Pushing through symptoms
Many ME/CFS patients attempt to "push through" symptoms by ignoring them and trying to do their usual activities when they first become ill with ME/CFS[1][2] - but people with ME/CFS find that exceeding their available energy - their "energy envelope" - causes post-exertional malaise, making their health much worse.[2][3] This post-exertional malaise or post-exertional symptom exacerbation is a mandatory symptom of ME/CFS but is not usually found in other illnesses that can cause chronic fatigue.[4][3]
Effects
If a person with ME/CFS does manage to push through their symptoms and exceeds their "energy limit," the result is a delayed onset of post-exertional symptoms, better known as post-exertional malaise, which can begin be delayed from between 24 hours to 3 days after over-exerting - the prolonged recovery time is usually over 24 hours, making it impossible for patients to consistently push through their symptoms without a significant, and longer, crash.[5]
Saunders (2020) states that anyone whose symptoms are not made worse by "pushing through" fatigue and other symptoms by definition does not have ME/CFS.[2]
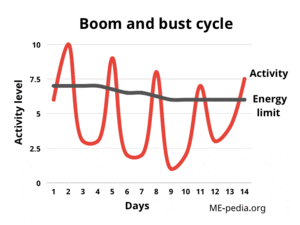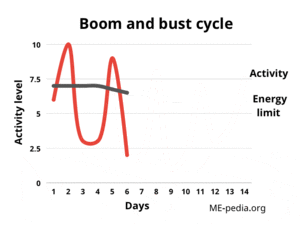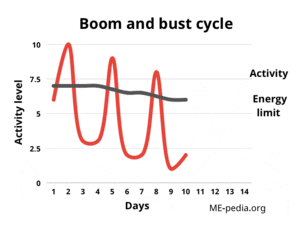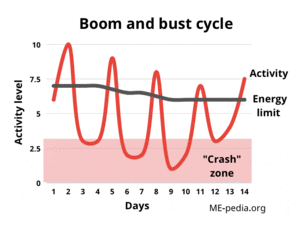
Boom and bust
When they become worse after pushing through their symptoms, people with ME/CFS then have to choose again between rest or trying again to "push through" - which causes them to deteriorate further, until eventually they physically cannot continue. Both resting and pushing through result in an "greatly lowered ability to do activities that were usual before the illness", a symptom that is required for the diagnosis of ME/CFS.[3][6]
The cycle of repeatedly exceeding energy limits by doing too much activity followed by being forced to totally stop has been referred to as the "boom and bust cycle", and is very widely recognized in ME/CFS, and in some patients without post-exertional malaise, including chronic pain and chronic fatigue patients.[7] A significant proportion of people with Long COVID report experiencing post-exertional malaise and find they have a boom and bust cycle as a result.[8]
Pacing as an alternative
The main alternative to pushing through symptoms in ME/CFS is activity pacing. Pacing or "energy management" is a way of planning and monitoring activity to try to avoid exceeding energy limits, in order to avoid the resulting periods of post-exertional malaise, which often involves patients being forced to spend days in bed recovering.[4][5]
Inability to push through
Some ME/CFS patients find themselves totally unable to push through their symptoms, the intensity of the symptoms becomes too severe, and this is not necessarily limited to severe ME/CFS patients. Professor Malcolm Hooper describes British politician Brynmor John's experience of ME/CFS:
"On 13th December 1988 Brynmor John MP died from ME/CFS. His experience of the illness was all too familiar:
Though there is only a slight gradient from our house to the main road, it could have been the North face of the Eiger. I just could not get up it.
— Magical Medicine: How to make a disease disappear (2010)
"He found himself unable to dress; the slightest exertion exhausted him and it took days to regain his strength. He was irritated by the profusion of psychiatric comment and was trying to ensure better understanding of ME/CFS (Perspectives, Summer 1991:28‐30). Brynmor John suddenly collapsed and died as he was leaving the UK Parliament's House of Commons gym after having been advised to exercise back to fitness."[9][10]
CBT and GET
Cognitive behavioral therapy (CBT) and graded exercise therapy (GET) for ME/CFS both encourage people to push through symptoms. In CBT patients are encouraged to view the fact that ME/CFS is a serious, physical illness - as the Institute of Medicine (2015) states it is - as an "illness belief" to be challenged rather than a scientific fact.[11][12] In CBT patients are expected to set "realistic" goals for what they would like to achieve and work towards those goals[13] - but with no biomarker or physical way to measure symptoms,[14][11] patients are unaware of the severity of their illness - they may be working towards goals that are actually not simply unrealistic but impossible. Patients may be told that they have a maladaptive fear of or avoidance of exertion that is causing them to reduce their activities,[14] and causing reversible deconditioning,[14] but scientific research shows that people cannot push through their symptoms on consecutive days - the post-exertional malaise caused by ME/CFS prevents this. Patients in the UK completing CBT for ME/CFS based on this biopsychosocial model were found to remain "severely disabled".[15]
In graded exercise therapy (GET) ME/CFS patients are expected to commit to very gradually increasing their activity levels, and are told to "push through" regardless of how much their symptoms worsen - they are told increases in symptoms are temporary but evidence shows this is a false assumption. A very large survey of UK patients found this GET approach caused most people to become more ill.[16]
Evidence
Trying to "push through" symptoms or "keep going" is a common response when people with ME/CFS feel pressured to continue working or continue their usual activities - but ME/CFS then causes symptoms to get far worse, this post-exertional symptom exacerbation and post-exertional malaise is the hallmark symptom of ME/CFS.[12]
Patients with severe ME - which means that they either almost fully housebound or may be bedbound - report being encouraged to "push through" or "keep going" - even after they became worse.[12]
Patients who are working when they fall ill with ME/CFS find that pushing they causes longer sickness absences from work, and any recovery is slowed down.[1]
People with ME/CFS often feel under pressure to continue working when they first become ill or when their symptoms worsen. Unfortunately, trying to push through this illness is counterproductive, potentially causing longer sickness absences and slower recovery. — Vink and Vink-Niese (2019)[1]
"Even though she feels very unwell, she tries to ignore or “push through” her symptoms, to push them out of her consciousness, and to continue her regular activities.
Eventually, however, Elizabeth’s exhaustion, increased muscle pain, and headaches make it impossible for her to ignore her symptoms; she has trouble climbing the few steps into her front door."
In a survey asking over 1,100 people with ME/CFS or fibromyalgia what they wish they had dond differently, "listened to my body more / stopped pushing so much" was the most common response, chosen by 78% of the group, and "been more careful not to overdo when I had good moments" was the second most common response.[17]
Clinicians
Pushing through symptoms is strongly advised against by clinicians, regardless of which alternative treatments they recommend instead.[6][4]
Risks and safety
Pushing through ME/CFS symptoms is widely recognized as harmful, and in some cases leads to long-term or permanent increase in symptoms which do not resolve when the patient stops attempting to push through. Many patients report developing severe ME/CFS after pushing through symptoms of mild or moderate ME/CFS.
Costs and availability
Free and available to all.
Notable studies
- 2016, Cognitive behavioural therapy in the treatment of chronic fatigue syndrome: A narrative review on efficacy and informed consent[14] - (Full text)
- 2019, Why Graded Exercise Therapy and Cognitive Behaviour Therapy are Controversial in Chronic Fatigue Syndrome[18]
- 2020, Could Cognitive Behavioural Therapy Be an Effective Treatment for Long COVID and Post COVID-19 Fatigue Syndrome? Lessons from the Qure Study for Q-Fever Fatigue Syndrome[13] - (Full text)
- 2021, Experiences of Living with Severe Chronic Fatigue Syndrome/Myalgic Encephalomyelitis[12] - (Full text)
- 2021, Elements of Suffering in Myalgic Encephalomyelitis /Chronic Fatigue Syndrome: The Experience of Loss, Grief, Stigma, and Trauma in the Severely and Very Severely Affected[19] - (Full text)
- 2021, CFS patients remain severely disabled after specialist treatment with CBT in the UK[15] - (Full text)
See also
Learn more
References
- ↑ 1.0 1.1 1.2 Vink, Mark; Vink-Niese, Alexandra (September 20, 2019). "Work Rehabilitation and Medical Retirement for Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients. A Review and Appraisal of Diagnostic Strategies". Diagnostics. 9 (4): 124. doi:10.3390/diagnostics9040124. ISSN 2075-4418.
- ↑ 2.0 2.1 2.2 Vink, Mark; Vink-Niese, Alexandra (January 28, 2021). "The draft updated NICE guidance for ME/CFS highlights the unreliability of subjective outcome measures in non-blinded trials". Journal of Health Psychology. 27 (1): 9–12. doi:10.1177/1359105321990810. ISSN 1359-1053.
- ↑ 3.0 3.1 3.2 "Symptoms | Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Centers for Disease Control and Prevention. January 27, 2021. Retrieved February 25, 2021.
- ↑ 4.0 4.1 4.2 Carruthers, BM; van de Sande, MI; De Meirleir, KL; Klimas, NG; Broderick, G; Mitchell, T; Staines, D; Powles, ACP; Speight, N; Vallings, R; Bateman, L; Bell, DS; Carlo-Stella, N; Chia, J; Darragh, A; Gerken, A; Jo, D; Lewis, DP; Light, AR; Light, KC; Marshall-Gradisnik, S; McLaren-Howard, J; Mena, I; Miwa, K; Murovska, M; Stevens, SR (2012), Myalgic encephalomyelitis: Adult & Paediatric: International Consensus Primer for Medical Practitioners (PDF), ISBN 978-0-9739335-3-6
- ↑ 5.0 5.1 Carruthers, Bruce M.; Jain, Anil Kumar; De Meirleir, Kenny L.; Peterson, Daniel L.; Klimas, Nancy G.; Lerner, A. Martin; Bested, Alison C.; Flor-Henry, Pierre; Joshi, Pradip; Powles, AC Peter; Sherkey, Jeffrey A.; van de Sande, Marjorie I. (2003). "Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Clinical Working Case Definition, Diagnostic and Treatment Protocols" (PDF). Journal of Chronic Fatigue Syndrome. 11 (2): 7–115. doi:10.1300/J092v11n01_02.
- ↑ 6.0 6.1 NICE Guideline Development Group (October 29, 2021). "Myalgic Encephalomyelitis (or Encephalopathy)/Chronic Fatigue Syndrome:diagnosis and management. NICE guideline". National Institute for Health and Care Excellence.
- ↑ Antcliff, Deborah; Keenan, Anne-Maree; Keeley, Philip; Woby, Steve; McGowan, Linda. ""Pacing does help you get your life back": The acceptability of a newly developed activity pacing framework for chronic pain/fatigue". Musculoskeletal Care. n/a (n/a). doi:10.1002/msc.1557. ISSN 1557-0681.
- ↑ Horton, Simon MC; Poland, Fiona; Kale, Swati; de Lourdes Drachler, Maria; de Carvalho Leite, Jose Carlos; McArthur, Maggie A.; Campion, Peter D.; Pheby, Derek; Nacul, Luis (November 15, 2010). "Chronic fatigue syndrome/myalgic encephalomyelitis (CFS/ME) in adults: a qualitative study of perspectives from professional practice". BMC Family Practice. 11 (1): 89. doi:10.1186/1471-2296-11-89. ISSN 1471-2296. PMC 2994803. PMID 21078171.
- ↑ Hooper, Malcolm; Williams, Margaret (Spring 2010), Magical Medicine: How to make a disease disappear (PDF)
- ↑ Price, Adam (September 2012). "We are the ones we have been waiting for". In Osmond, John; Finch, Peter (eds.). 25/25 Vision: Welsh Horizons Across 50 Years (PDF). Institute of Welsh Affairs. pp. 108–109.
The Pontypridd by-election, following the death from exhaustion of Brynmor John was held on 23 February that year.
- ↑ 11.0 11.1 Institute of Medicine (2015). Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Redefining an Illness. Washington, DC: The National Academies Press. doi:10.17226/19012. ISBN 0309316898. PMID 25695122.
- ↑ 12.0 12.1 12.2 12.3 Strassheim, Victoria; Newton, Julia L.; Collins, Tracy (February 5, 2021). "Experiences of Living with Severe Chronic Fatigue Syndrome/Myalgic Encephalomyelitis". Healthcare. 9 (2): 168. doi:10.3390/healthcare9020168. ISSN 2227-9032. PMC 7914910. PMID 33562474.
- ↑ 13.0 13.1 Vink, Mark; Vink-Niese, Alexandra (December 11, 2020). "Could Cognitive Behavioural Therapy Be an Effective Treatment for Long COVID and Post COVID-19 Fatigue Syndrome? Lessons from the Qure Study for Q-Fever Fatigue Syndrome". Healthcare. 8 (4): 552. doi:10.3390/healthcare8040552. ISSN 2227-9032. PMC 7764131. PMID 33322316.
- ↑ 14.0 14.1 14.2 14.3 Geraghty, Keith J; Blease, Charlotte (September 15, 2016). "Cognitive behavioural therapy in the treatment of chronic fatigue syndrome: A narrative review on efficacy and informed consent" (PDF). Journal of Health Psychology. 23 (1): 127–138. doi:10.1177/1359105316667798. ISSN 1359-1053.
- ↑ 15.0 15.1 Vink, Mark; Vink-Niese, Alexandra (May 27, 2021). "CFS patients remain severely disabled after specialist treatment with CBT in the UK". Journal of the Royal Society of Medicine. 114 (6): 284–284. doi:10.1177/01410768211013447. ISSN 0141-0768. PMC 8212546. PMID 34042529.
- ↑ Oxford Clinical Allied Technology and Trials Services Unit (OxCATTS) (February 27, 2019). "Evaluation of a survey exploring the experiences of adults and children with ME/CFS who have participated in CBT and GET interventional programmes. FINAL REPORT" (PDF).
- ↑ Johnson, Cort (June 23, 2019). "The ME/CFS and Fibromyalgia "What Would You Have Done Differently" Survey". Health Rising.
- ↑ Michiel, Tack (July 4, 2019). "Why Graded Exercise Therapy and Cognitive Behaviour Therapy are Controversial in Chronic Fatigue Syndrome". BMJ Medical Humanities Blog. Retrieved July 9, 2019.
- ↑ Fennell, Patricia A.; Dorr, Nancy; George, Shane S. (May 9, 2021). "Elements of Suffering in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: The Experience of Loss, Grief, Stigma, and Trauma in the Severely and Very Severely Affected". Healthcare (Basel, Switzerland). 9 (5): 553. doi:10.3390/healthcare9050553. ISSN 2227-9032. PMC 8150911. PMID 34065069.

