- This page was created by volunteers like you!
- Help us make it even better. To learn more about contributing to MEpedia, click here.
- Join the movement
- Visit #MEAction to find support or take action. Donate today to help us improve and expand this project.
Pain killers
Analgesic is a general name for types of painkillers that do not cause unconsciousness.[1] A large variety of analgesics are used in ME/CFS to help relieve both chronic and acute pain. They are also used to treat pain associated with comorbid illnesses such as IBS or fibromyalgia.[2][3][4]
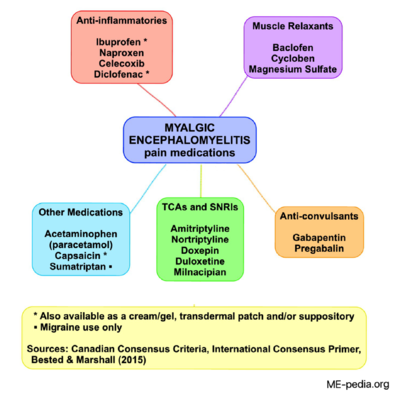
Analgesics act in a variety of ways on the peripheral and central nervous systems and can be taken in combination or alone.
Determining which analgesic is appropriate involves considering both the severity and type of pain presented. The patient's response to previous analgesics may also be considered.
Types of Painkillers
Acetaminophen
Acetaminophen, also known as paracetamol or Tylenol, is used to treat mild to moderate pain and fever. It is classed as a mild analgesic and does not reduce inflammation.[5] Acetaminophen can be taken by mouth (tablets or liquid), rectally (as suppositories), or intravenously, and is typically taken every four and six hours as needed.[6] Extended release acetaminophen can be taken every 8 hours.[7] Typical uses include headaches, muscle aches, colds and sore throats, back pain, toothaches), and to reduce fever. It is usually available over-the-counter without a prescription. Taking too much acetaminophen, or taking more than one product containing it can cause severe liver damage or death.[6][7]
Some pain medications combine acetaminophen with other drugs, for instance with NSAIDs (Anacin, Excedrin), or opioids (Hycet, Percocet, co-codamol), for stronger pain relief.[5][7]
Acetaminophen for pain in M.E.
Acetaminophen can be used as a baseline drug for pain; it has a weak effect but few side effects.[2]
NSAIDs
Nonsteroidal anti-imflammatory drugs are a class of drugs which provide both analgesic (pain-killing) and antipyretic (fever-reducing) effects, and anti-inflammatory effects in higher doses. They range from mild to strong pain relief.[3]
Commonly used NSAIDs include aspirin, ibuprofen, naproxen, diclofenac, celecoxib, meloxicam, mefenamic acid, and nabumetone.
COX-2 inhibitors
COX-2 inhibitors are NSAIDs that directly target cyclooxygenase-2 (COX-2), an enzyme responsible for inflammation and pain. Some COX-2 inhibitors used in ME/CFS include celecoxib and meloxicam.
NSAIDs for pain in M.E.
Ibuprofen, naproxen, and celecoxib, a COX-2 inhibitor. Ketorolac is a NSAID which can be used for up to 5 days, for example after surgery, and is available as tablets, by intramuscular injection or IV.[8][9]
Opioids
Opioids are drugs that bind to opioid receptors to produce morphine-like effects.[10] They provide moderate to very strong pain relief. Some of these are codeine, tramadol, oxycodone, vicodin, hydrocodone, fentanyl and morphine. Opioids are available in many different forms including tablets, slow-release tablets and patches.[11] Opioids rarely result in addiction when taken by people in pain, but they can become less effective over time (opioid tolerance), dependency may develop, and withdrawal effects can occur when opiods are stopped or doses are decreased.[11] Some side effects of opioids can be serious, initial use can cause sleepiness, dizziness, nausea and affect driving; long term use of opioids can cause breathing problems at night and weight gain.[11]
A number of different opioids may be used in patients with ME/CFS, if pain is particularly severe.[12][3]
Opioids for pain in ME/CFS
The International Consensus Criteria Primer for physicians and Canadian Consensus Criteria both state that opioids should only be used for severe pain, and with a management plan in place. No particular opioids are suggested.[3][8]
Tricyclic Antidepressants
Tricyclic antidepressant (TCAs) are a group of medications which are licensed for many different conditions besides depression, including chronic myofascial pain, dysautonomia (amitriptyline, nortriptyline, desipramine), long-term pain (amitriptyline, nortriptyline, imipramine), fibromyalgia (amitriptyline), Irritable Bowel Syndrome (amitriptyline, nortriptyline, doxepin, and others), migraine prevention (amitriptyline, nortriptyline), neuralgia (nerve pain), and sleep paralysis.[13] TCAs include amitriptyline, nortriptyline or clomipramine are commonly used in ME/CFS to treat chronic pain and to aid regular sleep.
TCAs for pain in M.E.
Most patients with M.E. are extremely sensitive to medication; the International Consensus Primer for Medical Practitioners recommends starting with a lower initial dose of TCAs, and that they should be used short term only.[3][8] There is evidence that amitriptyline, nortriptyline and doxepin are effective for pain caused by M.E.; like all TCAs benefits may not take effect for 2 to 4 weeks[8] The sedating effects of doxepin and amitriptyline may help patients with sleep problems remain asleep.[8] Side effects may be severe, and include morning or daytime sleepiness, dry mouth, weight gain, and increase dizziness and orthostatic intolerance.[13][8] Amitriptyline may also cause cognitive dysfunction, e.g. brain fog.[8] Nortriptyline causes the least side effects, and amitriptyline is particularly effective for people with fibromyalgia.[8] Some guidance states these drugs should be avoided in overweight patients with ME.[3]
Anticonvulsants
Anticonvulsants are a group of medications that were originally used in the treatment of epileptic seizures, but are increasingly used for other purposes, including the treatment of nerve pain.[14] Anticonvulsants commonly used for pain in ME/CFS include GABA analogs such as gabapentin (Neurontin) and pregabalin (Lyrica), and fatty acids such as tiagabine (Gabitril).
Anticonvulsants for pain in M.E.
Medical marijuana
Medical marijuana (cannabis designed for medical use) is available in various forms is increasingly used to treat chronic pain, including neuropathic pain.[15] CBD oil, made from marijuana or hemp, is also gaining popularity as an analgesic.[citation needed]
CBD oil, which can be made from hemp is an alternative that is legal everywhere, and cannot create a high.[citation needed]
Medical marijuana and CBD oil for pain in M.E.
Other pain medications
Other analgesic treatments for chronic pain include lidocaine infusions, ketamine infusions, steroid injections such as cortisone, and benzodiazepines such as diazepam. Low dose naltrexone has also been reported to reduce chronic pain in ME/CFS and fibromyalgia. A variety of supplements and herbs are also used to reduce pain.[citation needed]
Non-pharmacological pain relief include as TENS, massage therapy, and hot and cold treatments see pain relief (analgesic).
Muscle relaxants
Muscle relaxants for pain in M.E.
Baclofen, cyclobenzaprine and magnesium sulfate (prescription strength) have evidence for their use in M.E./CFS.[3][8] Baclofen may help muscle fasciculations and muscle spasms, and magnesium sulfate can be used for leg cramps at night.[3][8]
Combinations
Adjuvants
Application
Topical
Topical pain medication is a form applied to the skin, typically as a cream or gel. Examples include ibuprofen and diclofenac gel (Volteral), and capsaicin 0.025% cream. Some topical pain medications are available over-the-counter.
Transdermal
Transdermal skin patches can be prescribed for severe pain, some may be left in place for a number of days while others may need to be applied by a medical professional only, and removed after an hour. Examples include capsaicin 8% patches, buproprion (an anti-depressant also used for nerve pain), lidocaine and opioid patches.
Weaker medicated heat or cold patches are also available over-the-counter.
Oral
Tablets and capsules are the most common forms of pain relief. Some drugs are also available as liquids or in slow-release forms, for example opioids.
Suppositories
These pain medication are usually inserted into the rectum. Examples include acetaminophen (paracetamol( suppositories, and indometacin (a non-steroid anti-inflammatory).
Injections and IV Drugs
Intramuscular injections, subcutaneous injections and IV pain medication are typically only administered by medical professionals and may a much higher dose than over-the-counter forms of the same drug, for example acetaminophen on IV or codeine injections.
Learn more
- Over-the-counter pain relievers: MedlinePlus
- Myalgic Encephalomyelitis - Adult & Paediatric International Consensus Primer for Medical Practitioners, p13, p17
- Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Canadian Consensus Criteria, p53-p55
- Review of M.E./CFS: an evidence-based approach to diagnosis and management by clinicians, table 5
- Which painkiller? - NHS
- Fibromyalgia treatment - NHS
- Opioids Aware - A resource for patients and health professionals to support the prescribing of opioid medications for pain
See also
References
- ↑ "Definition of ANALGESIC". Merrian-Webster Dictionary. Retrieved October 1, 2018.
- ↑ 2.0 2.1 Carruthers BM, van de Sande MI (2005). Myalgic encephalomyelitis, chronic fatigue syndrome : a clinical case definition and guidelines for medical practitioners : an overview of the Canadian consensus document (PDF). Vancouver, B.C.: Carruthers & van de Sande. ISBN 097393350X. OCLC 71361905.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 Carruthers, BM; van de Sande, MI; De Meirleir, KL; Klimas, NG; Broderick, G; Mitchell, T; Staines, D; Powles, ACP; Speight, N; Vallings, R; Bateman, L; Bell, DS; Carlo-Stella, N; Chia, J; Darragh, A; Gerken, A; Jo, D; Lewis, DP; Light, AR; Light, KC; Marshall-Gradisnik, S; McLaren-Howard, J; Mena, I; Miwa, K; Murovska, M; Stevens, SR (2012), Myalgic encephalomyelitis: Adult & Paediatric: International Consensus Primer for Medical Practitioners (PDF), ISBN 978-0-9739335-3-6
- ↑ Bested, Alison C.; Marshall, Lynn M. (November 2, 2015). "Review of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: an evidence-based approach to diagnosis and management by clinicians" (PDF). Reviews on Environmental Health. 30 (4). doi:10.1515/reveh-2015-0026. ISSN 2191-0308.
- ↑ 5.0 5.1 "Over-the-counter pain relievers: MedlinePlus Medical Encyclopedia". medlineplus.gov. Retrieved October 2, 2018.
- ↑ 6.0 6.1 "Acetaminophen Monograph for Professionals - Drugs.com". Drugs.com. Retrieved October 1, 2018.
- ↑ 7.0 7.1 7.2 "Acetaminophen Dosage Guide with Precautions - Drugs.com". Drugs.com. Retrieved October 2, 2018.
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 Carruthers, Bruce M.; Jain, Anil Kumar; De Meirleir, Kenny L.; Peterson, Daniel L.; Klimas, Nancy G.; Lerner, A. Martin; Bested, Alison C.; Flor-Henry, Pierre; Joshi, Pradip (January 2003). "Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Clinical Working Case Definition, Diagnostic and Treatment Protocols" (PDF). Journal of Chronic Fatigue Syndrome. 11 (1): 7–115. doi:10.1300/j092v11n01_02. ISBN 0-7890-2207-9. ISSN 1057-3321.
- ↑ "Ketorolac - FDA prescribing information, side effects and uses". Drugs.com. Retrieved October 2, 2018.
- ↑ Hemmings, Hugh C.; Egan, Talmage D. (2013), Pharmacology and Physiology for Anesthesia: Foundations and Clinical Application: Expert Consult - Online and Print, Elsevier Health Science, p. 253, ISBN 1437716792,
Opiate is the older term classically used in pharmacology to mean a drug derived from opium. Opioid, a more modern term, is used to designate all substances, both natural and synthetic, that bind to opioid receptors (including antagonists).
- ↑ 11.0 11.1 11.2 The Royal College of Anaesthetists (2016). "Taking Opioids for Pain | Information for Patients". rcoa.ac.uk. Retrieved October 3, 2018.
- ↑ Carruthers, Bruce M.; Jain, Anil Kumar; De Meirleir, Kenny L.; Peterson, Daniel L.; Klimas, Nancy G.; Lerner, A. Martin; Bested, Alison C.; Flor-Henry, Pierre; Joshi, Pradip; Powles, AC Peter; Sherkey, Jeffrey A.; van de Sande, Marjorie I. (2003), "Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Clinical Working Case Definition, Diagnostic and Treatment Protocols" (PDF), Journal of Chronic Fatigue Syndrome, 11 (2): 7–115, doi:10.1300/J092v11n01_02
- ↑ 13.0 13.1 "Tricyclic Antidepressants: List, Uses & Side Effects - Drugs.com". Drugs.com. Retrieved October 1, 2018.
- ↑ Rogawski, Michael A.; Löscher, Wolfgang (2004), "The neurobiology of antiepileptic drugs", Nature Reviews Neuroscience, 5 (7): 553-564, doi:10.1038/nrn1430, PMID 15208697
- ↑ Jensen, Bjorn; Chen, Jeffrey; Furnish, Tim; Wallace, Mark (September 1, 2015), "Medical Marijuana and Chronic Pain: a Review of Basic Science and Clinical Evidence", Current Pain and Headache Reports, 19 (10), doi:10.1007/s11916-015-0524-x

