- This page was created by volunteers like you!
- Help us make it even better. To learn more about contributing to MEpedia, click here.
- Join the movement
- Visit #MEAction to find support or take action. Donate today to help us improve and expand this project.
Hypokalemic periodic paralysis
Hypokalemic periodic paralysis (hypoKPP) is a rare channelopathy characterized by repeated, temporary attacks of muscle weakness or paralysis that are the result of a fall in potassium levels in the blood.[1]
Hypokalemic periodic paralysis can be either genetic (familial) or acquired (not life long), and is classed as a form of acute flaccid paralysis,[2][3] and has been described in people with severe myalgic encephalomyelitis.[4]
Types of periodic paralysis
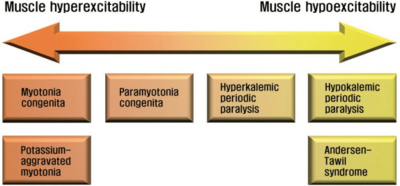
Image: K June-Bum, 2014[1] CC-BY-NC-3.0
Hypokalemic periodic paralysis is one of several types of periodic paralysis.
Other types include hyperkalemic periodic paralysis, which is linked to high potassium levels, thyrotoxic periodic paralysis, linked to thyroid hormone levels.[1]
Muscle weakness
Muscle weakness may be mild and limited to certain muscle groups, resulting in partial paralysis or paresis, or more severe full-body paralysis. During an attack reflexes may be decreased or absent. Hypokalemic periodic paralysis attacks may last for a few hours, or persist for several days. Recovery is usually sudden, and occurs when the swollen muscles release potassium as they recover.[5][6]
Prevalence
Hypokalemic periodic paralysis is said to be rare in the general population,[5] but has been found in people with ME/CFS, especially in people with severe and very severe ME.[4]
De Becker et al. (2001) conducted a large study of chronic fatigue syndrome patients, and found that 27.2% of patients meeting the Fukuda criteria and 33.2% of patients meeting the Holmes criteria for CFS experienced episodes of paralysis.[7]
Symptom recognition
Hypokalemic periodic paralysis was only discovered fairly recently.[1] It is commonly misdiagnosed as conversion disorder or "functional" paralysis, and can be missed since potassium levels may be normal between attacks.[6]
The International Consensus Criteria and the International Consensus Primer refer to channelopathies and ion transportation problems, but do not mention hypokalemic periodic paralysis directly.[8]
Notable studies
- 2003, Paralysis: A qualitative study of the people with Severe Myalgic Encephalomyelitis[4] - [(Full text), not peer reviewed
- 2001, A definition‐based analysis of symptoms in a large cohort of patients with chronic fatigue syndrome[7] - (Full text)
Causes of temporary paralysis
In individuals with the inherited genetic mutation, attacks often begin in adolescence. Attacks of paralysis are most commonly occur:
- on awakening or after sleep
- after rest following strenuous exercise (attacks during exercise are rare)
- after high carbohydrate meals
- after meals with high sodium content (high salt content)
- as a result of sudden changes in temperature, or cold temperatures
- sensory input, such as noise, or flashing lights may trigger paralysis
- and even excitement.[6]
Potential treatments
Electrolytes are one of the suggestions for treating energy metabolism and ion transportation problems in ME. Potassium would seem the obvious electrolyte, and is used to treat and reduce attacks of hypokalemic periodic paralysis in people without comorbid ME/CFS.[5][6]
See also
Learn more
- Hypokalemic periodic paralysis - Genetic and Rare Diseases Information Center
- Channelopathies (review) - Kim June-Bum.
- Periodic Paralysis - What clinicians should know
References
- ↑ 1.0 1.1 1.2 1.3 Kim, June-Bum (January 2014). "Channelopathies". Korean Journal of Pediatrics. 57 (1): 1–18. doi:10.3345/kjp.2014.57.1.1. ISSN 1738-1061. PMC 3935107. PMID 24578711.
- ↑ Padmaperuma, Pacd; Dissanayake, H.A. (July 18, 2018). "Periodic paralysis: what clinician needs to know?". Endocrinology & Metabolism International Journal. 6 (4): 1–0. doi:10.15406/emij.2018.6.00189. ISSN 2473-0815.
- ↑ Phuyal P, Nagalli S (November 25, 2021). Hypokalemic periodic paralysis. Treasure Island (FL): StatPearls Publishing LLC.
- ↑ 4.0 4.1 4.2 Crowhurst, Greg; Crowhurst, Linda (August 8, 2013). "Paralysis, a qualitative study of people with Severe Myalgic Encephalomyelitis". Stonebird. Retrieved December 28, 2018.
- ↑ 5.0 5.1 5.2 "Hypokalemic periodic paralysis". Genetic and Rare Diseases Information Center. Retrieved March 26, 2022.
- ↑ 6.0 6.1 6.2 6.3 Segal, Michael M.; Jurkat-Rott, Karin; Levitt, Jacob; Lehmann, Frank. "Hypokalemic Periodic Paralysis Owner's Manual". Retrieved March 26, 2022.
- ↑ 7.0 7.1 De Becker, Pascale; McGregor, Neil; De Meirleir, Kenny (December 2001). "A definition‐based analysis of symptoms in a large cohort of patients with chronic fatigue syndrome". Journal of Internal Medicine. 250 (3): 234–240. doi:10.1046/j.1365-2796.2001.00890.x.
- ↑ Carruthers, BM; van de Sande, MI; De Meirleir, KL; Klimas, NG; Broderick, G; Mitchell, T; Staines, D; Powles, ACP; Speight, N; Vallings, R; Bateman, L; Bell, DS; Carlo-Stella, N; Chia, J; Darragh, A; Gerken, A; Jo, D; Lewis, DP; Light, AR; Light, KC; Marshall-Gradisnik, S; McLaren-Howard, J; Mena, I; Miwa, K; Murovska, M; Stevens, SR (2012), Myalgic encephalomyelitis: Adult & Paediatric: International Consensus Primer for Medical Practitioners (PDF), ISBN 978-0-9739335-3-6

