ME/CFS on Student Learning and K–12 Educational Limitations". Healthcare. 9 (6): 627. doi:10.3390/healthcare9060627. PMC 8225090. PMID 34070286.
- ↑ Fennell, Patricia A.; Dorr, Nancy; George, Shane S. (May 9, 2021). "Elements of Suffering in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: The Experience of Loss, Grief, Stigma, and Trauma in the Severely and Very Severely Affected". Healthcare (Basel, Switzerland). 9 (5): 553. doi:10.3390/healthcare9050553. ISSN 2227-9032. PMC 8150911. PMID 34065069.
- ↑ Vink, Mark; Vink-Niese, Alexandra (May 27, 2021). "CFS patients remain severely disabled after specialist treatment with CBT in the UK". Journal of the Royal Society of Medicine. 114 (6): 284–284. doi:10.1177/01410768211013447. ISSN 0141-0768. PMC 8212546. PMID 34042529.
- ↑ Maksoud, Rebekah; Eaton-Fitch, Natalie; Matula, Michael; Cabanas, Hélène; Staines, Donald; Marshall-Gradisnik, Sonya (May 2021). "Systematic Review of Sleep Characteristics in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Healthcare. 9 (5): 568. doi:10.3390/healthcare9050568. PMC 8150292. PMID 34065013.
- ↑ Strassheim, Victoria; Newton, Julia L.; Collins, Tracy (February 5, 2021). "Experiences of Living with Severe Chronic Fatigue Syndrome/Myalgic Encephalomyelitis". Healthcare. 9 (2): 168. doi:10.3390/healthcare9020168. ISSN 2227-9032. PMC 7914910. PMID 33562474.
- ↑ van Campen, C (Linda) M.C.; Rowe, Peter C.; Visser, Frans C. (June 30, 2020). "Two-Day Cardiopulmonary Exercise Testing in Females with a Severe Grade of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Comparison with Patients with Mild and Moderate Disease". Healthcare. 8 (3): 192. doi:10.3390/healthcare8030192. ISSN 2227-9032. PMC 7551790. PMID 32629923.
- ↑ Speight, Nigel (September 2020). "Severe ME in Children". Healthcare. 8 (3): 211. doi:10.3390/healthcare8030211. PMC 7551866. PMID 32674263.
- ↑ van Campen, C. (Linda) MC; Rowe, Peter C.; Visser, Frans C. (October 12, 2020). "Reductions in Cerebral Blood Flow Can Be Provoked by Sitting in Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients". Healthcare. 8 (4): 394. doi:10.3390/healthcare8040394. PMC 7712289. PMID 33050553.
- ↑ Iversen, Per Ole; Lueder, Thomas Gero von; Kardel, Kristin Reimers; Lien, Katarina (December 2020). "Cardiac Dimensions and Function are Not Altered among Females with the Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Healthcare. 8 (4): 406. doi:10.3390/healthcare8040406. PMC 7712104. PMID 33081294.
- ↑ Boulazreg, Samir; Rokach, Ami (December 2020). "The Lonely, Isolating, and Alienating Implications of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Healthcare. 8 (4): 413. doi:10.3390/healthcare8040413. PMC 7711762. PMID 33092097.
- ↑ van Campen, C. (Linda) M.C.; Rowe, Peter C.; Visser, Frans C. (September 2020). "Validation of the Severity of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome by Other Measures than History: Activity Bracelet, Cardiopulmonary Exercise Testing and a Validated Activity Questionnaire: SF-36". Healthcare. 8 (3): 273. doi:10.3390/healthcare8030273. PMC 7551321. PMID 32823979.
- ↑ Kingdon, Caroline; Giotas, Dionysius; Nacul, Luis; Lacerda, Eliana (September 2020). "Health Care Responsibility and Compassion-Visiting the Housebound Patient Severely Affected by ME/CFS". Healthcare. 8 (3): 197. doi:10.3390/healthcare8030197. PMC 7551603. PMID 32635535.
- ↑ Conroy, Karl; Bhatia, Shaun; Islam, Mohammed; Jason, Leonard A. (February 2021). "Homebound versus Bedridden Status among Those with Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Healthcare. 9 (2): 106. doi:10.3390/healthcare9020106. PMC 7909520. PMID 33498489.
- ↑ Williams, Leah R.; Isaacson-Barash, Carol (February 2021). "Three Cases of Severe ME/CFS in Adults". Healthcare. 9 (2): 215. doi:10.3390/healthcare9020215. PMC 7920463. PMID 33669438.
- ↑ Dafoe, Whitney (May 2021). "Extremely Severe ME/CFS—A Personal Account". Healthcare. 9 (5): 504. doi:10.3390/healthcare9050504. PMC 8145314. PMID 33925566.
- ↑ Healthcare (2021). "Special Issue: ME/CFS ― The Severely and Very Severely Affected". Healthcare. Retrieved February 19, 2021.
- ↑ Tomas, Cara; Elson, Joanna L.; Newton, Julia L.; Strassheim, Victoria; Walker, Mark (April 10, 2020). "The effect of myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) severity on cellular bioenergetic function". PLoS ONE. 15 (4): e0231136. doi:10.1371/journal.pone.0231136.
- ↑ Strassheim, Victoria Jane; Lambson, Rebecca; Hackett, Katie; Newton, Julia L (2017). "Understanding severely affected chronic fatigue syndrome (CFS): the gravity of the situation". Physical Therapy Reviews. 22 (3–4): 197–201. doi:10.1080/10833196.2017.1327131. Retrieved October 20, 2018.
- ↑ Pendergrast, Tricia; Brown, Abigail; Sunnquist, Madison; Jantke, Rachel; Newton, Julia L; Strand, Elin Bolle; Jason, Leonard A (December 2016). "Housebound versus nonhousebound patients with myalgic encephalomyelitis and chronic fatigue syndrome". Chronic illness. 12 (4): 292–307. doi:10.1177/1742395316644770. ISSN 1742-3953. PMC 5464362. PMID 27127189.
- ↑ Mihelicova, Martina; Siegel, Zachary; Evans, Meredyth; Brown, Abigail; Jason, Leonard (December 2016). "Caring for People with Severe Myalgic Encephalomyelitis: An Interpretative Phenomenological Analysis of Parents' Experiences". Journal of health psychology. 21 (12): 2824–2837. doi:10.1177/1359105315587137. ISSN 1359-1053. PMC 4675701. PMID 26063209.
- ↑ McDermott, Clare; Al Haddabi, Atheer; Akagi, Hiroko; Selby, Michelle; Cox, Diane; Lewith, George (June 19, 2014). "What is the current NHS service provision for patients severely affected by chronic fatigue syndrome/myalgic encephalomyelitis? A national scoping exercise". BMJ Open. 4 (6): 292–307. doi:10.1136/bmjopen-2014-005083. ISSN 2044-6055. PMC 4078780. PMID 24984956.
- ↑ Wiborg, Jan F.; van der Werf, Sieberen; Prins, Judith B.; Bleijenberg, Gijs (May 2010). "Being homebound with chronic fatigue syndrome: A multidimensional comparison with outpatients". Psychiatry Research. 177 (1–2): 246–249. doi:10.1016/j.psychres.2010.02.010. ISSN 0165-1781.
- ↑ Pheby, Derek; Saffron, Lisa (2009). "Risk factors for severe ME/CFS". Biology and Medicine. 1 (4): 50–74.
- ↑ Burley, Lucy; Cox, Diane; Findley, Leslie (August 1, 2007). "Severe Chronic Fatigue Syndrome: Recovery is Possible" (PDF). British Journal of Occupational Therapy. pp. 339–344. doi:10.1177/030802260707000803. Retrieved February 11, 2019.
- ↑ Rangel, L; Garralda, M E; Levin, M; Roberts, H (2000). "The course of severe chronic fatigue syndrome in childhood" (PDF). Journal of the Royal Society of Medicine. 93 (3): 129–134. doi:10.1177/014107680009300306. PMID 10741312.
- ↑ Cox, Diane L.; Findley, Leslie J. (2000). "Severe and Very Severe Patients with Chronic Fatigue Syndrome". Journal of Chronic Fatigue Syndrome. 7 (3): 33–47. doi:10.1300/j092v07n03_04. ISSN 1057-3321.
- ↑ Rolfe, Brooke (October 16, 2018). "Woman, 33, has been living on a dementia ward for FIVE years". Mail Online. Retrieved October 17, 2018.
- ↑ 49.0 49.1 Pates, Andrew (November 14, 2014). "My life stopped..." (PDF). Action for ME.
- ↑ "Benefizspiel für den schwer kranken Olaf Bodden". Die Welt (in Deutsch). 2021. Retrieved November 17, 2021.
- ↑ Bassett, Jodi (June 2012). "The comprehensive M.E. symptom list" (PDF). The Hummingbirds' Foundation for M.E. (HFME). Retrieved December 12, 2018.
- ↑ The Grace Charity for M.E.; 25% ME Group (January 2019). "Knowledge in the Hope of Protecting M.E. Sufferers from Unnecessary Sectioning". Retrieved July 12, 2019.
- ↑ "Symptoms - 25% M.E. Group". 25% M.E. Group. Retrieved October 20, 2018.
- ↑ Crowhurst, Greg (2005). "Supporting people with severe myalgic encephalomyelitis" (PDF). ME Foreningen. Nursing Standard.

