- This page was created by volunteers like you!
- Help us make it even better. To learn more about contributing to MEpedia, click here.
- Join the movement
- Visit #MEAction to find support or take action. Donate today to help us improve and expand this project.
Fibromyalgia notable studies
Fibromyalgia notable studies houses the research for the Fibromyalgia (FM/FMS) page.
Notable studies
2000-2004
- 2002, Functional magnetic resonance imaging evidence of augmented pain processing in fibromyalgia[1]
- Reported as Fibromyalgia Pain Isn't All In Patient's Heads, New Brain Study Finds
- 2004, A link between irritable bowel syndrome and fibromyalgia may be related to findings on lactulose breath testing[2]
2005-2009
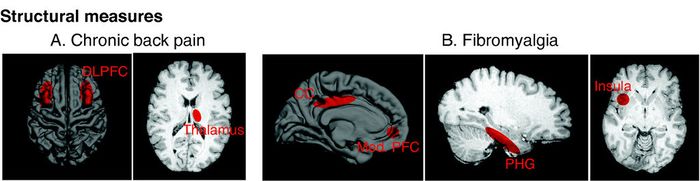
Chronic pain is a multidimensional process that now must be considered as a chronic degenerative disease not only affecting sensory and emotional processing, but also producing an altered brain state. Therapeutic interventions should be reconsidered in this context.[4]
- 2007, Clinical and Economic Characteristics of Patients With Fibromyalgia Syndrome[5] (Abstract)
- 2008, Symptom Clusters in Fibromyalgia[6] (Abstract)
2010-2014
- 2010, Interstitial cystitis/painful bladder syndrome and associated medical conditions with an emphasis on irritable bowel syndrome, fibromyalgia and chronic fatigue syndrome.[8]
- 2010, Pain Inhibition Is Deficient in Chronic Widespread Pain but Normal in Major Depressive Disorder[9]
- 2011, Fibromyalgia and neuropathic pain - differences and similarities. A comparison of 3057 patients with diabetic painful neuropathy and fibromyalgia.[11]
- 2011, The comparative burden of mild, moderate and severe Fibromyalgia: results from a cross-sectional survey in the United States[13]
Pathophysiology: Although the etiology remains unclear, characteristic alterations in the pattern of sleep and changes in neuroendocrine transmitters such as serotonin, substance P, growth hormone and cortisol suggest that regulation of the autonomic and neuro-endocrine system appears to be the basis of the syndrome. Fibromyalgia is not a life-threatening, deforming, or progressive disease. Anxiety and depression are the most common association. Aberrant pain processing, which can result in chronic pain, may be the result of several interplaying mechanisms. Central sensitization, blunting of inhibitory pain pathways and alterations in neurotransmitters lead to aberrant neuro-chemical processing of sensory signals in the CNS, thus lowering the threshold of pain and amplification of normal sensory signals causing constant pain.[14]
The frequent co-morbidity of fibromyalgia with mood disorders suggests a major role for the stress response and for neuroendocrine abnormalities. The hypothalamic pituitary axis (HPA) is a critical component of the stress-adaptation response. In FMS, stress adaptation response is disturbed leading to stress induce symptoms. Psychiatric co-morbidity has been associated with FMS and needs to be identified during the consultation process, as this requires special consideration during treatment.[14]
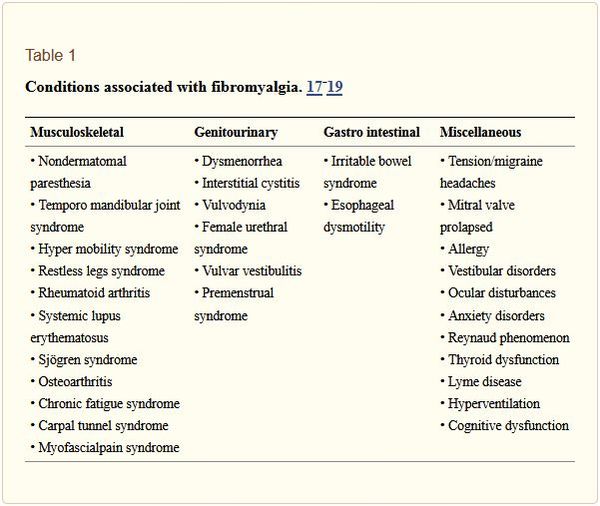
Source: Oman Med J 2012 May; 27(3):192-195. Jahan F, Nanji K, Qidwai W, Qasim R.Fibromyalgia Syndrome: An Overview of Pathophysiology, Diagnosis and Management. Oman Med J 2012 May; 27(3):192-195. Table 1.[14] License: CC BY-NC-4.0
- 2012, Dysfunctional endogenous analgesia during exercise in patients with chronic pain: To exercise or not to exercise?[15]
- 2014, Aquatic exercise training for fibromyalgia.[16]
2015-2019
Whole-brain voxel-wise analyses. (A) Median SUVR map from healthy controls (n = 9) and patients with chronic LBP (n = 10) are presented. Matched-pairs tests (nine versus nine) revealed significantly higher TSPO levels in patients, in thalamus, pre- and postcentral gyri, and paracentral lobule (P < 0.05 corrected for multiple comparisons; permutation testing, 10 000 permutations). As two patients were matching the same controls, the analyses were performed first using the patient best matching the control. A second analysis was performed using the other patient, limiting our search to significant clusters from the first analysis, with identical results. (B) Boxplots for each of the four regions demonstrating statistically higher SUVRs in patients are shown for illustrative purposes. postc. = postcentral; g. = gyrus; parac. lob. = postcentral lobule; prec. = precentral.[17]
- 2015, Some oxidative and antioxidative parameters and their relationship with clinical symptoms in women with fibromyalgia syndrome[18]
- 2015, Understanding the Association of Fatigue With Other Symptoms of Fibromyalgia: Development of a Cluster Model [19]
- 2015, Evaluation of Antiviral Antibodies against Epstein-Barr Virus and Neurotransmitters in Patients with Fibromyalgia[20]
- 2015, Sleep is associated with task-negative brain activity in fibromyalgia participants with comorbid chronic insomnia[21]
- 2015, Cognitive performance is related to central sensitization in patients with chronic whiplash-associated disorders and fibromyalgia: a case-control study[22]
- 2015, Normalization of aberrant resting state functional connectivity in fibromyalgia patients following a three-month physical exercise therapy[24]
Our model also suggests that drugs that specifically target the somatosensory thalamus may be effective in treating fibromyalgia.[25]
- 2015, The effects of aquatic, isometric strength-stretching and aerobic exercise on physical and psychological parameters of female patients with fibromyalgia syndrome[27]
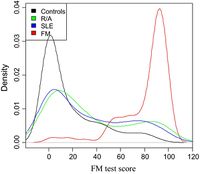
- 2015, Cytokine and chemokine profiles in fibromyalgia, rheumatoid arthritis, and systemic lupus erythematosus: a potentially useful tool in differential diagnosis.[28]
Nearly 500 FM, autoimmune and healthy control patients underwent testing for cytokine/chemokine activity after mitogenic stimulation. Using a numerical score, all three groups had unique patterns with FM patients demonstrating less response to stimulation. This cytokine profile test had a 93 % sensitivity and an 89.4 % specificity for the diagnosis of FM. We also found that these profiles are relatively sensitive and specific for FM compared to SLE and RA. It remains unclear if these differences are directly related to the pathogenesis of FM.[28]
- 2015, The Somatosensory Link in Fibromyalgia: Functional Connectivity of the Primary Somatosensory Cortex Is Altered by Sustained Pain and Is Associated With Clinical/Autonomic Dysfunction[29]
- 2015, Identification of a MicroRNA Signature for the Diagnosis of Fibromyalgia[30]
- 2016, Fibromyalgia syndrome: metabolic and autophagic processes in intermittent cold stress mice.[31]
- 2016, The association between borderline personality disorder, fibromyalgia and chronic fatigue syndrome: systematic review[32]
There does not appear to be firm and consistent evidence to support the hypothesis that the prevalence of BPD (Borderline Personality Disorder) would be higher in individuals with fibromyalgia compared with the general population.[32]
Fibromyalgia causes subclinical axonal damage in the RNFL that can be detected using innocuous and non-invasive OCT, even in the early disease stages. The impact on the RNFL in the temporal sectors is greater in patients with biologic fibromyalgia, suggesting the presence of neurodegenerative processes in this subgroup of patients with fibromyalgia.[33]
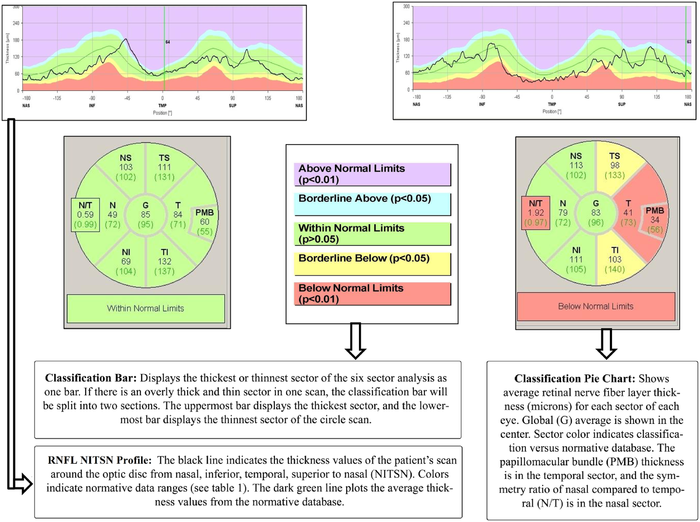
- 2016, Characteristics of Disturbed Sleep in Patients With Fibromyalgia Compared With Insomnia or With Pain-Free Volunteers[36]
- 2016, Is Efficacy of Milnacipran in Fibromyalgia Predictable? A Data Mining Analysis of Baseline and Outcome Variables.[37]
- 2017, The degree of cardiac baroreflex involvement during active standing is associated with the quality of life in fibromyalgia patients.[38] (Orthostatic intollerance.)
- 2017, Evidence of both systemic inflammation and neuroinflammation in fibromyalgia patients, as assessed by a multiplex protein panel applied to the cerebrospinal fluid and to plasma[39]
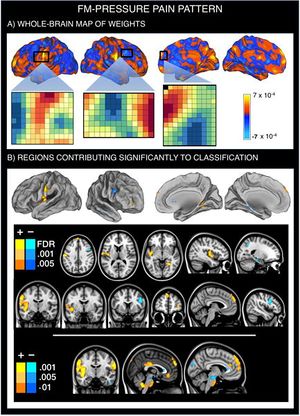
Here, we identify a set of three brain patterns based on fMRI responses to pressure pain and non-painful multisensory stimulation. These patterns, taken together, discriminate FM from matched healthy controls with 92% sensitivity and 94% specificity.[40]
Figure 2. Multivariate brain pattern that predicts fibromyalgia status on the basis of brain activation during painful (pressure) stimulation. Positive weight values reflect higher pain-evoked activation in FM patients relative to healthy participants, whereas negative weight values reflect reduced pain-evoked activation in FM patients. A. SVM pattern of whole-brain voxel weights that optimizes classification of FM patients and healthy participants. We provide the voxel-by-voxel weights for three representative regions (anterior SII, right dorsolateral and dorsomedial PFC) to illustrate the concept of weighted pattern. B. Regions whose voxel weights contributed most reliably to the prediction of FM status (q<0.05 FDR-corrected for the first two rows; p-uncorrected<0.001 to further illustrate the findings).[40]
- 2018, A Blinded, Randomized, Placebo-Controlled Study to Investigate the Efficacy and Safety of Ferric Carboxymaltose in Iron-Deficient Patients with Fibromyalgia.[42]
- 2018, Primary and Secondary Fibromyalgia Are The Same: The Universality of Polysymptomatic Distress[43] "PFM and SFM are equivalent regarding symptom burden."[43]
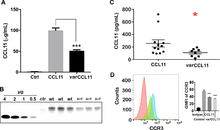
SNPs with significant TDTs were found in 36% of the cohort for CCL11 and 12% for MEFV, along with a protein variant in CCL4 (41%) that affects CCR5 down-regulation, supporting an immune involvement for FM.[44]
-
Fig 1. Expression of wild type and variant (Ala23Thr) CCL11
-
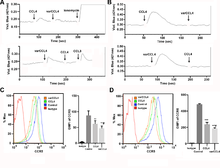
Fig 3. Functional analyses of WT vs varCCL4 in immature dendritic cells or CEM.NKR CCR5 T-cells
-
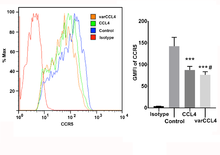
Fig 4. Wild type versus varCCL4 in the down-regulation of CCR5 in a 9 day mixed lymphocyte culture
- 2018, A comparison of the clinical manifestation and pathophysiology of myofascial pain syndrome and fibromyalgia: implications for differential diagnosis and management[46]:Table 1 "Summary of the pathophysiology of fibromyalgia and myofascial pain syndrome." p. 29
- See Table 1 "Summary of the pathophysiology of fibromyalgia and myofascial pain syndrome." p. 29 (p. 4 of PDF)
- 2018, Brain glial activation in fibromyalgia – A multi-site positron emission tomography investigation[47]
Our work provides the first in vivo evidence supporting a role for glial activation in FM pathophysiology. Given that the elevations in [11C]PBR28 signal were not also accompanied by increased [11C]-L-deprenyl-D2 signal, our data suggests that microglia, but not astrocytes, may be driving the TSPO elevation in these regions. Although [11C]-L-deprenyl-D2 signal was not found to be increased in FM patients, larger studies are needed to further assess the role of possible astrocytic contributions in FM. Overall, our data support glial modulation as a potential therapeutic strategy for FM.[47]
-
Fig 1. Fibromyalgia Glial Activation Voxelwise group differences in [11C]PBR28 VT. A
-
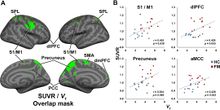
Fig. 2. Fibromyalgia Glial Activation Voxelwise group differences in [11C]PBR28 SUVR A
-
Fig. 3. Fibromyalgia Glial Activation Agreement between SUVR and VT analyses A
-
Fig 4. Fibromyalgia Glial Cells Associations between [11C]PBR28 SUVR and clinical variables
-
Fig. 5. Fibromyalgia Glial Cells Absence of group differences in [11C]-L-deprenyl-D2 λk3
- 2018, Altered Cervical Spinal Cord Resting State Activity in Fibromyalgia[48] (See: "Supporting Information" for images.)
- 2018, Fibromyalgia diagnosis and biased assessment: Sex, prevalence and bias[49]
What we did not find in our unbiased CritFM samples was 9:1 female to male fibromyalgia ratios that are widely described by expert sources [11–13]. We believe that such findings only occur in the presence of selection bias or biased ascertainment.[49]
As unbiased epidemiological studies show only a small increase in the female to male sex ratio (~1.5:1) as opposed to the observed ratio in clinical studies of 9:1, we believe that the over-identification of fibromyalgia in women and the consequent under-identification of men is the result of bias.[49]
- 2018, Characterizing classes of fibromyalgia within the continuum of central sensitization syndrome[50]
FM is a disease continuum characterized by progressive and identifiable classifications. Four classes of FM can be differentiated by pain and symptom severity, specific comorbidities, and use of clinical procedures.[50]
- 2018, Myalgic Encephalomyelitis/Chronic Fatigue Syndrome and Fibromyalgia: Definitions, Similarities, and Differences[51]
This commentary presents a simplified way of making the diagnosis of myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) using the 1994 Centers for Disease Control and Prevention case definition. The format used can easily be modified for other case definitions. The commentary then discusses whether ME/CFS is the same or a different illness from fibromyalgia. Because overlap exists between the 2 syndromes, some investigators have posited that they are variants of the same illness. I have viewed this as an empirically testable hypothesis and have summoned considerable amounts of data that suggest that the 2 illnesses differ. Were differences to exist, that would suggest different pathophysiologic processes for each, leading to different treatments.[51]
- A fibromyalgia blood test was the aim of the study by Hacksaw et al (2018), which looked for a fibromyalgia biomarker and found a unique metabolic fingerprint which distinguished all patients with fibromyalgia from those with systemic lupus erythematosus, rheumatoid arthritis and osteoarthritis.[53] The study only analysed blood samples from rheumatic diseases, so it did not include patients with ME/CFS or other illnesses which can chronic pain.[53]
- 2019, RETRACTED Is insulin resistance the cause of fibromyalgia? A preliminary report[54] (Full text)
- Retraction notice. :Retracted due to post-publication ethics approval and lack of gender, age and ethnic group controls in comparison group.
- 2019, A systematic review and meta-analysis of the prevalence of small fiber pathology in fibromyalgia: Implications for a new paradigm in fibromyalgia ethiopathogenesis[55]
- 2019, An experimental randomized study on the analgesic effects of pharmaceutical-grade cannabis in chronic pain patients with fibromyalgia[57]
2020-2024
- 2020, Determining the association between fibromyalgia, the gut microbiome and its biomarkers: A systematic review [61]
- 2020, A systematic review of the association between fibromyalgia and functional gastrointestinal disorders[62]
- 2020, Investigating Fatigue and Exercise Intolerance in a University Immunology Clinic[63]
- 2020, Comorbidities of self-reported fibromyalgia in United States adults: A cross-sectional study from The National Epidemiological Survey on Alcohol and Related Conditions (NESARC-III)[65]
- 2020, Is Transcranial Direct Current Stimulation (tDCS) Effective for the Treatment of Pain in Fibromyalgia? A Systematic Review and Meta-Analysis[66]
- 2020, Effects of transcranial direct current stimulation and transcranial magnetic stimulation in patients with fibromyalgia. A systematic review[67]
- 2021, Analysis of Retinal Layers in Fibromyalgia Patients with Premium Protocol in Optical Tomography Coherence and Quality of Life[68]
- A potential biomarker for fibromyalgia, using a non-invasive eye test.
- 2021, The Search for Biomarkers in Fibromyalgia[69]
- 2021, Insulin Resistance is Associated with Central Pain in Patients with Fibromyalgia Observational Study[70] - authors in common with the retracted 2019 insulin resistance study
Depression and anxiety
- 2008, The relationship between fibromyalgia and major depressive disorder: a comprehensive review[71] (Abstract)
- 2010, Anxiety and depressive symptoms in fibromyalgia are related to poor perception of health but not to pain sensitivity or cerebral processing of pain[72] (Abstract)
- 2012, Fibromyalgia a discrete entity?[73] (Full text)
Psychological paradigm
- 2012, Personality and Fibromyalgia Syndrome[74] (Full text)
Conclusion: No specific fibromyalgia personality is defined but it is proposed that personality is an important filter that modulates a person’s response to psychological stressors. Certain personalities may facilitate translation of these stressors to physiological responses driving the fibromyalgia mechanism.[74]
- 2015, Brain "fog," inflammation and obesity: key aspects of neuropsychiatric disorders improved by luteolin.[75] (Full text)
- 2015, Hyperbaric Oxygen Therapy Can Diminish Fibromyalgia Syndrome[76] (Full text)
- 2016, Explaining unexplained pain to fibromyalgia patients: finding a narrative that is acceptable to patients and provides a rationale for evidence-based interventions[77] (Full text)
- 2016, Fibromyalgia: A Short Commentary[78] (Full text)
Grant awards and current research
- Oct 2016, Chronic pain researchers to expand work with $7.5M award from NIH[79]
- Jun 2018, The Bateman Horne Center will be an All of Us recruitment center for people living with ME/CFS and fibromyalgia. All of Us is a ten year Precision Medicine Initiative project that has been funded $1.5 Billion to recruit one million patients for its bio-bank. The idea is to research all diseases, from the most common to the most rare while taking into account lifestyle, environment, and biology.[80][81]
See also
References
- ↑ Gracely, Richard H.; Petzke, Frank; Wolf, Julie M.; Clauw, Daniel J. (2002). "Functional magnetic resonance imaging evidence of augmented pain processing in fibromyalgia". Arthritis & Rheumatism. 46 (5): 1333–1343. doi:10.1002/art.10225. ISSN 1529-0131.
- ↑ Pimentel, M; Wallace, D; Hallegua, D; Chow, E; Kong, Y; Park, S; Lin, H (2004). "A link between irritable bowel syndrome and fibromyalgia may be related to findings on lactulose breath testing". Annals of the Rheumatic Diseases. 63 (4): 450–452. doi:10.1136/ard.2003.011502. ISSN 0003-4967. PMID 15020342.
- ↑ Ifergane, G.; Buskila, D.; Simiseshvely, N.; Zeev, K.; Cohen, H. (2006). "Prevalence of fibromyalgia syndrome in migraine patients". Cephalalgia: An International Journal of Headache. 26 (4): 451–456. doi:10.1111/j.1468-2982.2005.01060.x. ISSN 0333-1024. PMID 16556247.
- ↑ 4.0 4.1 4.2 Borsook, David; Moulton, Eric A; Schmidt, Karl F; Becerra, Lino R (September 11, 2007). "Neuroimaging Revolutionizes Therapeutic Approaches to Chronic Pain". Molecular Pain. 3 (1): 1744–8069-3-25. doi:10.1186/1744-8069-3-25. ISSN 1744-8069. PMID 17848191.
- ↑ Lachaine, Jean; Beauchemin, Catherine; Landry, Pierre-Alexandre (May 2010). "Clinical and Economic Characteristics of Patients With Fibromyalgia Syndrome". The Clinical Journal of Pain. 26 (4): 284–290. doi:10.1097/AJP.0b013e3181cf599f. ISSN 0749-8047.
- ↑ Rutledge, Dana N.; Mouttapa, Michele; Wood, Patrick B. (September 2009). "Symptom Clusters in Fibromyalgia". Nursing Research. 58 (5): 359–367. doi:10.1097/NNR.0b013e3181b499d2. ISSN 0029-6562.
- ↑ de Tommaso, M.; Sardaro, M.; Serpino, C.; Costantini, F.; Vecchio, E.; Prudenzano, M. Pia; Lamberti, P.; Livrea, P. (2009). "Fibromyalgia comorbidity in primary headaches". Cephalalgia: An International Journal of Headache. 29 (4): 453–464. doi:10.1111/j.1468-2982.2008.01754.x. ISSN 1468-2982. PMID 19170692.
- ↑ Nickel, J. Curtis; Tripp, Dean A.; Pontari, Michel; Moldwin, Robert; Mayer, Robert; Carr, Lesley K.; Doggweiler, Ragi; Yang, Claire C.; Mishra, Nagendra (2010). "Interstitial cystitis/painful bladder syndrome and associated medical conditions with an emphasis on irritable bowel syndrome, fibromyalgia and chronic fatigue syndrome". The Journal of Urology. 184 (4): 1358–1363. doi:10.1016/j.juro.2010.06.005. ISSN 1527-3792. PMID 20719340.
- ↑ Normand, Edith; Potvin, Stéphane; Gaumond, Isabelle; Cloutier, Guylaine; Corbin, Jean-François; Marchand, Serge (August 10, 2010). "Pain Inhibition Is Deficient in Chronic Widespread Pain but Normal in Major Depressive Disorder". The Journal of Clinical Psychiatry. 72 (2): 219–224. doi:10.4088/JCP.08m04969blu.
- ↑ Arnold, Lesley M.; Clauw, Daniel J.; McCarberg, Bill H. (May 1, 2011). "Improving the Recognition and Diagnosis of Fibromyalgia". Mayo Clinic Proceedings. 86 (5): 457–464. doi:10.4065/mcp.2010.0738. ISSN 0025-6196.
- ↑ Koroschetz, Jana; Rehm, Stefanie E.; Gockel, Ulrich; Brosz, Mathias; Freynhagen, Rainer; Tölle, Thomas R.; Baron, Ralf (May 25, 2011). "Fibromyalgia and neuropathic pain - differences and similarities. A comparison of 3057 patients with diabetic painful neuropathy and fibromyalgia". BMC Neurology. 11 (1): 1–8. doi:10.1186/1471-2377-11-55. ISSN 1471-2377. PMC 3125308. PMID 21612589.
- ↑ Fitzcharles, Mary-Ann; Yunus, Muhammad B. (October 29, 2012). "The Clinical Concept of Fibromyalgia as a Changing Paradigm in the Past 20 Years". Pain Research and Treatment. 2012: 1–8. doi:10.1155/2012/184835. ISSN 2090-1542. PMC 3205680. PMID 22135738.
- ↑ Schaefer, Caroline; Chandran, Arthi; Hufstader, Meghan; Baik, Rebecca; McNett, Michael; Goldenberg, Don; Gerwin, Robert; Zlateva, Gergana (August 22, 2011). "The comparative burden of mild, moderate and severe Fibromyalgia: results from a cross-sectional survey in the United States". Health and Quality of Life Outcomes. 9 (1): 71. doi:10.1186/1477-7525-9-71. ISSN 1477-7525. PMC 3179696. PMID 21859448.
- ↑ 14.0 14.1 14.2 14.3 Jahan, Firdous; Nanji, Kashmira; Qidwai, Waris; Qasim, Rizwan (2012). "Fibromyalgia Syndrome: An Overview of Pathophysiology, Diagnosis and Management". Oman Medical Journal. 27 (3): 192–195. doi:10.5001/omj.2012.44. ISSN 1999-768X. PMID 22811766.
- ↑ Meeus, M.; Kosek, E.; Van Oosterwijck, J.; Nijs, J. (September 2011). "Dysfunctional endogenous analgesia during exercise in patients with chronic pain: To exercise or not to exercise?". European Journal of Pain Supplements. 5 (1): 8. doi:10.1016/s1754-3207(11)70024-4. ISSN 1754-3207.
- ↑ Bidonde, Julia; Busch, Angela J.; Webber, Sandra C.; Schachter, Candice L.; Danyliw, Adrienne; Overend, Tom J.; Richards, Rachel S.; Rader, Tamara (October 28, 2014). "Aquatic exercise training for fibromyalgia". The Cochrane Database of Systematic Reviews (10): CD011336. doi:10.1002/14651858.CD011336. ISSN 1469-493X. PMID 25350761.
- ↑ 17.0 17.1 Loggia, Marco L.; Chonde, Daniel B.; Akeju, Oluwaseun; Arabasz, Grae; Catana, Ciprian; Edwards, Robert R.; Hill, Elena; Hsu, Shirley; Izquierdo-Garcia, David (January 8, 2015). "Evidence for brain glial activation in chronic pain patients". Brain. 138 (3): 604–615. doi:10.1093/brain/awu377. ISSN 1460-2156.
- ↑ Fatima, Ghizal; Das, Siddharth Kumar; Mahdi, Abbas Ali (July 14, 2015). "Some oxidative and antioxidative parameters and their relationship with clinical symptoms in women with fibromyalgia syndrome". International Journal of Rheumatic Diseases. 20 (1): 39–45. doi:10.1111/1756-185x.12550. ISSN 1756-1841.
- ↑ Lukkahatai, Nada; Walitt, Brian; Espina, Alexandra; Gelio, Alves; Saligan, Leorey N. (December 21, 2015). "Understanding the Association of Fatigue With Other Symptoms of Fibromyalgia: Development of a Cluster Model". Arthritis Care & Research. 68 (1): 99–107. doi:10.1002/acr.22626. ISSN 2151-464X. PMID 26017904.
- ↑ Reshkova, V; D, Kalinova; Milanov, Ivan (January 1, 2015). "Evaluation of Antiviral Antibodies against Epstein-Barr Virus and Neurotransmitters in Patients with Fibromyalgia". Journal of Neurology and Neuroscience. 6: 35. doi:10.21767/2171-6625.100035.
- ↑ Vatthauer, Karlyn E; Craggs, Jason G; Robinson, Michael E; Staud, Roland; Berry, Richard B; Perlstein, William M; McCrae, Christina S (November 12, 2015). "Sleep is associated with task-negative brain activity in fibromyalgia participants with comorbid chronic insomnia". Journal of Pain Research. 8: 819–827. doi:10.2147/JPR.S87501. ISSN 1178-7090. PMID 26648751.
- ↑ Coppieters, Iris; Ickmans, Kelly; Cagnie, Barbara; Nijs, Jo; De Pauw, Robby; Meeus, Mira (2015). "Cognitive performance is related to central sensitization in patients with chronic whiplash-associated disorders and fibromyalgia: a case-control study". Pain Science in Motion congress, abstracts.
- ↑ Wyatt, H.J.; Day, N.W. (January 16, 1976). "Specific effects of neurotransmitter antagonists on ganglion cells in rabbit retina" (PDF). Science (New York, N.Y.). 191 (4223): 204–205. ISSN 0036-8075. PMID 1857 – via European Scientific Journal.
- ↑ "Normalization of aberrant resting state functional connectivity in fibromyalgia patients following a three month physical exercise therapy". NeuroImage: Clinical. 9: 134–139. January 1, 2015. doi:10.1016/j.nicl.2015.08.004. ISSN 2213-1582.
- ↑ 25.0 25.1 Vijayan, Sujith; Klerman, Elizabeth B.; Adler, Gail K.; Kopell, Nancy J. (September 1, 2015). "Thalamic mechanisms underlying alpha-delta sleep with implications for fibromyalgia". Journal of Neurophysiology. 114 (3): 1923–1930. doi:10.1152/jn.00280.2015. ISSN 0022-3077. PMC 4575971. PMID 26245315.
- ↑ Banafsheh, Ghavidel-Parsa; Ali, Bidari; Alireza, Amir Maafi; Babak, Ghalebaghi (July 1, 2015). "The Iceberg Nature of Fibromyalgia Burden: The Clinical and Economic Aspects". The Korean Journal of Pain. 28 (3). doi:10.3344/kjp.2015.28.3.169&code=0047kjp&vmode=full. ISSN 2005-9159.
- ↑ Sevimli, Dilek; Kozanoglu, Erkan; Guzel, Rengin; Doganay, Ahmet (2015). "The effects of aquatic, isometric strength-stretching and aerobic exercise on physical and psychological parameters of female patients with fibromyalgia syndrome". Journal of Physical Therapy Science. 27 (6): 1781–1786. doi:10.1589/jpts.27.1781. ISSN 0915-5287. PMID 26180320.
- ↑ 28.0 28.1 28.2 Wallace, Daniel J.; Gavin, Igor M.; Karpenko, Oleksly; Barkhordar, Farnaz; Gillis, Bruce S. (2015). "Cytokine and chemokine profiles in fibromyalgia, rheumatoid arthritis and systemic lupus erythematosus: a potentially useful tool in differential diagnosis". Rheumatology International. 35 (6): 991–996. doi:10.1007/s00296-014-3172-2. ISSN 1437-160X. PMID 25377646.
- ↑ Kim, Jieun; Loggia, Marco L.; Cahalan, Christine M.; Harris, Richard E.; Beissner, Florian; Garcia, Ronald G.; Kim, Hyungjun; Barbieri, Riccardo; Wasan, AjayD. (April 27, 2015). "The Somatosensory Link in Fibromyalgia: Functional Connectivity of the Primary Somatosensory Cortex Is Altered by Sustained Pain and Is Associated With Clinical/Autonomic Dysfunction". Arthritis & Rheumatology. 67 (5): 1395–1405. doi:10.1002/art.39043. ISSN 2326-5191. PMID 25622796.
- ↑ Cerdá-Olmedo, Germán; Mena-Durán, Armando Vicente; Monsalve, Vicente; Oltra, Elisa (March 24, 2015). "Identification of a MicroRNA Signature for the Diagnosis of Fibromyalgia". PLoS ONE. 10 (3). doi:10.1371/journal.pone.0121903. ISSN 1932-6203. PMID 25803872.
- ↑ Oezel, Lisa; Then, Hanna; Jung, Anna L.; Jabari, Samir; Bonaterra, Gabriel A.; Wissniowski, Thaddeus T.; Önel, Susanne F.; Ocker, Matthias; Thieme, Kati (2016). "Fibromyalgia syndrome: metabolic and autophagic processes in intermittent cold stress mice". Pharmacology Research & Perspectives. 4 (5): e00248. doi:10.1002/prp2.248. ISSN 2052-1707. PMID 27713820.
- ↑ 32.0 32.1 Penfold, Sarah; Denis, Emily St; Mazhar, Mir Nadeem (July 2016). "The association between borderline personality disorder, fibromyalgia and chronic fatigue syndrome: systematic review". BJPsych Open. 2 (4): 275–279. doi:10.1192/bjpo.bp.115.002808. ISSN 2056-4724.
- ↑ 33.0 33.1 Garcia-Martin, Elena; Garcia-Campayo, Javier; Puebla-Guedea, Marta; Ascaso, Francisco J.; Roca, Miguel; Gutierrez-Ruiz, Fernando; Vilades, Elisa; Polo, Vicente; Larrosa, Jose M. (September 1, 2016). "Fibromyalgia Is Correlated with Retinal Nerve Fiber Layer Thinning". PLOS ONE. 11 (9): e0161574. doi:10.1371/journal.pone.0161574. ISSN 1932-6203. PMID 27584145.
- ↑ Garcia-Martin, Elena; Garcia-Campayo, Javier; Puebla-Guedea, Marta; Ascaso, Francisco J.; Roca, Miguel; Gutierrez-Ruiz, Fernando; Vilades, Elisa; Polo, Vicente; Larrosa, Jose M. (September 1, 2016). "Fibromyalgia Is Correlated with Retinal Nerve Fiber Layer Thinning". PLOS ONE. 11 (9): e0161574. doi:10.1371/journal.pone.0161574. ISSN 1932-6203.
- ↑ Overman, Cécile L.; Kool, Marianne B.; Da Silva, José A.P.; Geenen, Rinie (2016). "The prevalence of severe fatigue in rheumatic diseases: an international study". Clinical Rheumatology. 35 (2): 409–415. doi:10.1007/s10067-015-3035-6. ISSN 1434-9949. PMID 26272057.
- ↑ Roth, Thomas; Bhadra-Brown, Pritha; Pitman, Verne W.; Roehrs, Timothy A.; Resnick, E. Malca (2016). "Characteristics of Disturbed Sleep in Patients With Fibromyalgia Compared With Insomnia or With Pain-Free Volunteers". The Clinical Journal of Pain. 32 (4): 302–307. doi:10.1097/AJP.0000000000000261. ISSN 0749-8047.
- ↑ Abtroun, Lilia; Bunouf, Pierre; Gendreau, Roger M.; Vitton, Olivier (2016). "Is the Efficacy of Milnacipran in Fibromyalgia Predictable? A Data-Mining Analysis of Baseline and Outcome Variables". The Clinical Journal of Pain. 32 (5): 435–440. doi:10.1097/AJP.0000000000000284. ISSN 1536-5409. PMID 26218005.
- ↑ Zamunér, Antonio Roberto; Porta, Alberto; Andrade, Carolina Pieroni; Forti, Meire; Marchi, Andrea; Furlan, Raffaello; Barbic, Franca; Catai, Aparecida Maria; Silva, Ester (2017). "The degree of cardiac baroreflex involvement during active standing is associated with the quality of life in fibromyalgia patients". PloS One. 12 (6): e0179500. doi:10.1371/journal.pone.0179500. ISSN 1932-6203. PMID 28614420.
- ↑ Bäckryd, Emmanuel; Tanum, Lars; Lind, Anne-Li; Larsson, Anders; Gordh, Torsten (2017). "Evidence of both systemic inflammation and neuroinflammation in fibromyalgia patients, as assessed by a multiplex protein panel applied to the cerebrospinal fluid and to plasma". Journal of Pain Research. 10: 515–525. doi:10.2147/JPR.S128508. ISSN 1178-7090.
- ↑ 40.0 40.1 40.2 40.3 López-Solà, Marina; Woo, Choong-Wan; Pujol, Jesus; Deus, Joan; Harrison, Ben J.; Monfort, Jordi; Wager, TorD. (2017). "Towards a neurophysiological signature for fibromyalgia". Pain. 158 (1): 34–47. doi:10.1097/j.pain.0000000000000707. ISSN 1872-6623. PMID 27583567.
- ↑ Häuser, Winfried; Perrot, Serge; Sommer, Claudia; Shir, Yoram; Fitzcharles, Mary-Ann (May 2017). "Diagnostic confounders of chronic widespread pain: not always fibromyalgia". Pain Reports. 2 (3): e598. doi:10.1097/PR9.0000000000000598. ISSN 2471-2531. PMC 5741304. PMID 29392213.
- ↑ Boomershine, Chad S.; Koch, Todd A.; Morris, David (2018). "A Blinded, Randomized, Placebo-Controlled Study to Investigate the Efficacy and Safety of Ferric Carboxymaltose in Iron-Deficient Patients with Fibromyalgia". Rheumatology and Therapy. 5 (1): 271–281. doi:10.1007/s40744-017-0088-9. ISSN 2198-6576. PMID 29149437.
- ↑ 43.0 43.1 Wolfe, Frederick; Walitt, Brian; Rasker, Johannes J.; Häuser, Winfried (July 15, 2018). "Primary and Secondary Fibromyalgia Are The Same: The Universality of Polysymptomatic Distress". The Journal of Rheumatology. 46 (2): 204–212. ISSN 0315-162X. PMID 30008459.
- ↑ 44.0 44.1 Zhang, Zhifang; Feng, Jinong; Mao, Allen; Le, Keith; Placa, Deirdre La; Wu, Xiwei; Longmate, Jeffrey; Marek, Claudia; Amand, R. Paul S t (June 21, 2018). "SNPs in inflammatory genes CCL11, CCL4 and MEFV in a fibromyalgia family study". PLOS ONE. 13 (6): e0198625. doi:10.1371/journal.pone.0198625. ISSN 1932-6203. PMID 29927949.
- ↑ Wu, Yu-Lin; Huang, Chun-Jen; Fang, Su-Chen; Ko, Ling-Hsin; Tsai, Pei-Shan (2018). "Cognitive Impairment in Fibromyalgia: A Meta-Analysis of Case-Control Studies". Psychosomatic medicine. 80 (5): 432–438. PMID 29528888.
- ↑ Bourgaize, Sheryl; Newton, Genevieve; Kumbhare, Dinesh; Srbely, John (2018). "A comparison of the clinical manifestation and pathophysiology of myofascial pain syndrome and fibromyalgia: implications for differential diagnosis and management" (PDF). Journal of the Canadian Chiropractic Assoc. 62 (1): 26–41.
- ↑ 47.0 47.1 Albrecht, Daniel S.; Forsberg, Anton; Sandstrom, Angelica; Bergan, Courtney; Kadetoff, Diana; Protsenko, Ekaterina; Lampa, Jon; Lee, Yvonne C.; Höglundi, Caroline Olgar t (September 14, 2018). Catana, Ciprian; Cervenka, Simon; Akeju, Oluwaseun; Lekander, Mats; Cohen, George; Halldin, Christer; Taylor, Norman; Kim, Minhae; Hooker, Jacob M.; Loggia, Marco L. "Brain glial activation in fibromyalgia – A multi-site positron emission tomography investigation". Brain, Behavior, and Immunity. 75: 72–83. doi:10.1016/j.bbi.2018.09.018. ISSN 0889-1591. PMC 6541932. PMID 30223011.
- ↑ Martucci, Katherine T; Weber, Kenneth A; Mackey, Sean C (October 3, 2018). "Altered Cervical Spinal Cord Resting State Activity in Fibromyalgia". Arthritis & Rheumatology. 71 (3): 441–450. doi:10.1002/art.40746. ISSN 2326-5191.
- ↑ 49.0 49.1 49.2 Wolfe, Frederick; Walitt, Brian; Perrot, Serge; Rasker, Johannes J.; Häuser, Winfried (September 13, 2018). "Fibromyalgia diagnosis and biased assessment: Sex, prevalence and bias". PLOS ONE. 13 (9): e0203755. doi:10.1371/journal.pone.0203755. ISSN 1932-6203. PMID 30212526.
- ↑ 50.0 50.1 Davis, Fred; Gostine, Mark; Roberts, Bradley; Risko, Rebecca; Cappelleri, Joseph; Sadosky, Alesia (2018). "Characterizing classes of fibromyalgia within the continuum of central sensitization syndrome". Journal of Pain Research. 11: 2551–2560. doi:10.2147/JPR.S147199. ISSN 1178-7090.
- ↑ 51.0 51.1 Natelson, Benjamin H. (February 19, 2019). "Myalgic Encephalomyelitis/Chronic Fatigue Syndrome and Fibromyalgia: Definitions, Similarities, and Differences". Clinical Therapeutics. 41 (4): 612. doi:10.1016/j.clinthera.2018.12.016. ISSN 0149-2918. PMID 30795933.
- ↑ Harte, Steven E.; Harris, Richard E.; Clauw, Daniel J. (2018). "The neurobiology of central sensitization". Journal of Applied Biobehavioral Research. 23 (2): e12137. doi:10.1111/jabr.12137. ISSN 1751-9861.
- ↑ 53.0 53.1 53.2 Rodriguez-Saona, Luis; Giusti, M. Mónica; Buffington, Charles A. T.; Yu, Lianbo; Madiai, Francesca; Pujolras, Marcal Plans; Sigurdson, Gregory T.; Aykas, Didem P.; Hackshaw, Kevin V. (December 6, 2018). "Metabolic fingerprinting for diagnosis of fibromyalgia and other rheumatologic disorders". Journal of Biological Chemistry: jbc.RA118.005816. doi:10.1074/jbc.RA118.005816. ISSN 0021-9258. PMID 30523152.
- ↑ Pappolla, Miguel A.; Manchikanti, Laxmaiah; Andersen, Clark R.; Greig, Nigel H.; Ahmed, Fawad; Fang, Xiang; Seffinger, Michael A.; Trescot, Andrea M. (May 6, 2019). "Is insulin resistance the cause of fibromyalgia? A preliminary report". PLOS ONE. 14 (5): e0216079. doi:10.1371/journal.pone.0216079. ISSN 1932-6203. PMC 6502334. PMID 31059525.
- ↑ Grayston, Rebecca; Czanner, Gabriela; Elhadd, Kareim; Goebel, Andreas; Frank, Bernhard; Üçeyler, Nurcan; Malik, Rayaz A; Alam, Uazman (April 1, 2019). "A systematic review and meta-analysis of the prevalence of small fiber pathology in fibromyalgia: Implications for a new paradigm in fibromyalgia etiopathogenesis". Seminars in Arthritis and Rheumatism. 48 (5): 933–940. doi:10.1016/j.semarthrit.2018.08.003. ISSN 0049-0172.
- ↑ Bidonde, Julia; Busch, Angela J; Schachter, Candice L; Webber, Sandra C; Musselman, Kristin E; Overend, Tom J; Góes, Suelen M; Dal Bello-Haas, Vanina; Boden, Catherine (May 24, 2019). Cochrane Musculoskeletal Group (ed.). "Mixed exercise training for adults with fibromyalgia". Cochrane Database of Systematic Reviews. doi:10.1002/14651858.CD013340. PMC 6931522. PMID 31124142.
- ↑ van de Donk, Tine; Niesters, Marieke; Kowal, Mikael A.; Olofsen, Erik; Dahan, Albert; van Velzen, Monique (April 2019). "An experimental randomized study on the analgesic effects of pharmaceutical-grade cannabis in chronic pain patients with fibromyalgia". Pain. 160 (4): 860–869. doi:10.1097/j.pain.0000000000001464. ISSN 0304-3959. PMC 6430597. PMID 30585986.
- ↑ Silva, Ana Rita; Bernardo, Alexandra; Costa, João; Cardoso, Alexandra; Santos, Paula; de Mesquita, Maria Fernanda; Vaz Patto, José; Moreira, Pedro; Silva, Maria Leonor (March 29, 2019). "Dietary interventions in fibromyalgia: a systematic review". Annals of Medicine. 51 (sup1): 2–14. doi:10.1080/07853890.2018.1564360. ISSN 0785-3890. PMC 7888848. PMID 30735059.
- ↑ Yeh, Shu-Wei; Hong, Chien-Hsiung; Shih, Ming-Chieh; Tam, Ka-Wai; Huang, Yao-Hsien; Kuan, Yi-Chun (May 2019). "Low-Level Laser Therapy for Fibromyalgia: A Systematic Review and Meta-Analysis". Pain Physician. 22 (3): 241–254. ISSN 2150-1149. PMID 31151332.
- ↑ Arnold, Lesley M.; Bennett, Robert M.; Crofford, Leslie J.; Dean, Linda E.; Clauw, Daniel J.; Goldenberg, Don L.; Fitzcharles, Mary-Ann; Paiva, Eduardo S.; Staud, Roland (June 1, 2019). "AAPT Diagnostic Criteria for Fibromyalgia". The Journal of Pain. 20 (6): 611–628. doi:10.1016/j.jpain.2018.10.008. ISSN 1526-5900. PMID 30453109.
- ↑ Erdrich, Sharon; Hawrelak, Jason A.; Myers, Stephen P.; Harnett, Joanna E. (March 20, 2020). "Determining the association between fibromyalgia, the gut microbiome and its biomarkers: A systematic review". BMC Musculoskeletal Disorders. 21 (1): 181. doi:10.1186/s12891-020-03201-9. ISSN 1471-2474. PMC 7083062. PMID 32192466.
- ↑ Erdrich, S; Hawrelak, JA; Myers, SP; Harnett, JE (December 8, 2020). "A systematic review of the association between fibromyalgia and functional gastrointestinal disorders". Therapeutic Advances in Gastroenterology. 13. doi:10.1177/1756284820977402.
- ↑ Ambrus, Julian L.; Isackson, Paul; Moore, Molly; Butsch, John; Balos, Lucia (February 18, 2020). "Investigating Fatigue and Exercise Intolerance in a University Immunology Clinic". Archives of Rheumatology & Arthritis Research. 1 (1): 1–8.
- ↑ D'Onghia, Martina; Ciaffi, Jacopo; Lisi, Lucia; Mancarella, Luana; Ricci, Susanna; Stefanelli, Nicola; Meliconi, Riccardo; Ursini, Francesco (April 1, 2021). "Fibromyalgia and obesity: A comprehensive systematic review and meta-analysis". Seminars in Arthritis and Rheumatism. 51 (2): 409–424. doi:10.1016/j.semarthrit.2021.02.007. ISSN 0049-0172.
- ↑ Sleurs, David; Tebeka, Sarah; Scognamiglio, Claire; Dubertret, Caroline; Le Strat, Yann (2020). "Comorbidities of self-reported fibromyalgia in United States adults: A cross-sectional study from The National Epidemiological Survey on Alcohol and Related Conditions (NESARC-III)". European Journal of Pain. 24 (8): 1471–1483. doi:10.1002/ejp.1585. ISSN 1532-2149.
- ↑ Lloyd, Donna M.; Wittkopf, Priscilla G.; Arendsen, Laura J.; Jones, Anthony K. P. (November 2020). "Is Transcranial Direct Current Stimulation (tDCS) Effective for the Treatment of Pain in Fibromyalgia? A Systematic Review and Meta-Analysis". The Journal of Pain. 21 (11–12): 1085–1100. doi:10.1016/j.jpain.2020.01.003. ISSN 1528-8447. PMID 31982685.
- ↑ Conde-Antón, Á; Hernando-Garijo, I.; Jiménez-Del-Barrio, S.; Mingo-Gómez, M.T.; Medrano-de-la-Fuente, R.; Ceballos-Laita, L. (October 15, 2020). "Effects of transcranial direct current stimulation and transcranial magnetic stimulation in patients with fibromyalgia. A systematic review". Neurologia (Barcelona, Spain): S0213–4853(20)30278–4. doi:10.1016/j.nrl.2020.07.024. ISSN 2173-5808. PMID 33071017.
- ↑ Cordón, B.; Orduna, E.; Viladés, E.; Garcia-Martin, E.; Garcia-Campayo, J.; Puebla-Guedea, M.; Polo, V.; Larrosa, J.M.; Pablo, L.E. (July 2, 2021). "Analysis of Retinal Layers in Fibromyalgia Patients with Premium Protocol in Optical Tomography Coherence and Quality of Life". Current Eye Research. 0 (0): 1–11. doi:10.1080/02713683.2021.1951301. ISSN 0271-3683. PMID 34213409.
- ↑ Hackshaw, Kevin V. (February 2021). "The Search for Biomarkers in Fibromyalgia". Diagnostics. 11 (2): 156. doi:10.3390/diagnostics11020156. PMC 7911687. PMID 33494476.
- ↑ Pappolla, Miguel A.; Manchikanti, Laxmaiah; Candido, KennethD.; Grieg, Nigel; Seffinger, Michael; Ahmed, Fauwad; Fang, Xiang; Andersen, Clark; Trescot, Andrea M. (March 2021). "Insulin Resistance is Associated with Central Pain in Patients with Fibromyalgia". Pain Physician. 24 (2): 175–184. ISSN 2150-1149. PMID 33740353.
- ↑ Pae, Chi-Un; Luyten, Patrick; Marks, David M.; Han, Changsu; Park, Sung-Hwan; Patkar, Ashwin A.; Masand, Prakash S.; Houdenhove, Boudewijn Van (August 1, 2008). "The relationship between fibromyalgia and major depressive disorder: a comprehensive review". Current Medical Research and Opinion. 24 (8): 2359–2371. doi:10.1185/03007990802288338. ISSN 0300-7995. PMID 18606054.
- ↑ Jensen, Karin B.; Petzke, Frank; Carville, Serena; Fransson, Peter; Marcus, Hanke; Williams, Steven C.R.; Choy, Ernest; Mainguy, Yves; Gracely, Richard (2010). "Anxiety and depressive symptoms in fibromyalgia are related to poor perception of health but not to pain sensitivity or cerebral processing of pain". Arthritis & Rheumatism. 62 (11): 3488–3495. doi:10.1002/art.27649. ISSN 1529-0131.
- ↑ Ablin, Jacob N.; Buskila, Dan; Van Houdenhove, Boudewijn; Luyten, Patrick; Atzeni, Fabiola; Sarzi-Puttini, Piercarlo (June 2012). "Is fibromyalgia a discrete entity?". Autoimmunity Reviews. 11 (8): 585–588. doi:10.1016/j.autrev.2011.10.018. ISSN 1568-9972.
- ↑ 74.0 74.1 Malin, Katrina; Littlejohn, Geoffrey O (September 7, 2012). "Personality and Fibromyalgia Syndrome". The Open Rheumatology Journal. 6: 273–285. doi:10.2174/1874312901206010273. ISSN 1874-3129. PMID 23002409.
- ↑ Theoharides, Theoharis C.; Stewart, Julia M.; Hatziagelaki, Erifili; Kolaitis, Gerasimos (2015). "Brain "fog," inflammation and obesity: key aspects of neuropsychiatric disorders improved by luteolin". Frontiers in Neuroscience. 9: 225. doi:10.3389/fnins.2015.00225. ISSN 1662-4548. PMID 26190965.
- ↑ Efrati, Shai; Golan, Haim; Bechor, Yair; Faran, Yifat; Daphna-Tekoah, Shir; Sekler, Gal; Fishlev, Gregori; Ablin, Jacob N.; Bergan, Jacob; Volkov, Olga; Friedman, Mony; Ben-Jacob, Eshel; Buskila, Dan (May 26, 2015). "Hyperbaric Oxygen Therapy Can Diminish Fibromyalgia Syndrome – Prospective Clinical Trial". PLOS ONE. 10 (5): e0127012. doi:10.1371/journal.pone.0127012. ISSN 1932-6203. PMID 26010952.
- ↑ Hyland, Michael E; Hinton, Claire; Hill, Charlotte; Whalley, Ben; Jones, Rupert CM; Davies, Anthony F (July 8, 2016). "Explaining unexplained pain to fibromyalgia patients: finding a narrative that is acceptable to patients and provides a rationale for evidence based interventions". British Journal of Pain. 10 (3): 156–161. doi:10.1177/2049463716642601. ISSN 2049-4637. PMID 27583142.
- ↑ Wolfe, Frederick; Walitt, Brian (October 15, 2016). "Fibromyalgia: A Short Commentary" (PDF). Journal of Headache & Pain Management. 1 (3): 27. doi:10.4172/2472-1913.100027. ISSN 2472-1913.
- ↑ "Chronic pain researchers to expand work with $7.5M award from NIH | Michigan Medicine". uofmhealth.org. October 17, 2016. Retrieved August 9, 2018.
- ↑ Black, Rachel (June 20, 2018). "NIH Announces Precision Medicine Initiative - Bateman Horne Center". Bateman Horne Center. Retrieved August 9, 2018.
- ↑ "National Institutes of Health (NIH) — All of Us". allofus.nih.gov. Retrieved August 9, 2018.


![Fig 1. Fibromyalgia Glial Activation Voxelwise group differences in [11C]PBR28 VT. A](/w/images/thumb/b/b5/Fibromyalgia_Glial_Activation_Voxelwise_group_differences_in_11CPBR28_VT._A_Fig._1.jpg/220px-Fibromyalgia_Glial_Activation_Voxelwise_group_differences_in_11CPBR28_VT._A_Fig._1.jpg)
![Fig. 2. Fibromyalgia Glial Activation Voxelwise group differences in [11C]PBR28 SUVR A](/w/images/thumb/e/ed/Fibromyalgia_Glial_Activation_Voxelwise_group_differences_in_11CPBR28_SUVR_A._Fig._2.jpg/220px-Fibromyalgia_Glial_Activation_Voxelwise_group_differences_in_11CPBR28_SUVR_A._Fig._2.jpg)
![Fig 4. Fibromyalgia Glial Cells Associations between [11C]PBR28 SUVR and clinical variables](/w/images/thumb/3/39/Fibromyalgia_Glial_Cells_Associations_between_11CPBR28_SUVR_and_clinical_variables._Fig._4.jpg/130px-Fibromyalgia_Glial_Cells_Associations_between_11CPBR28_SUVR_and_clinical_variables._Fig._4.jpg)
![Fig. 5. Fibromyalgia Glial Cells Absence of group differences in [11C]-L-deprenyl-D2 λk3](/w/images/thumb/1/12/Fibromyalgia_Glial_Cells_Absence_of_group_differences_in_11C-L-deprenyl-D2_%CE%BBk3._Fig._5.jpg/220px-Fibromyalgia_Glial_Cells_Absence_of_group_differences_in_11C-L-deprenyl-D2_%CE%BBk3._Fig._5.jpg)