- This page was created by volunteers like you!
- Help us make it even better. To learn more about contributing to MEpedia, click here.
- Join the movement
- Visit #MEAction to find support or take action. Donate today to help us improve and expand this project.
Eicosanoid
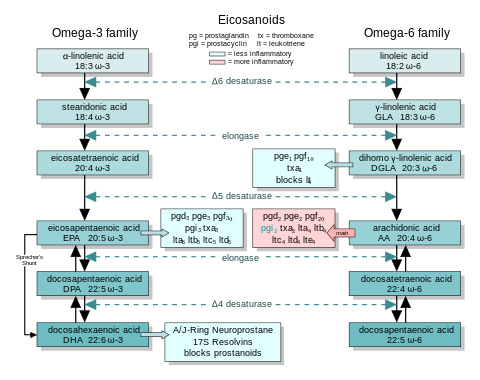
Eicosanoids are signaling molecules made from the long chain polyunsaturated fatty acids (PUFAs) eicosapentaenoic acid (EPA), dihomo-gamma-linolenic acid (DGLA) and especially arachidonic acid (AA).
Like cytokines and inflammasomes, they play an important role in the initiation and resolution of immune responses to infection and injury. Their complex role in inflammation and homeostasis is not well understood.
Types of eicosanoids
Eicosanoids include leukotrienes, eoxins and three types of prostanoids – prostaglandins, prostacyclins and thromboxanes.
Eicosanoids derived from omega 6 fatty acids tend to be pro-inflammatory while those derived from omega 3 fatty acids tend to be anti-inflammatory or perhaps more accurately, less active.[citation needed]
Eicosanoids are also related to docosanoids, signaling molecules derived primarily from docosahexaenoic acid (DHA) and resolvins and lipoxins, signaling molecules that induce the resolution of inflammation following acute infection or injury that are made from EPA and EHA.
Biosynthesis
Eicosanoids are made from the oxidation of arachidonic acid and other PUFAs by cyclooxygenase (COX), lipoxygenase (LOX) and cytochrome P450 (CYP) enzymes from cell membranes or via free radicals. [1]
The majority of eicosanoids require arachidonic acid, which is cleaved from cell membranes by phospholipase A2 (PLA2) enzymes.
Most cells produce insignificant amount of eicosanoids under normal conditions and produce a small number of specific eicosanoids when exposed to stimuli that activate PLA2.
Function
Eicosanoids are involved in vasodilation and vasoconstriction, promotion of sleep, pain and fever. They pay a role in up- or down-regulating inflammatory cytokines.
What eicosanoids cells produce and their effects depend on the type of cell, the tissue in which that cell is found, and the cell's activation state. For example, those produced via the COX enzyme pathway generate the symptoms commonly associated with inflammation: heat, swelling, redness, and pain. Those produced via the LOX pathway tend to be associated with the leukotrienes involved in allergy and asthma. The same prostaglandin that causes pain signaling in the brain can lead to a decrease in inflammation in other parts of the body.[2]
Medical applications
NSAIDs
Non-steroidal anti-inflammatory drugs like aspirin relieve pain, swelling and fever by inhibiting the receptors for leukotrienes, for example, or by inhibiting COX enzymes.[3]
Inhibition of Omega 6 products by Omega 3 supplementation
Omega 3 and Omega 6 derived eicosanoids compete with each other in three ways: displacement (dietary Omega 3 decreases tissue concentrations of AA), competitive inhibition (DGLA and EPA compete with AA for enzymes), and counteraction (some DGLA and EPA-derived eicosanoids counteract their AA derived counterparts).
Omega 3 supplementation is commonly prescribed for the treatment of inflammatory and cardiovascular disease because of the capacity of EPA and DHA to inhibit arachidonic acid metabolism by the COX1 pathway (but less so by COX2).[4]

