- This page was created by volunteers like you!
- Help us make it even better. To learn more about contributing to MEpedia, click here.
- Join the movement
- Visit #MEAction to find support or take action. Donate today to help us improve and expand this project.
Autoimmune hypothesis
This article is a stub. |
Theory
The Open Medicine Foundation, with immunologist Mark Davis, and geneticist Lars Steinmetz, is currently investigating the replication of T cells in ME, which may indicate an autoimmune disease is present in some ME/CFS patients.[1] HLA gene associations are a possible hallmark of autoimmune disease, and were investigated by Fluge et al. in 2020.[2]
Evidence
ME/CFS can cause a number of immune symptoms including a sore throat, swollen lymph nodes, and flu-like symptoms.[3][4]
Evidence for autoimmunity in ME and CFS
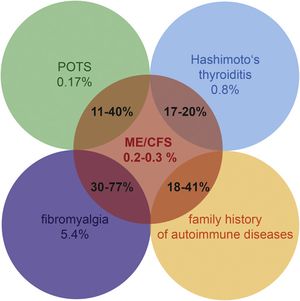
Many people with ME/CFS also have autoimmune conditions such as Hashimoto's thyroiditis, or have a family history of autoimmune diseases.[5] POTS, or postural orthostatic tachycardia syndrome, can be initiated or maintained by autoantibodies as well, and POTS is common in people with ME. A number of different immune system abnormalities have been found in some patients with ME/CFS.[5]
One study found elevated cellular antigens in 83% of CFS patients.[6]
Autoimmune disease is one of several illnesses or conditions experienced alongside of ME/CFS.[7]
Samples from a large cohort (n=268) in Berlin, Germany and a smaller sample of patients treated with Rituximab (n=25) were measured against controls (n=168). Researchers found that antibodies against a neurotransmitter receptor were elevated in 29.5% of patients. Specifically, antibodies to ß2 adrenergic and M3 and M4 muscarinic cholinergic receptors, which are both G protein-coupled receptors (GCPRs). In patients receiving Rituximab, those who were responders had significantly lower levels of ß2 and M4 autoantibodies after treatment. The authors suggest that these autoantibodies could be biomarkers to those CFS patients most likely to respond to Rituximab treatment.[8][9]
Notable studies
- 2020, Autoantibodies to beta-adrenergic and muscarinic cholinergic receptors in Myalgic Encephalomyelitis (ME) patients – A validation study in plasma and cerebrospinal fluid from two Swedish cohorts[10] - (Full text)
- 2020, Human Leukocyte Antigen alleles associated with Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)[2] - (Full text)
- 2018, Infection Elicited Autoimmunity and Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: An Explanatory Model[11] - (Full text)
- 2018, Myalgic Encephalomyelitis/Chronic Fatigue Syndrome – Evidence for an autoimmune disease[5]
- 2017-2020, Defining Autoimmune Aspects of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)[12] - Clinical Trial
- 2014, The emerging role of autoimmunity in myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS)[13]
- 2013, In myalgic encephalomyelitis/chronic fatigue syndrome, increased autoimmune activity against 5-HT is associated with immuno-inflammatory pathways and bacterial translocation[14]
- 2012, Increased autoimmune activity against 5-HT: a key component of depression that is associated with inflammation and activation of cell-mediated immunity, and with severity and staging of depression[15]
- 2004, Is chronic fatigue syndrome an autoimmune disorder of endogenous neuropeptides, exogenous infection and molecular mimicry?[16] - Donald Staines
Talks and interviews
- 2015, Partnerships to Accelerate Biomarker and Mechanisms Discovery in ME/CFS and Fibromyalgia - Professor Alan Light discusses recent studies hypothesising autoimmune causation)
See also
- Autoimmune disease
- Innate immune system
- Rituximab
- Cyclophosphamide
- Autoantibody
- Human leukocyte antigen genes (HLA genes)
Learn more
- T-cells, molecular Immunology and autoimmune hypothesis[1] - Open Medicine Foundation
- Autoimmune encephalitis - diagnosis - International Autoimmune Encephalitis Society
- Autoimmune encephalitis - Genetic and Rare Diseases Information Center
References
- ↑ 1.0 1.1 Open Medicine Foundation (February 28, 2018). "OMF-funded research: T cells and molecular immunology". Open Medicine Foundation. Retrieved July 11, 2019.
- ↑ 2.0 2.1 Lande, Asgeir; Fluge, Øystein; Strand, Elin B.; Flåm, Siri T.; Sosa, Daysi D.; Mella, Olav; Egeland, Torstein; Saugstad, Ola D.; Lie, Benedicte A. (March 24, 2020). "Human Leukocyte Antigen alleles associated with Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)". Scientific Reports. 10 (1): 1–8. doi:10.1038/s41598-020-62157-x. ISSN 2045-2322.
- ↑ Carruthers, BM; van de Sande, MI; De Meirleir, KL; Klimas, NG; Broderick, G; Mitchell, T; Staines, D; Powles, ACP; Speight, N; Vallings, R; Bateman, L; Bell, DS; Carlo-Stella, N; Chia, J; Darragh, A; Gerken, A; Jo, D; Lewis, DP; Light, AR; Light, KC; Marshall-Gradisnik, S; McLaren-Howard, J; Mena, I; Miwa, K; Murovska, M; Stevens, SR (2012), Myalgic encephalomyelitis: Adult & Paediatric: International Consensus Primer for Medical Practitioners (PDF), ISBN 978-0-9739335-3-6
- ↑ Fukuda, K.; Straus, S.E.; Hickie, I.; Sharpe, M.C.; Dobbins, J.G.; Komaroff, A. (December 15, 1994). "The chronic fatigue syndrome: a comprehensive approach to its definition and study. International Chronic Fatigue Syndrome Study Group" (PDF). Annals of Internal Medicine. American College of Physicians. 121 (12): 953–959. ISSN 0003-4819. PMID 7978722.
- ↑ 5.0 5.1 5.2 Sotzny, Franziska; Blanco, Julià; Capelli, Enrica; Castro-Marrero, Jesús; Steiner, Sophie; Murovska, Modra; Scheibenbogen, Carmen (2018), "Myalgic Encephalomyelitis/Chronic Fatigue Syndrome – Evidence for an autoimmune disease", Autoimmunity Reviews, 17 (6): 601-609, doi:10.1016/j.autrev.2018.01.009
- ↑ von Mikecz, A.; Konstantinov, K.; Buchwald, D.S.; Gerace, L.; Tan, E.M. (February 1997). "High frequency of autoantibodies to insoluble cellular antigens in patients with chronic fatigue syndrome". Arthritis and Rheumatism. 40 (2): 295–305. ISSN 0004-3591. PMID 9041942.
- ↑ "Overlapping Conditions – American ME and CFS Society". ammes.org. Retrieved August 12, 2018.
- ↑ "Autoantibodies found in subset of CFS patients | #MEAction". The MEAction Network. Retrieved August 12, 2018.
- ↑ Loebel, Madlen; Grabowski, Patricia; Heidecke, Harald; Bauer, Sandra; Hanitsch, Leif G.; Wittke, Kirsten; Meisel, Christian; Reinke, Petra; Volk, Hans-Dieter (February 2016). "Antibodies to β adrenergic and muscarinic cholinergic receptors in patients with Chronic Fatigue Syndrome". Brain, Behavior, and Immunity. 52: 32–39. doi:10.1016/j.bbi.2015.09.013. ISSN 1090-2139. PMID 26399744.
- ↑ Bynke, Annie; Julin, Per; Gottfries, Carl-Gerhard; Heidecke, Harald; Scheibenbogen, Carmen; Bergquist, Jonas (August 1, 2020). "Autoantibodies to beta-adrenergic and muscarinic cholinergic receptors in Myalgic Encephalomyelitis (ME) patients – A validation study in plasma and cerebrospinal fluid from two Swedish cohorts". Brain, Behavior, & Immunity - Health. 7: 100107. doi:10.1016/j.bbih.2020.100107. ISSN 2666-3546.
- ↑ Blomberg, Jonas; Gottfries, Carl-Gerhard; Elfaitouri, Amal; Rizwan, Muhammad; Rosén, Anders (February 15, 2018). "Infection Elicited Autoimmunity and Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: An Explanatory Model". Frontiers in Immunology. 9. doi:10.3389/fimmu.2018.00229. ISSN 1664-3224. PMC 5818468. PMID 29497420.
- ↑ "Autoimmunity in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS) - Full Text View". clinicaltrials.gov. Retrieved April 25, 2020.
- ↑ Morris, Gerwyn; Berk, Michael; Galecki, Piotr; Maes, Michael (April 1, 2014). "The Emerging Role of Autoimmunity in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/cfs)". Molecular Neurobiology. 49 (2): 741–756. doi:10.1007/s12035-013-8553-0. ISSN 1559-1182.
- ↑ Maes, Michael; Ringel, Karl; Kubera, Marta; Anderson, George; Morris, Gerwyn; Galecki, Piotr; Geffard, Michel (September 5, 2013). "In myalgic encephalomyelitis/chronic fatigue syndrome, increased autoimmune activity against 5-HT is associated with immuno-inflammatory pathways and bacterial translocation". Journal of Affective Disorders. 150 (2): 223–230. doi:10.1016/j.jad.2013.03.029. ISSN 0165-0327.
- ↑ Maes, Michael; Ringel, Karl; Kubera, Marta; Berk, Michael; Rybakowski, Janusz Rybakowski (February 1, 2012). "Increased autoimmune activity against 5-HT : a key component of depression that is associated with inflammation and activation of cell-mediated immunity, and with severity and staging of depression". Journal of affective disorders. 136 (3): 386–392. doi:10.1016/j.jad.2011.11.016. ISSN 0165-0327.
- ↑ Staines, Donald R (May 1, 2004). "Is chronic fatigue syndrome an autoimmune disorder of endogenous neuropeptides, exogenous infection and molecular mimicry?". Medical Hypotheses. 62 (5): 646–652. doi:10.1016/j.mehy.2004.01.012. ISSN 0306-9877.

