- This page was created by volunteers like you!
- Help us make it even better. To learn more about contributing to MEpedia, click here.
- Join the movement
- Visit #MEAction to find support or take action. Donate today to help us improve and expand this project.
Gulf War Illness
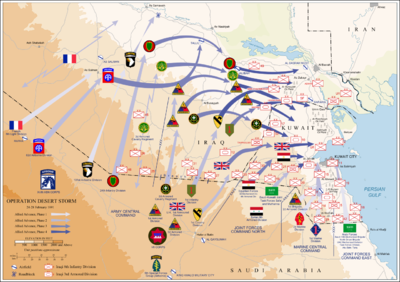
Gulf War Illness (GWI), also known as Gulf War Syndrome (GWS), is a term used for unexplained illnesses occurring in veterans of the 1991 Gulf War in Southwest Asia. According to the Institute of Medicine in 2013, about one-third of US Gulf War veterans (250,000 of 700,000 personnel) suffer from “chronic multi-symptom illness (CMI): a series of symptoms that cannot be medically explained.”[1][2] Science News summary of June 29, 2016, states: "Veterans of the Gulf War are more than twice as likely to have medically unexplained symptoms known as "multisymptom illness" (MSI), compared to Iraq/Afghanistan War veterans, according to an updated research."[3]
In a May 2022 study Robert W Haley et al.[4] have concluded that "exposure to sarin gas that occurred after coalition airplanes blew up chemical storage tanks" was the cause, and that genetic differences in the PON1 gene resulted in different risk levels to GWI.[5][4] The PON1 gene determines the genetic risk of susceptibility to organophosphate cholinesterase-inhibiting chemicals including nerve agents such as sarin.[4]
Symptoms
The U.S. Department of Veterans Affairs has a list on Gulf War Veterans' Medically Unexplained Illnesses.[6]
- Myalgic Encephalomyelitis/Chronic fatigue syndrome (ME/CFS) with long-term severe fatigue.
- Fibromyalgia characterized by chronic widespread muscle pain and may include insomnia, morning stiffness, headache, and memory problems.[6]
Functional gastrointestinal disorders
A group of conditions marked by chronic or recurrent symptoms related to any part of the gastrointestinal tract. Functional condition refers to an abnormal function of an organ, without a structural alteration in the tissues.
- functional abdominal pain syndrome
- functional dyspepsia (indigestion)
- irritable bowel syndrome[6][6]
Undiagnosed illnesses
These symptoms may be connected to undiagnosed illnesses.
- abnormal weight loss
- cardiovascular disease
- fatigue
- headache
- joint pain
- menstrual disorders
- muscle pain
- neurological and psychological problems
- respiratory disorders
- skin conditions
- sleep dysfunction[6]
Other symptoms
Multisystem condition
In March 2003, New Scientist magazine's print edition reported on Dr. Robert Haley and his team identifying three distinct syndromes in Gulf war veterans that involved brain damage.
- Syndrome 1: Symptoms are impaired cognition, distractions, and insomnia from the exposure of pesticide with basal ganglia damage.
- Syndrome 2: The symptoms are confusion, disorientation, ataxia, and vertigo due to exposure to sarin and pyridostigmine with damage to the brainstem and basal ganglia.
- Syndrome 3: Symptoms are pain, tingling, and numbness from exposure to DEET and pyridostigmine with damage to the brainstem.[7]
175,000 of 700,000 US Gulf War personnel are affected by the brain damage syndromes categorized by Dr. Haley and 75,000 are ill due to other exposures; in total 250,000 are chronically ill with GWI.[8][7][9]
Cause of illness
Causation include vaccinations; oil well fires; chemical and biological weapons; depleted uranium; noise; CARC paint used on military vehicles; occupational hazards; pyridostigmine bromide; pesticides or other organophosphates; sand, dust, and particulates; toxic embedded fragments; infectious diseases; heat injuries; fuel; decontamination solutions; and the fluoroquinolone antibiotic ciprofloxacin.[10][9][11][7]
Toxins
The conclusions and recommendations of the Gulf War Illness and the Health of Gulf War Veterans: Research Update and Recommendations, 2009-2013 report[12] conclude "exposure to pesticides and pyridostigmine bromide are causally associated with Gulf War illness" as well as other hazardous exposures including gas agents sarin/cyclosarin. "Mixed exposures include not only mixtures of chemicals but also chemicals combined with heat, dehydration, infection and other environmental stressors."[12]
A May 2022 study by Robert W Haley et al.[4] - "have concluded that "exposure to sarin gas that occurred after coalition airplanes blew up chemical storage tanks" was the cause of Gulf War Illness.[13]
Vaccinations
Mass vaccinations "against infectious diseases including medical counter-measures against biological weapons" were given prior to military deployment.[14] Vaccination in the presence of elevated cortisol levels can drive cytokine expression toward Th2 dominance.[15][16]
Comorbidities
Gulf War Illness increases the risk of developing other medical conditions. The U.S. Department of Veteran's Affairs found that "1990-1991 Gulf War deployment is associated with an increased risk for ME/CFS, fibromyalgia, skin conditions, and dyspepsia."[17]
Potential treatments
Vagus nerve stimulation has been identified as a possible treatment for GWI.[18]
Controversy
U.S. Department of Veterans Affairs' cover-up of GWI
- Aug 28, 1997, The Cover-up of Gulf War Syndrome -- A Question of Natinal Integrity[19]
- Mar 13, 2013, Whistleblower: Veterans Affairs Covered Up Data on Mental Health, Gulf War Syndrome[20]
- Mar 13, 2013, Researcher says officials covered up vets' health data[21] - USA Today
WASHINGTON — U.S. Department of Veterans Affairs officials purposely manipulate or hide data that would support the claims of veterans from Iraq and Afghanistan to prevent paying costly benefits, a former VA researcher told a House subcommittee Wednesday.
"If the studies produce results that do not support the office of public health's unwritten policy, they do not release them," said Steven Coughlin, a former epidemiologist in the VA's public health department.
"This applies to data regarding adverse health consequences of environmental exposures, such as burn pits in Iraq and Afghanistan, and toxic exposures in the Gulf War," Coughlin said. "On the rare occasions when embarrassing study results are released, data are manipulated to make them unintelligible."[21]
- Apr 12, 2013, Dr. Robert Haley, What Caused Gulf War Illness[8] (Video) Dr. Haley speaks about the United States Department of Veterans Affairs' cover-up of US Gulf War troop illness being due to environmental exposure.
- Mar 14, 2014, Congress Confronts VA Over Gulf War Illness Research[22]
- Mar 30, 2015, Former VA Chief Of Staff Linked To Gulf War Scandal[23]
Professor Simon Wessely, psychiatric paradigm researcher of chronic fatigue syndrome, believed that stress was the common denominator of GWI.
- 2004, Interview with New Scientist, US in U-turn over Gulf war syndrome[7]
Wessely told New Scientist: “There is not one single cause for the ill health,” adding that he believes we may never fully know what happened to the people who became ill.
Wessely asked both Gulf and non-Gulf veterans about 50 standard symptoms. “Gulf veterans reported every symptom twice as often,” he told the Lloyd inquiry. If there were a unique Gulf syndrome, some would be relatively more frequent in the Gulf group. “But they are just experiencing more ill health. There is no unique syndrome here.”
Wessely favours psychological explanations for Gulf war illnesses. The only thing that could have affected so many different people, he says, was stress, especially anxiety about chemical weapons, misinformation about Gulf war syndrome afterwards, and the many vaccinations Gulf troops received. His team found the more vaccine Gulf, but not non-Gulf veterans, received the more likely they are to be ill.
Haley says the questions in Wessely’s study were too vague to distinguish between a real syndrome and people who have, say, occasional dizziness or joint pain. He says this will confound efforts to uncover a meaningful pattern behind the veterans’ symptoms.[7]
- 2006, A study published in The Lancet that Wessely was involved with, The health of UK military personnel who deployed to the 2003 Iraq war: a cohort study[24] interpretation:
For regular personnel in the UK armed forces, deployment to the Iraq war has not, so far, been associated with significantly worse health outcomes, apart from a modest effect on multiple physical symptoms. There is evidence of a clinically and statistically significant effect on health in reservists.[24]
- 2006, Something old, something new, something borrowed, something blue: The true story of Gulf War Syndrome[25]
So my story then: something old, we have seen some of these before; something new, there was a definite hazard with some of the precautions that were taken to protect Gulf veterans; something borrowed, soldiers can also be civilians and the things that concern us also can concern them; something blue, the psychiatry of Gulf War is the psychiatry more of depression than it is of PTSD.[25]
- 2010, A second study What are the consequences of deployment to Iraq and Afghanistan on the mental health of the UK armed forces? A cohort study[26] interpretation:
Symptoms of common mental disorders and alcohol misuse remain the most frequently reported mental disorders in UK armed forces personnel, whereas the prevalence of probable post-traumatic stress disorder was low. These findings show the importance of continued health surveillance of UK military personnel.[26]
- 2011, Two decades on, battle goes on over 'Gulf War Syndrome'[27] - BBC News
Professor Simon Wessely is director of the King's Centre for Military Health Research in London and an adviser to the Ministry of Defence. He does not believe Gulf War Syndrome exists as a distinct illness.
Even so, he has no doubt that a significant number of Gulf veterans became ill as a direct result of their military service.
"The evidence is incontrovertible that there is a Gulf War health effect," he says.
"Something to do with the Gulf has affected health and no-one serious has ever disputed that.
"Is there a problem? Yes there is. Is it Gulf War Syndrome or isn't it? I think that's a statistical and technical question that's of minor interest."
The Ministry of Defence echoes Professor Wessely's view.[27]
News articles and interviews
- 2022, Researchers Think They've Found the Cause of Gulf War Illness - Military.com
- 2013, Researcher says officials covered up vets' health data - USA Today
- 2011, Two decades on, battle goes on over 'Gulf War Syndrome' - BBC News
- 2004, US in U-turn over Gulf war syndrome - New Scientist
Notable studies
- 2015, Cytokine expression provides clues to the pathophysiology of Gulf War illness and myalgic encephalomyelitis[28] - (Full text)
- 2017, Role of mitochondrial DNA damage and dysfunction in veterans with Gulf War Illness[29] - (Full Text)
- 2018, The Multiple Hit Hypothesis for Gulf War Illness: Self-Reported Chemical/Biological Weapons Exposure and Mild Traumatic Brain Injury[31] - (Full Text)
- 2018, Fatigue in Gulf War Illness is associated with tonically high activation in the executive control network[32] - (Full Text)
- 2018, Gulf War agents pyridostigmine bromide and permethrin cause hypersensitive nociception that is restored after vagus nerve stimulation[33] - (Full text)
- 2019, Gastrointestinal neuroimmune disruption in a mouse model of Gulf War illness[34] - (Full text)
- GI neuroimmune disruption contributes to Gulf War Illness
Many Persian Gulf War veterans experience Gulf War Illness (GWI), a chronic condition with symptoms ranging from gastrointestinal to neurological. While exposure to the anti-nerve gas pyridostigmine bromide (PB) is linked to the development of GWI, the exact cause and mechanisms of the illness remain unclear. Recently, an animal study tested the hypothesis that exposure to PB contributes to the development of GWI by disrupting the neural and immune systems of the intestine.[35]
- GI neuroimmune disruption contributes to Gulf War Illness
- 2020, In-vivo imaging of neuroinflammation in veterans with Gulf War illness[36] - (Full text)
- 2020, Acetylcholinesterase inhibitor exposures as an initiating factor in the development of Gulf War Illness, a chronic neuroimmune disorder in deployed veterans[37] - (Full text)
- 2020, Exercise alters brain activation in Gulf War Illness and Myalgic Encephalomyelitis/Chronic Fatigue Syndrome[38] - (Full text)
- 2021, Exposure to Gulf War Illness-related agents leads to the development of chronic pain and fatigue[39] - (Full text)
- 2021, Vagal nerve stimulation as a possible non-invasive treatment for chronic widespread pain in Gulf Veterans with Gulf War Illness[18] - (Full text)
- 2021, Pyridostigmine bromide, chlorpyrifos, and DEET combined Gulf War exposure insult depresses mitochondrial function in neuroblastoma cells[40] - (Full text)
- 2022, Evaluation of a Gene-Environment Interaction of PON1 and Low-Level Nerve Agent Exposure with Gulf War Illness: A Prevalence Case-Control Study Drawn from the U.S. Military Health Survey's National Population Sample[4] - (Full Text)
See also
- Vagal nerve stimulation
- Organophosphate
- Mestinon (pyridostigmine bromide)
- Vaccine
Learn more
- 2019, Veterans Study Suggests Two Subtypes of Gulf War Illness - Georgetown University Medical Center
- 2019, Brain studies show chronic fatigue syndrome and Gulf War illness are distinct conditions
- 2016, Testing nine potential treatments for Gulf War Illness pain and fatigue - Jarred Younger
- 2015, GULF WAR RESEARCH STRATEGIC PLAN 2013-2017[41]
- 2014, Gulf War Illness and the Health of Gulf War Veterans: Research Update and Recommendations, 2009-2013
- 2014, Advisory Group: Exposures, Not Stress Caused Gulf War Illness - U.S. Medicine
- 2008, Gulf War Illness and the Health of Gulf War Veterans Scientific Findings and Recommendations - Research Advisory Committee on Gulf War Veterans' llnesses
- 2004, Independent Public Inquiry on Gulf War Illnesses - The Lloyd Inquiry (Report Resume)
References
- ↑ "Gulf War Syndrome". Johns Hopkins Medicine Health Library. Retrieved August 24, 2018.
- ↑ Stencel, Christine (April 9, 2010). "Gulf War Service Linked to Post-Traumatic Stress Disorder, Multisymptom Illness, Other Health Problems, But Causes Are Unclear". The National Academies of Science Engineering Medicine. Retrieved August 26, 2018.
- ↑ https://journals.lww.com/joem/Abstract/2016/07000/Multisymptom_Illness_in_Gulf_War_Veterans__A.3.aspx
- ↑ 4.0 4.1 4.2 4.3 4.4 Haley, Robert W.; Kramer, Gerald; Xiao, Junhui; Dever, Jill A.; Teiber, John F. (May 2022). "Evaluation of a Gene-Environment Interaction of PON1 and Low-Level Nerve Agent Exposure with Gulf War Illness: A Prevalence Case-Control Study Drawn from the U.S. Military Health Survey's National Population Sample". Environmental Health Perspectives. 130 (5): 57001. doi:10.1289/EHP9009. ISSN 1552-9924. PMC 9093163. PMID 35543525.
- ↑ Johnson, Cort (May 21, 2022). "The Gulf War Illness Breakthrough and why it Matters to ME/CFS/FM and long COVID". Health Rising. Retrieved June 9, 2022.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 "Gulf War Veterans' Medically Unexplained Illnesses - Public Health". U.S. Department of Veterans Affairs, Veterans Health Administration. Retrieved August 24, 2018.
- ↑ 7.0 7.1 7.2 7.3 7.4 MacKenzie, Deborah (November 3, 2004). "US in U-turn over Gulf war syndrome". New Scientist. Retrieved August 26, 2018.
- ↑ 8.0 8.1 Haley, Robert (May 6, 2013). "Dr. Robert Haley, What Caused Gulf War Illness". YouTube. David Spencer.
- ↑ 9.0 9.1 "Gulf War Exposures". U.S. Department of Veterans Affairs, Veterans Health Administration. Retrieved August 26, 2018.
- ↑ "New FDA warnings on Cipro may tie into Gulf War illness". Military Times. August 8, 2017. Retrieved September 13, 2020.
- ↑ Hogg, Matthew (June 8, 2017). "Gulf War Syndrome - Overview, Symptoms & Possible Causes". EI Resource. Retrieved August 26, 2018.
- ↑ 12.0 12.1 Research Advisory Committee on Gulf War Veterans' Illnesses (May 2014). "Gulf War Illness and the Health of Gulf War Veterans: Research Update and Recommendations, 2009-2013: Updated Scientific Findings and Recommendations" (PDF). Washington,D.C.: U.S. Government Printing Office. p. 60.
- ↑ Johnson, Cort (May 21, 2022). "The Gulf War Illness Breakthrough and why it Matters to ME/CFS/FM and long COVID". Health Rising. Retrieved June 9, 2022.
- ↑ Peakman, Mark; Skowera, Ania; Hotopf, Matthew (2006), "Immunological dysfunction, vaccination and Gulf War illness", Philosophical Transactions of the Royal Society B: Biological Sciences, 361 (1468): 681–687, doi:10.1098/rstb.2006.1826
- ↑ Bernton, E.; Hoover, D.; Galloway, R.; Popp, K. (December 29, 1995). "Adaptation to chronic stress in military trainees. Adrenal androgens, testosterone, glucocorticoids, IGF-1, and immune function". Annals of the New York Academy of Sciences. 774: 217–231. ISSN 0077-8923. PMID 8597461.
- ↑ Ramírez, F.; Fowell, D.J.; Puklavec, M.; Simmonds, S.; Mason, D. (April 1, 1996). "Glucocorticoids promote a TH2 cytokine response by CD4+ T cells in vitro". Journal of Immunology. 156 (7): 2406–2412. ISSN 0022-1767. PMID 8786298.
- ↑ "Myalgic Encephalomyelitis/Chronic Fatigue Syndrome in Gulf War Veterans - Public Health". U.S. Department of Veterans Affairs, Veterans Health Administration. Retrieved August 24, 2018.
- ↑ 18.0 18.1 Natelson, Benjamin H.; Stegner, Aaron J.; Lange, Gudrun; Khan, Sarah; Blate, Michelle; Sotolongo, Anays; DeLuca, Michelle; Van Doren, William W.; Helmer, Drew A. (October 1, 2021). "Vagal nerve stimulation as a possible non-invasive treatment for chronic widespread pain in Gulf Veterans with Gulf War Illness". Life Sciences. 282: 119805. doi:10.1016/j.lfs.2021.119805. ISSN 0024-3205.
- ↑ Harrison III, H. Lindsey (August 28, 1997). "The Cover-Up of Gulf War Syndrome -- A Question of National Integrity". gulfwarvets.com. Retrieved August 26, 2018.
- ↑ Reno, Jamie (March 13, 2013). "Whistleblower: Veterans Affairs Covered Up Data on Mental Health, Gulf War Syndrome". gulfwarvets.com. Retrieved August 26, 2018.
- ↑ 21.0 21.1 Kennedy, Kelly (March 13, 2013). "Researcher says officials covered up vets' health data". USA TODAY. Retrieved August 26, 2018.
- ↑ Ruiz, Rebecca (March 24, 2014). "Congress Confronts VA Over Gulf War Illness Research". Forbes. Retrieved August 26, 2018.
- ↑ Krause, Benjamin (March 30, 2015). "Former VA Chief Of Staff Linked To Gulf War Scandal". DisabledVeterans.Org. Retrieved August 26, 2018.
- ↑ 24.0 24.1 Hotopf, Matthew; Hull, Lisa; Fear, Nicola T; Browne, Tess; Horn, Oded; Iversen, Amy; Jones, Margaret; Murphy, Dominic; Bland, Duncan (2006). Earnshaw, Mark; Greenberg, Neil; Hacker Hughes, Jamie; Tate, Rosemary; Dandeker, Christopher; Rona, Robert; Wessely, Simon. "The health of UK military personnel who deployed to the 2003 Iraq war: a cohort study". The Lancet. 367 (9524): 1731–1741. doi:10.1016/S0140-6736(06)68662-5. ISSN 0140-6736.
- ↑ 25.0 25.1 "Something old, something new, something borrowed, something blue: The true story of Gulf War Syndrome". Gresham College. Retrieved August 29, 2018.
- ↑ 26.0 26.1 Fear, Nicola T; Jones, Margaret; Murphy, Dominic; Hull, Lisa; Civerson, Amy; Coker, Bolaji; Machell, Louise; Sundin, Josefin; Woodhead, Charlotte (2010). "What are the consequences of deployment to Iraq and Afghanistan on the mental health of the UK armed forces?: A cohort study" (PDF). kcl.ac.uk (PDF). Jones, Norman; Greenberg, Neil; Landau, Sabine; Dandeker, Christopher; Rona, Roberta J; Hotopf, Mathew; Wessely, Simon.
- ↑ 27.0 27.1 Hughes, Caroline Hawley and Stuart (2011). "Battle continues over Gulf War Syndrome". BBC News. Retrieved August 26, 2018.
- ↑ Khaiboullina, Svetlana F.; DeMeirleir, Kenny L.; Rawat, Shanti; Berk, Grady S.; Gaynor-Berk, Rory S.; Mijatovic, Tatjana; Blatt, Natalia; Rizvanov, Albert A.; Young, Sheila G.; Lombardi, Vincent C. (March 1, 2015). "Cytokine expression provides clues to the pathophysiology of Gulf War illness and myalgic encephalomyelitis". Cytokine. 72 (1): 1–8. doi:10.1016/j.cyto.2014.11.019. ISSN 1043-4666. PMC 4410698.
- ↑ Falvo, Michael; Meyer, Joel; Hill, Helene Z.; Lange, Gudrun; Condon, Michael; Klein, Jacquelyn C.; Ndirangu, Duncan; Falvo, Michael J. (2017). "Role of mitochondrial DNA damage and dysfunction in veterans with Gulf War Illness". PLoS One. 12 (9): e0184832. doi:10.1371/journal.pone.0184832. PMC 5599026. PMID 28910366.
- ↑ Richman, Mike (October 19, 2017). "Researchers find evidence of DNA damage in Vets with Gulf War illness". U.S. Department of Veterans Affairs. Retrieved August 26, 2018.
- ↑ Janulewicz, Patricia; Krengel, Maxine; Quinn, Emily; Heeren, Timothy; Toomey, Rosemary; Killiany, Ronald; Zundel, Clara; Ajama, Joy; O'Callaghan, James (November 2018). "The Multiple Hit Hypothesis for Gulf War Illness: Self-Reported Chemical/Biological Weapons Exposure and Mild Traumatic Brain Injury". Brain Sciences. 8 (11): 198. doi:10.3390/brainsci8110198.
- ↑ Wylie, Glenn; Genova, Helen; Dobryakova, Ekaterina; DeLuca, John; Chiaravalloti, Nancy; Falvo, Michael; Cook, Dane (December 11, 2018). "Fatigue in Gulf War Illness is associated with tonically high activation in the executive control network". NeuroImage: Clinical: 101641. doi:10.1016/j.nicl.2018.101641. ISSN 2213-1582.
- ↑ Institute of Medicine (US) Committee on Health Effects Associated with Exposures During the Gulf War; Fulco, Carolyn E.; Liverman, Catharyn T.; Sox, Harold C. (2000). Pyridostigmine Bromide. National Academies Press (US).
- ↑ Hernandez, Siomara; Fried, David E.; Grubišić, Vladimir; McClain, Jonathon L.; Gulbransen, BrianD. (February 21, 2019). "Gastrointestinal neuroimmune disruption in a mouse model of Gulf War illness". The FASEB Journal. 33 (5): 6168–6184. doi:10.1096/fj.201802572R. ISSN 0892-6638.
- ↑ "GI neuroimmune disruption contributes to Gulf War Illness: Mouse model points to gastrointestinal neuroimmune disruption as contributing mechanism of Gulf War Illness". Retrieved February 22, 2019 – via Science Daily for Federation of American Societies for Experimental Biology.
- ↑ Alshelh, Zeynab; Albrecht, Daniel S.; Bergan, Courtney; Akeju, Oluwaseun; Clauw, Daniel J.; Conboy, Lisa; Edwards, Robert R.; Kim, Minhae; Lee, Yvonne C.; Protsenko, Ekaterina; Napadow, Vitaly; Sullivan, Kimberly; Loggia, Marco F. (February 4, 2020). "In-vivo imaging of neuroinflammation in veterans with Gulf War illness". Brain, Behavior, and Immunity. doi:10.1016/j.bbi.2020.01.020. ISSN 0889-1591.
- ↑ Michalovicz, Lindsay T.; Kelly, Kimberly A.; Sullivan, Kimberly; O'Callaghan, James P. (July 2020). "Acetylcholinesterase inhibitor exposures as an initiating factor in the development of Gulf War Illness, a chronic neuroimmune disorder in deployed veterans". Neuropharmacology. 171: 108073. doi:10.1016/j.neuropharm.2020.108073. ISSN 0028-3908. PMC 7398580. PMID 32247728.
- ↑ Washington, StuartD.; Rayhan, Rakib U.; Garner, Richard; Provenzano, Destie; Zajur, Kristina; Addiego, Florencia Martinez; VanMeter, John W.; Baraniuk, James N. (July 1, 2020). "Exercise alters brain activation in Gulf War Illness and Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Brain Communications. 2 (2). doi:10.1093/braincomms/fcaa070.
- ↑ Nguyen, Huy; Sahbaie, Peyman; Goba, Lihle; Sul, Julian; Suzaki, Aoi; Clark, J. David; Huang, Ting-Ting (October 15, 2021). "Exposure to Gulf War Illness-related agents leads to the development of chronic pain and fatigue". Life Sciences. 283: 119867. doi:10.1016/j.lfs.2021.119867. ISSN 0024-3205.
- ↑ Delic, Vedad; Karp, Joshua; Klein, Julian; Stalnaker, Katherine J.; Murray, Kathleen E.; Ratliff, Whitney A.; Myers, Catherine E.; Beck, KevinD.; Citron, Bruce A. (December 2021). "Pyridostigmine bromide, chlorpyrifos, and DEET combined Gulf War exposure insult depresses mitochondrial function in neuroblastoma cells". Journal of Biochemical and Molecular Toxicology. 35 (12). doi:10.1002/jbt.22913. ISSN 1095-6670. PMC 8678325. PMID 34528356.
- ↑ "GULF WAR RESEARCH STRATEGIC PLAN 2013-2017 - 2015 Update" (PDF). U.S. Department of Veterans Affairs. 2015.

