Central sensitization
Central sensitization (CS) refers to an “increased responsiveness of nociceptive neurons in the central nervous system to their normal or subthreshold afferent input.”[1] Clinically this corresponds with a heightened perception of pain stimuli (hyperalgesia) or the experience of pain after normally innocuous stimuli (allodynia).[2] Some researchers speculate central sensitization to be the explanatory mechanism behind various unexplained medical disorders that have chronic pain as a dominant feature.[3] Preliminary evidence suggests central sensitization to be involved in the symptomatology of ME/CFS.[4]
History[edit | edit source]
Secondary hyperalgesia[edit | edit source]
In 1950, Hardy and colleagues proposed that there were two types of hyperalgesia.[5] Primary hyperalgesia refers to pain sensitivity at the site of an injury, while secondary hyperalgesia refers to enhanced sensation in surrounding undamaged tissues, sometimes in remote sites distant from the injury. Hardy and colleagues speculated the former to be mediated by peripheral mechanisms, while the latter was suspected to be the result of "a central excitatory state", involving lasting changes in the responsiveness of the central nervous system.[6]
Decades went by before this hypothesis could be corroborated by experimental research. In 1965 Mendell and Wall reported that repetitive C-fiber stimulation at low frequency results in a progressive increase of electoral discharge in cat dorsal horn neurons.[7] They called this pattern of activity “the wind-up of a cell”.[8] Though wind-up demonstrated synaptic plasticity, the changes in the neuron did not last beyond the stimulation that incited it.
In 1983 Clifford Woolf and colleagues demonstrated a more lasting form of central neural plasticity.[9] After heat-induced inflammatory lesions at a rat knee joint, an enhanced responsiveness was seen in undamaged muscles surrounding the injury site. According to Woolf, "a local anesthetic block of the site of the peripheral injury did not result in collapse of the expanded receptive fields: The change was autonomous once it was triggered by the peripheral input."[10] This provided evidence of lasting changes in excitability of the central nervous system. Referring to this phenomenon, Woolf and colleagues first used the term central sensitization in the literature in 1989.[11]
In 1991, LaMotte and colleagues were the first to demonstrate central sensitization in human volunteers.[12] They used an injection of capsaicin, the active and painful component of chili peppers, to elicit hyperalgesia in their test subjects. Anesthetizing the region where capsaicin was injected was insufficient to block hyperalgesia. However, if the skin region was anesthetized prior to capsaicin injection, hyperalgesia does not develop.[6] This clearly demonstrated it to be crucial for the development of hyperalgesia, that initial noxious input reaches the central nervous system. Once developed, however hyperalgesia became “only partially dependent on peripheral neural activity originating at the site of injury.”
Inflation of the central sensitization concept[edit | edit source]
These experiments referred to central sensitization as an activity-dependent increase in the excitability of spinal neurons. It was related to peripheral tissue damage and mostly confined to the area surrounding the site of injury.[13] Though the secondary hyperalgesia it elicited lasted beyond the initial stimulus, this effect was usually short-lived and sometimes disappeared within the time-span of a day.[14]
Since then the concept of central sensitization has gone through a significant expansion.[15] It became widespread, lasting and unrelated to an identifiable nociceptive input form the periphery. Clifford Woolf who championed the broadening of the definition, now defines central sensitization as the “genus of all forms of pain sensitization that arise within the central nervous system”.[16] Woolf argues that the increase in excitability of the spinal cord he discovered in the 1980s represented only one example of what should be regarded as central sensitization.
Central sensitivity syndromes[edit | edit source]
The main rationale behind the expansion of the concept of central sensitivity came from clinical practice. Some researchers[17][18] speculated that central sensitization might elucidate several of the so-called ‘medically unexplained syndromes (MUS)’. Not only is there a significant overlap between these syndromes, but patients who suffer from it usually have a wide array of symptoms related to chronic pain. This suggested a common, previously unrecognized mechanism involving lowered thresholds to noxious stimuli, to be behind the expression of MUS.[19] In 2000 Muhammad Yunus suggested to group these disorders under the unifying concept of central sensitivity syndromes (CSS).[20] In Yunus’ vision central sensitization could explain not only the widespread and lasting hyperalgesia these patients suffered, but also a hypersensitivity to other environmental stimuli such as sounds, chemicals and light. Central sensitization was thus extended beyond the somatosensory system.[15]
The physiological mechanism[edit | edit source]
The physiology of central sensitization involves the activation of unmyelinated C-fibers that release excitatory neuropeptides such as glutamate, tachykinins and substance P in the dorsal horn of the spinal cord.[10] A primary role is played by the neurotransmitter glutamate which activates N-methyl-D-aspartic acid (NMDA) receptors. Normally, the ion channel of these NMDA-receptors is blocked by a magnesium ion, but the block can be removed by a depolarization of the cell leading to an influx of calcium, which leads to further depolarization. These changes cause an escalation of hyperexcitability of spinal cord neurons, giving rise to a hypersensitivity to noxious stimuli.[21][22] Nitric oxide (NO) also plays a role in CS as it has been shown to modulate neuron excitability through multiple mechanisms.[23]
Criteria for the classification of central sensitization pain[edit | edit source]
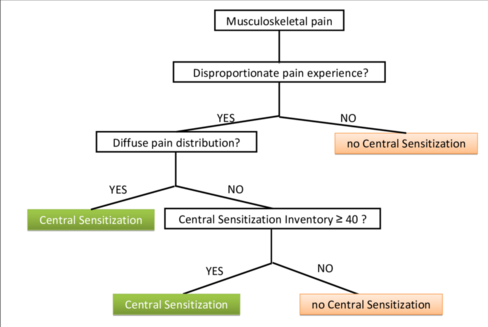
In 2014 a consensus paper was published by 18 experts from 7 different countries that set out criteria for the classification of central sensitization pain.[24] After neuropathic pain has been ruled out, the criteria advise to assess if the severity of pain is “disproportionate to the nature and extent of injury and pathology”. This is an obligatory criterion; if pain is not disproportionate, then it doesn’t involve CS.
Secondly it is proposed to look at the pain distribution; if pain is widespread and diffuse then the clinician can diagnose CS in his patient. If this is not the case, then the clinician can use the Central Sensitization Inventory (CSI), a questionnaire that has been developed to assess CS and mostly looks at secondary symptoms like sensitivity to light, poor sleep and concentration problems. If the patient scores 40 or more on the CSI, then the diagnosis of CS should be made.
Remarkably, psychological aspects such as catastrophizing, somatization and hypervigilance – considered by some to be central to CS – are not included in the criteria. While the authors acknowledge the importance of these maladaptive psychosocial factors, they do not consider them to be unique to central sensitization as they are often present in other chronic pain patients as well.
Evidence for central sensitization in ME/CFS[edit | edit source]
Pain thresholds and hyperalgesia[edit | edit source]
Various quantitative sensory tests (QST) can be used to evaluate if the CNS overreacts to stimuli and the presence of CS is to be suspected.[25] One method involves measuring pain thresholds all over the body with an algometer.
The Belgian Pain in Motion research group tested this in 30 ME/CFS who suffered from chronic pain. Pain pressure thresholds were significantly lower compared to those of the control group, also when pain-free areas of the body were tested (secondary hyperalgesia).[26] In an additional study it was shown that ME/CFS patients experienced more pain following heat stimuli.[27] In a large Norwegian study involving 120 adolescent with ME/CFS, pain pressure thresholds were significantly lower in patients compared to healthy controls.[28]
Other studies yielded conflicting results. Using cold pressor tests, Schmaling et al. did not find any differences in pain thresholds between ME/CFS patients and healthy controls.[29] The same finding was reported by Buchwald and colleagues in a study involving 15 twin pairs discordant for CFS.[30] An Italian group of the D’Annuzio University of Chieti found pain thresholds in the skin and subcutis to be normal in ME/CFS.[31] They did however find hyperalgesia in the muscles of these patients. Because a number of “anatomical muscle alterations” were discovered, the authors speculated the hyperalgesia to be caused by peripheral instead of central mechanisms.
Wind-up and temporal summation[edit | edit source]
To assess pain facilitation, researchers can test temporal summation of second pain. This refers to the process where neurons of the CNS react to repeated stimuli with an increased response. If one quickly repeats a fixed noxious stimulus 10 times, the last one will be experienced as more painful than the first. Researchers can measure the amount of ‘wind-up’ of the neurons by looking at the difference between the first and the last stimulus. In chronic pain conditions like fibromyalgia, that difference is greater than in normal controls, suggesting these patients experience a heightened form of temporal summation (TS). Collin et al. tested this procedure in 48 ME/CFS patients, but the results were ambiguous. There was only a difference in wind-up compared to control subjects if the pain stimuli were administered to the finger and not to the shoulder.[32] Testing of temporal summation was part of the procedure in three other studies without it being the primary outcome measure. One study[33] found TS to be higher in ME/CFS patients than controls, while two others did not find significant differences.[34][35]
Conditioned pain modulation: pain inhibits pain[edit | edit source]
Central sensitization doesn’t necessarily involve an increased susceptibility to stimuli; it can also be caused by a defect in the inhibitory pain pathways of the body. One highly researched mechanism in this respect is called 'conditioned pain modulation'[36] (CPM; an older name is 'diffuse noxious inhibitory control'). This refers to the fact that pain in one area of the body can decrease pain in another area. The chronic pain in your back for example might lessen if you sprain your ankle because your brain will focus more on the new information and dampen the other pain stimuli it receives. Meeus & Nijs of the Pain in Motion group tested this using heat stimuli and reported that conditioned pain modulation was normal but delayed in ME/CFS patients.[27] In four other studies, [32][37][33][35] the same research group tested CPM using the pressure of an inflatable occlusion cuff as the conditioning stimulus. In all cases there were no significant differences between ME/CFS patients and healthy controls.
Endogenous pain inhibition after exercise[edit | edit source]
Another way to induce endogenous inhibition is to exercise. When healthy people exercise, their brain produces endorphins that increase pain thresholds. In some chronic pain patients like fibromyalgia and whiplash associated disorders, this endogenous pain inhibition response is defect and pain thresholds decrease shortly after exercise (i.e. they experience more pain while they should be feeling less). In 2004 Whiteside et al. first showed this defect in ME/CFS patients, though their study only involved 5 patients.[38] The Pain in Motion group confirmed these results in two of their studies.[39][40] While pain thresholds increased in normal controls they decreased in the ME/CFS patient group. As a caveat, one must note that these studies only included ME/CFS patients that were suffering from chronic pain while comorbid fibromyalgia (FM) was not assessed. It remains unclear if these results will also hold true in ME/CFS patients that do not have comorbid FM.[41]
Other findings[edit | edit source]
In 2015 Staud et al. found indirect evidence for sensitized fatigue pathways in ME/CFS. Patients underwent exhausting handgrip-exercises and showed higher increased fatigue ratings than healthy controls after muscle metabolites were trapped in forearm tissues. The fact that fatigue ratings returned to baseline rapidly after removing the forearm occlusion suggests that ME/CFS patients display an increased sensitivity to exercise metabolites.[42]
In 2009 Light et al. found an increase in metabolite detecting receptors in the white blood cells of ME/CFS patients after an exercise test - an increase that was not seen in controls.[43] Results were confirmed by three other studies.[44][45][46] The authors speculate this might reflect an increased sensitivity to fatigue pathways in ME/CFS:
“If these receptors are increased in CFS patients, it is possible that low levels of metabolites can activate leukocytes, and moderate exercise could increase the signal, thereby increasing cytokine levels that sensitize muscle sensory fatigue signaling afferents.”[43]
In 2002 Nijs et al. reported bronchial hyperesponsiveness (BHR) after a histamine provocation test in 77 ME/CFS patients out of a sample of 137. Further research into immune factors failed to show a link with IGE-mediated activation of mast cells and eosinophils as is seen in asthma patients, but there was a connection with increased cytotoxic T-cell count and BHR.[47] According to Nijs “the high prevalence of bronchial hyperresponsiveness can be viewed as another piece of evidence in support of central sensitisation in at least a large subset of the CFS population.”[4]
The research group of Jo Nijs was initially drawn to exploring central sensitization in ME/CFS because of increased nitric oxide (NO) levels in these patients, as reported by Kurup & Kurup in 2003.[48] Subsequent research however showed that NO concentrations were normal and unrelated to activity levels in 30 ME/CFS patients.[49]
Substance P is another element believed to be involved in central sensitization. Increased levels of Substance P in cerebrospinal fluid have been reported in patients with fibromyalgia[50][51] – the prototype of central sensitivity syndromes. A small Swedish study involving 15 patients found values of Substance P to be in the normal range in ME/CFS.[52]
Conclusion[edit | edit source]
Interpretations of these preliminary findings on central sensitization in ME/CFS have been discordant. In a 2012 review, Nijs & Meeus concluded that “mounting evidence supporting a role for central sensitisation in at least a large subset of the CFS population is currently available.”[4] Mohammed Yunus however omitted ME/CFS on his list of central sensitivity disorders in 2015, due to a lack of evidence:
“Despite the fact that chronic fatigue syndrome (CFS) (systemic exertion intolerance disease) clinically overlaps with other members of the CSS family, definitive evidence of CS in this disease (excluding those having pain) is lacking, and was, therefore, not included.”[41]
Treatment of central sensitization[edit | edit source]
Nijs & Meeus wrote two reviews[53][54] on the treatment of central sensitization. While it is advised to eliminate peripheral nociceptive input as this might sustain CS, the focus lies on medications that target the CNS. One example is acetaminophen (paracetamol) that reinforces the inhibitory serotonergic pathway. Meeus & Nijs tested this in ME/CFS patients with comorbid fibromyalgia. Although pain thresholds rose, there was no influence on temporal summation or conditioned pain modulation.[34]
Selective serotonin reuptake inhibitors (SSRI, such as fluoxetine) also activate the serotonergic descending pathways. In a 2011 study, Meeus & Nijs gave their test subjects intravenous SSRI (citalopram) but the trial had to be stopped prematurely since the medication gave too many side-effects.[55]
Opioids (morphine, codeine etc.) form another option, although these drugs are rather controversial because they can lead to addiction and cause selective pain sensitization. In 2017 Meeus & Nijs tested morphine and naloxone (an opioid antagonist) against a placebo, but the results were rather bleak:
“neither morphine nor naloxone influenced deep tissue pain, temporal summation or CPM. Therefore, these results suggest that the opioid system is not dominant in (enhanced) bottom-up sensitization (temporal summation) or (impaired) endogenous pain inhibition (CPM) in patients with CFS/FM or RA.”[33]
There are other therapeutic options to treat central sensitization like N-methyl-D-aspartate –receptor antagonists (e.g. ketamine), GABA-antagonists (e.g. pregabalin) or a ketogenic diet. Nijs & Meeus also propose exercise therapy and emphasize that a time-contingent approach is to be preferred in treating CS:
“A symptom-contingent approach may facilitate the brain in its production of nonspecific warning signs like pain, whereas a time-contingent approach may deactivate brain-orchestrated top-down pain facilitatory pathways.”[54]
The authors do however caution that this approach might not work in every CS-patient group:
“some patients with CS pain, including those with chronic whiplash associated disorders , chronic fatigue syndrome and fibromyalgia, are unable to activate endogenous analgesia following exercise. It remains to be established whether long-term exercise therapy accounting for the dysfunctional endogenous analgesia is able to ‘treat’ CS in these patients.”
Criticism[edit | edit source]
Central sensitization only involves pain[edit | edit source]
Several researchers have questioned the expansion of the concept of central sensitization. Per Hansson for example wrote that “a significant body of human experimental and clinical literature interprets a multitude of symptoms and signs as expressions of CS, to an extent that is not supported by current research evidence.”[13] A Belgian research group made the same argument:
“We argue that CS, as defined by the International Association for the Study of Pain, refers to changes in nociceptive neurons only and therefore cannot be applied to enhanced responses to stimuli other than nociceptive and/or pain. Moreover, the evidence for CS in widespread pain (other than secondary hyperalgesia) and many other conditions is scarce to absent.”[56]
Overly broad use of central sensitization[edit | edit source]
In its definition, the International Association for the Study of Pain warns against using a too broad use of the term (central) sensitization:
“This is a neurophysiological term that can only be applied when both input and output of the neural system under study are known, e.g., by controlling the stimulus and measuring the neural event. Clinically, sensitization may only be inferred indirectly from phenomena such as hyperalgesia or allodynia.”[1]
Phillips and Clauw suggest the use of other terms such as ‘central pain’ or ‘central augmentation’ instead of CS, given that the term CS was originally used in the context of a sustained peripheral noxious input in an experimental (not a clinical) setting.[57] Katsuhiro Toda questioned the need for CS-pain as a separate category next to neuropathic and nociceptive pain, as was suggested by the 2014 CS-criteria:
“[…] differentiation between lesion/disease and dysfunction in the central nervous system makes no sense. Parkinson’s disease and multiple sclerosis were functional diseases in the sixth century. In all likelihood, dysfunction of the central nervous system in patients with CS pain such as fibromyalgia will be lesion in the twenty-fourth century. Differentiating CS pain from neuropathic pain confuses clinical practice. CS pain should be included in (central) neuropathic pain.”[58]
A popular myth?[edit | edit source]
Cervero (2014) has questioned the popularity and widespread acceptance of central sensitization despite the limited evidence base.[59]
Cognitive-emotional sensitization[edit | edit source]
A related concept to CS is cognitive-emotional sensitization, as put forward by Jos Brosschot in 2002. In his theory sensitization is presented as a psychological concept, related to anxiety and cognitive bias. According to Brosschot “those who have an extreme concern about somatic disease will develop a cognitive bias for information related to somatic disease. This bias would be reflected in an activated cognitive network that guides the brain into early detection of all information related to patients’ concerns.”[60] A similar hypothesis was made by the Norwegians Olger Ursin and Hege Eriksen. In 2004 they suggested that “sensitization is the psychobiological mechanism explaining the individual differences in tolerance and acceptance of common health complaints.”[61]
Mohammed Yunus has criticized these mere psychological interpretations of (central) sensitization. He emphasizes that central sensitivity syndromes have an “objective pathology of neurochemistry and neuroimaging that explain many symptoms of CSS diseases”. The same argument was made by the authors of the 2014 CS-criteria, who wrote: “CS is not a disorder of the mind, but rather a disease of the brain and spinal cord.”
In 2015 Gracely & Schweinhardt presented an original hypothesis. They suggest that the symptoms of CSS should not be regarded as a direct consequence of a disease state or a pathological process but rather as an adaptive reaction of the body, similar to a sickness response. In their view the purpose of CS is to promote quiescence by inhibiting and limiting the normal range of behavior, which would lead to an increased survival from an evolutionary point of view.[15]
Notable articles[edit | edit source]
- 1996, Windup and central sensitization are not equivalent[7] (Abstract)
- 2007, Fibromyalgia and Overlapping Disorders: The Unifying Concept of Central Sensitivity Syndromes[3] (Full text)
- 2014, Central sensitization and visceral hypersensitivity: Facts and fictions[59] (Full text)
- 2015, Editorial Review (Thematic Issue: An Update on Central Sensitivity Syndromes and the Issues of Nosology and Psychobiology)[41] (Full text)
Ongoing Studies[edit | edit source]
- Brain in Pain III – The neurophysiology of chronic fatigue syndrome (Bourke, White) Centre for Psychiatry (ending later 2016, Peter White)
Learn more[edit | edit source]
See also[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 "IASP Terminology". International Association for the Study of Pain. Retrieved August 25, 2018.
- ↑ McAllister, Murray J. "What is Central Sensitization?". Retrieved August 25, 2018.
- ↑ 3.0 3.1 Yunus, Muhammad B. (June 2007). "Fibromyalgia and Overlapping Disorders: The Unifying Concept of Central Sensitivity Syndromes". Seminars in Arthritis and Rheumatism. 36 (6): 339–356. doi:10.1016/j.semarthrit.2006.12.009. ISSN 0049-0172.
- ↑ 4.0 4.1 4.2 Nijs, Jo; Meeus, Mira; Van Oosterwijck, Jessica; Ickmans, Kelly; Moorkens, Greta; Hans, Guy; De Clerck, Luc S. (July 27, 2011). "In the mind or in the brain? Scientific evidence for central sensitisation in chronic fatigue syndrome". European Journal of Clinical Investigation. 42 (2): 203–212. doi:10.1111/j.1365-2362.2011.02575.x. ISSN 0014-2972.
- ↑ Hardy, James D.; Wolff, Harold G.; Goodell, Helen (January 1, 1950). "Experimental Evidence on The Nature of Cutaneous Hyperalgesia". Journal of Clinical Investigation. 29 (1): 115–140. doi:10.1172/jci102227. ISSN 0021-9738.
- ↑ 6.0 6.1 Coderre, Terence J.; Katz, Joel; Vaccarino, Anthony L.; Melzack, Ronald (March 1993). "Contribution of central neuroplasticity to pathological pain: review of clinical and experimental evidence". Pain. 52 (3): 259–285. doi:10.1016/0304-3959(93)90161-h. ISSN 0304-3959.
- ↑ 7.0 7.1 Woolf, Clifford J. (August 1996). "Windup and central sensitization are not equivalent". Pain. 66 (2): 105–108. doi:10.1097/00006396-199608000-00001. ISSN 0304-3959.
- ↑ MENDELL, LORNE M.; WALL, PATRICKD. (April 1965). "Responses of Single Dorsal Cord Cells to Peripheral Cutaneous Unmyelinated Fibres". Nature. 206 (4979): 97–99. doi:10.1038/206097a0. ISSN 0028-0836.
- ↑ Woolf, Clifford J. (December 1983). "Evidence for a central component of post-injury pain hypersensitivity". Nature. 306 (5944): 686–688. doi:10.1038/306686a0. ISSN 0028-0836.
- ↑ 10.0 10.1 Latremoliere, Alban; Woolf, Clifford J. (September 2009). "Central Sensitization: A Generator of Pain Hypersensitivity by Central Neural Plasticity". The Journal of Pain. 10 (9): 895–926. doi:10.1016/j.jpain.2009.06.012. ISSN 1526-5900.
- ↑ Woolf, C.J.; Thompson, S.W.; King, A.E. (1988–1989). "Prolonged primary afferent induced alterations in dorsal horn neurones, an intracellular analysis in vivo and in vitro". Journal De Physiologie. 83 (3): 255–266. ISSN 0021-7948. PMID 3272296.
- ↑ LaMotte, R.H.; Shain, C.N.; Simone, D.A.; Tsai, E.F. (July 1991). "Neurogenic hyperalgesia: psychophysical studies of underlying mechanisms". Journal of Neurophysiology. 66 (1): 190–211. doi:10.1152/jn.1991.66.1.190. ISSN 0022-3077.
- ↑ 13.0 13.1 Hansson, Per (October 2014). "Translational aspects of central sensitization induced by primary afferent activity: What it is and what it is not". Pain. 155 (10): 1932–1934. doi:10.1016/j.pain.2014.07.016. ISSN 0304-3959.
- ↑ Woolf, Clifford J. (March 2011). "Central sensitization: Implications for the diagnosis and treatment of pain". Pain. 152 (Supplement): S2–S15. doi:10.1016/j.pain.2010.09.030. ISSN 0304-3959.
- ↑ 15.0 15.1 15.2 Gracely, Richard; Schweinhardt, Petra (July 2, 2015). "Programmed Symptoms: Disparate Effects United by Purpose". Current Rheumatology Reviews. 11 (2): 116–130. doi:10.2174/1573397111666150619095125. ISSN 1573-3971.
- ↑ Woolf, Clifford J. (October 2014). "What to call the amplification of nociceptive signals in the central nervous system that contribute to widespread pain?". Pain. 155 (10): 1911–1912. doi:10.1016/j.pain.2014.07.021. ISSN 0304-3959.
- ↑ Yunus, Muhammad B. (June 2008). "Central Sensitivity Syndromes: A New Paradigm and Group Nosology for Fibromyalgia and Overlapping Conditions, and the Related Issue of Disease versus Illness". Seminars in Arthritis and Rheumatism. 37 (6): 339–352. doi:10.1016/j.semarthrit.2007.09.003. ISSN 0049-0172.
- ↑ Toda, Katsuhiro (January 2012). "The Term of Functional Somatic Syndrome Should be Changed to the Term of Central Sensitivity Syndrome". Pain Practice. 12 (1): 83–83. doi:10.1111/j.1533-2500.2011.00504.x. ISSN 1530-7085.
- ↑ Adams, Leah; Turk, Dennis (July 2, 2015). "Psychosocial Factors and Central Sensitivity Syndromes". Current Rheumatology Reviews. 11 (2): 96–108. doi:10.2174/1573397111666150619095330. ISSN 1573-3971.
- ↑ Yunus, Muhammad B. (2000). "Central sensitivity syndromes: a unified concept for fibromyalgia and other similar maladies". JIRA. 8: 27–33.
- ↑ Woolf, Clifford J.; Chong, Mun-Seng (August 1993). "Preemptive Analgesia—Treating Postoperative Pain by Preventing the Establishment of Central Sensitization". Anesthesia & Analgesia. 77 (2): 362–379. doi:10.1213/00000539-199377020-00026. ISSN 0003-2999.
- ↑ DeLeo, Joyce A.; Winkelstein, Beth A. (November 2002). "Physiology of Chronic Spinal Pain Syndromes". Spine. 27 (22): 2526–2537. doi:10.1097/00007632-200211150-00026. ISSN 0362-2436.
- ↑ Luo, Z. David; Cizkova, Dasa (December 2000). "The role of nitric oxide in nociception". Current Review of Pain. 4 (6): 459–466. doi:10.1007/s11916-000-0070-y. ISSN 1069-5850.
- ↑ Nijs, Jo; Torres-Cueco, Rafael; van Wilgen, C. Paul; Girbes, Enrique Lluh; Struyf, Filip; Roussel, Nathalie; van Oosterwijck, Jessica; Daenen, Liesbeth; Kuppens, Kevin (September 2014). "Applying modern pain neuroscience in clinical practice: criteria for the classification of central sensitization pain". Pain Physician. 17 (5): 447–457. ISSN 2150-1149. PMID 25247901.
- ↑ Staud, Roland (May 2012). "Abnormal endogenous pain modulation is a shared characteristic of many chronic pain conditions". Expert Review of Neurotherapeutics. 12 (5): 577–585. doi:10.1586/ern.12.41. ISSN 1473-7175.
- ↑ Meeus, Mira; Nijs, Jo; Huybrechts, Sven; Truijen, Steven (January 14, 2010). "Evidence for generalized hyperalgesia in chronic fatigue syndrome: a case control study". Clinical Rheumatology. 29 (4): 393–398. doi:10.1007/s10067-009-1339-0. ISSN 0770-3198.
- ↑ 27.0 27.1 Meeus, Mira; Nijs, Jo; Van de Wauwer, Naomi; Toeback, Linda; Truijen, Steven (October 2008). "Diffuse noxious inhibitory control is delayed in chronic fatigue syndrome: An experimental study". Pain. 139 (2): 439–448. doi:10.1016/j.pain.2008.05.018. ISSN 0304-3959.
- ↑ Winger, Anette; Kvarstein, Gunnvald; Wyller, Vegard Bruun; Sulheim, Dag; Fagermoen, Even; Småstuen, Milada Cvancarova; Helseth, Sølvi (October 2014). "Pain and pressure pain thresholds in adolescents with chronic fatigue syndrome and healthy controls: a cross-sectional study". BMJ Open. 4 (10): e005920. doi:10.1136/bmjopen-2014-005920. ISSN 2044-6055.
- ↑ Schmaling, Karen B.; Hamilos, Daniel L.; Diclementi, Jeannie D.; Jones, James F. (January 1998). "Pain Perception in Chronic Fatigue Syndrome". Journal of Chronic Fatigue Syndrome. 4 (3): 13–22. doi:10.1300/j092v04n03_03. ISSN 1057-3321.
- ↑ Ullrich, Philip M.; Afari, Niloofar; Jacobsen, Clemma; Goldberg, Jack; Buchwald, Dedra (February 7, 2007). "Cold Pressor Pain Sensitivity in Monozygotic Twins Discordant for Chronic Fatigue Syndrome". Pain Medicine. 0 (0): 070207140827002–???. doi:10.1111/j.1526-4637.2007.00277.x. ISSN 1526-2375.
- ↑ Vecchiet, Leonardo; Montanari, Giuseppe; Pizzigallo, Eligio; Iezzi, Sabina; de Bigontina, Paolo; Dragani, Luca; Vecchiet, Jacopo; Giamberardino, Maria Adele (April 1996). "Sensory characterization of somatic parietal tissues in humans with chronic fatigue syndrome". Neuroscience Letters. 208 (2): 117–120. doi:10.1016/0304-3940(96)12559-3. ISSN 0304-3940.
- ↑ 32.0 32.1 Collin, Simon M.; Nijs, Jo; Meeus, Mira; Polli, Andrea; Willekens, Barbara; Ickmans, Kelly (May 2017). "Endogenous Pain Facilitation Rather Than Inhibition Differs Between People with Chronic Fatigue Syndrome, Multiple Sclerosis, and Controls: An Observational Study". Pain Physician. 20 (4): E489–E497. ISSN 2150-1149. PMID 28535557.
- ↑ 33.0 33.1 33.2 Hermans, Linda; Nijs, Jo; Calders, Patrick; De Clerck, Luc; Moorkens, Greta; Hans, Guy; Grosemans, Sofie; Roman De Mettelinge, Tine; Tuynman, Joanna (November 15, 2017). "Influence of Morphine and Naloxone on Pain Modulation in Rheumatoid Arthritis, Chronic Fatigue Syndrome/Fibromyalgia, and Controls: A Double-Blind, Randomized, Placebo-Controlled, Cross-Over Study". Pain Practice. 18 (4): 418–430. doi:10.1111/papr.12613. ISSN 1530-7085.
- ↑ 34.0 34.1 Meeus, Mira; Ickmans, Kelly; Struyf, Filip; Hermans, Linda; Van Noesel, Kevin; Oderkerk, Jorinde; Declerck, Luc S.; Moorkens, Greta; Hans, Guy (March 2013). "Does acetaminophen activate endogenous pain inhibition in chronic fatigue syndrome/fibromyalgia and rheumatoid arthritis? A double-blind randomized controlled cross-over trial". Pain Physician. 16 (2): E61–70. ISSN 2150-1149. PMID 23511692.
- ↑ 35.0 35.1 Ickmans, Kelly; Meeus, Mira; De Kooning, Margot; Lambrecht, Luc; Pattyn, Nathalie; Nijs, Jo (September 2015). "Associations Between Cognitive Performance and Pain in Chronic Fatigue Syndrome: Comorbidity with Fibromyalgia Does Matter". Pain Physician. 18 (5): E841–852. ISSN 2150-1149. PMID 26431138.
- ↑ Kennedy, Donna L.; Kemp, Harriet I.; Ridout, Deborah; Yarnitsky, David; Rice, Andrew S.C. (November 2016). "Reliability of conditioned pain modulation". PAIN. 157 (11): 2410–2419. doi:10.1097/j.pain.0000000000000689. ISSN 0304-3959.
- ↑ Meeus, Mira; Ickmans, Kelly; Struyf, Filip; Hermans, Linda; Van Noesel, Kevin; Oderkerk, Jorinde; Declerck, Luc S.; Moorkens, Greta; Hans, Guy (March 2013). "Does acetaminophen activate endogenous pain inhibition in chronic fatigue syndrome/fibromyalgia and rheumatoid arthritis? A double-blind randomized controlled cross-over trial". Pain Physician. 16 (2): E61–70. ISSN 2150-1149. PMID 23511692.
- ↑ Whiteside, Alan; Hansen, Stig; Chaudhuri, Abhijit (June 2004). "Exercise lowers pain threshold in chronic fatigue syndrome". Pain. 109 (3): 497–499. doi:10.1016/j.pain.2004.02.029. ISSN 0304-3959.
- ↑ Meeus, M; Roussel, NA; Truijen, S (2010). "Reduced pressure pain thresholds in response to exercise in chronic fatigue syndrome but not in chronic low back pain: An experimental study". Journal of Rehabilitation Medicine. 42 (9): 884–890. doi:10.2340/16501977-0595. ISSN 1650-1977.
- ↑ Van Oosterwijck, J.; Nijs, J.; Meeus, M.; Lefever, I.; Huybrechts, L.; Lambrecht, L.; Paul, L. (March 3, 2010). "Pain inhibition and postexertional malaise in myalgic encephalomyelitis/chronic fatigue syndrome: An experimental study". Journal of Internal Medicine. 268 (3): 265–278. doi:10.1111/j.1365-2796.2010.02228.x. ISSN 0954-6820.
- ↑ 41.0 41.1 41.2 Yunus, Muhammad (July 2, 2015). "Editorial Review (Thematic Issue: An Update on Central Sensitivity Syndromes and the Issues of Nosology and Psychobiology)". Current Rheumatology Reviews. 11 (2): 70–85. doi:10.2174/157339711102150702112236. ISSN 1573-3971.
- ↑ Staud, Roland; Mokthech, Meriem; Price, Donald D.; Robinson, Michael E. (April 2015). "Evidence for sensitized fatigue pathways in patients with chronic fatigue syndrome". PAIN. 156 (4): 750–759. doi:10.1097/j.pain.0000000000000110. ISSN 0304-3959.
- ↑ 43.0 43.1 Light, Alan R.; White, Andrea T.; Hughen, Ronald W.; Light, Kathleen C. (October 2009). "Moderate exercise increases expression for sensory, adrenergic, and immune genes in chronic fatigue syndrome patients but not in normal subjects". The Journal of Pain: Official Journal of the American Pain Society. 10 (10): 1099–1112. doi:10.1016/j.jpain.2009.06.003. ISSN 1528-8447. PMC 2757484. PMID 19647494.
- ↑ Light, A.R.; Bateman, L.; Jo, D.; Hughen, R.W.; Vanhaitsma, T.A.; White, A.T.; Light, K.C. (January 2012). "Gene expression alterations at baseline and following moderate exercise in patients with Chronic Fatigue Syndrome and Fibromyalgia Syndrome". Journal of Internal Medicine. 271 (1): 64–81. doi:10.1111/j.1365-2796.2011.02405.x. ISSN 1365-2796. PMC 3175315. PMID 21615807.
- ↑ Meyer, Jacob D.; Light, Alan R.; Shukla, Sanjay K.; Clevidence, Derek; Yale, Steven; Stegner, Aaron J.; Cook, Dane B. (October 2013). "Post-exertion malaise in chronic fatigue syndrome: symptoms and gene expression". Fatigue: Biomedicine, Health & Behavior. 1 (4): 190–209. doi:10.1080/21641846.2013.838444. ISSN 2164-1846.
- ↑ White, Andrea T.; Light, Alan R.; Hughen, Ronald W.; Vanhaitsma, Timothy A.; Light, Kathleen C. (January 2012). "Differences in metabolite-detecting, adrenergic, and immune gene expression after moderate exercise in patients with chronic fatigue syndrome, patients with multiple sclerosis, and healthy controls". Psychosomatic Medicine. 74 (1): 46–54. doi:10.1097/PSY.0b013e31824152ed. ISSN 1534-7796. PMC 3256093. PMID 22210239.
- ↑ Nijs, Jo; De Becker, Pascale; De Meirleir, Kenny; Demanet, Christian; Vincken, Walter; Schuermans, Daniel; McGregor, Neil (April 2003). "Associations Between Bronchial Hyperresponsiveness and Immune Cell Parameters in Patients With Chronic Fatigue Syndrome". Chest. 123 (4): 998–1007. doi:10.1378/chest.123.4.998. ISSN 0012-3692.
- ↑ Nijs, Jo; Van de Velde, Bart; De Meirleir, Kenny (January 2005). "Pain in patients with chronic fatigue syndrome: Does nitric oxide trigger central sensitisation?". Medical Hypotheses. 64 (3): 558–562. doi:10.1016/j.mehy.2004.07.037. ISSN 0306-9877.
- ↑ Meeus, Mira; Van Eupen, Inge; Hondequin, Jasmien; DE Hauwere, Lieve; Kos, Daphne; Nijs, Jo (November 2010). "Nitric oxide concentrations are normal and unrelated to activity level in chronic fatigue syndrome: a case-control study". In Vivo (Athens, Greece). 24 (6): 865–869. ISSN 1791-7549. PMID 21164046.
- ↑ Russell, I. Jon; Orr, Malcolm D.; Littman, Bruce; Vipraio, Gilbert A.; Alboukrek, David; Michalek, Joel E.; Lopez, Yolanda; Mackillip, Fane (November 1994). "Elevated cerebrospinal fluid levels of substance p in patients with the fibromyalgia syndrome". Arthritis & Rheumatism. 37 (11): 1593–1601. doi:10.1002/art.1780371106. ISSN 0004-3591.
- ↑ Vaerøy, Henning; Helle, Robert; Førre, Øystein; Kåss, Erik; Terenius, Lars (January 1988). "Elevated CSF levels of substance P and high incidence of Raynaud phenomenon in patients with fibromyalgia: new features for diagnosis". Pain. 32 (1): 21–26. doi:10.1016/0304-3959(88)90019-x. ISSN 0304-3959.
- ↑ Evengard, B.; Nilsson, C.G.; Lindh, G.; Lindquist, L.; Eneroth, P.; Fredrikson, S.; Terenius, L.; Henriksson, K.G. (November 1998). "Chronic fatigue syndrome differs from fibromyalgia. No evidence for elevated substance P levels in cerebrospinal fluid of patients with chronic fatigue syndrome". Pain. 78 (2): 153–155. ISSN 0304-3959. PMID 9839828.
- ↑ Nijs, Jo; Meeus, Mira; Van Oosterwijck, Jessica; Roussel, Nathalie; De Kooning, Margot; Ickmans, Kelly; Matic, Milica (January 22, 2011). "Treatment of central sensitization in patients with 'unexplained' chronic pain: what options do we have?". Expert Opinion on Pharmacotherapy. 12 (7): 1087–1098. doi:10.1517/14656566.2011.547475. ISSN 1465-6566.
- ↑ 54.0 54.1 Nijs, Jo; Malfliet, Anneleen; Ickmans, Kelly; Baert, Isabel; Meeus, Mira (June 15, 2014). "Treatment of central sensitization in patients with 'unexplained' chronic pain: an update". Expert Opinion on Pharmacotherapy. 15 (12): 1671–1683. doi:10.1517/14656566.2014.925446. ISSN 1465-6566.
- ↑ Meeus, Mira; Ickmans, Kelly; De Clerck, Luc S.; Moorkens, Greta; Hans, Guy; Grosemans, Sofie; Nijs, Jo (November 2011). "Serotonergic descending inhibition in chronic pain: design, preliminary results and early cessation of a randomized controlled trial". In Vivo (Athens, Greece). 25 (6): 1019–1025. ISSN 1791-7549. PMID 22021700.
- ↑ van den Broeke, Emanuel N.; Torta, Diana M.; Van den Bergh, Omer (July 2, 2018). "Central Sensitization: Explanation or Phenomenon?". Clinical Psychological Science: 216770261878180. doi:10.1177/2167702618781804. ISSN 2167-7026.
- ↑ Phillips, Kristine; Clauw, Daniel J. (January 28, 2013). "Review: Central pain mechanisms in the rheumatic diseases: Future directions". Arthritis & Rheumatism. 65 (2): 291–302. doi:10.1002/art.37739. ISSN 0004-3591.
- ↑ Toda, Katsuhiro (November 2014). "Central sensitization pain should be included in (central) neuropathic pain". Pain Physician. 17 (6): E783. ISSN 2150-1149. PMID 25415794.
- ↑ 59.0 59.1 Cervero, Fernando (2014). "Central sensitization and visceral hypersensitivity: Facts and fictions". Scandinavian Journal of Pain. 5 (2): 49–50. doi:10.1016/j.sjpain.2014.02.005. ISSN 1877-8860.
- ↑ Brosschot, Jos F. (April 2002). "Cognitive-emotional sensitization and somatic health complaints". Scandinavian Journal of Psychology. 43 (2): 113–121. doi:10.1111/1467-9450.00276. ISSN 0036-5564.
- ↑ Eriksen, H.R; Ursin, H (April 2004). "Subjective health complaints, sensitization, and sustained cognitive activation (stress)". Journal of Psychosomatic Research. 56 (4): 445–448. doi:10.1016/s0022-3999(03)00629-9. ISSN 0022-3999.