- This page was created by volunteers like you!
- Help us make it even better. To learn more about contributing to MEpedia, click here.
- Join the movement
- Visit #MEAction to find support or take action. Donate today to help us improve and expand this project.
Raynaud's syndrome
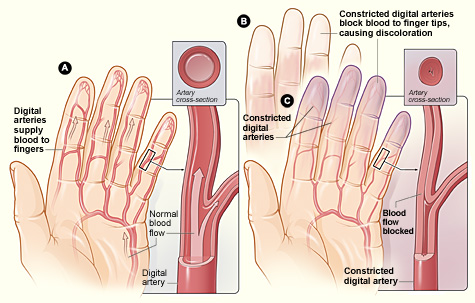
Raynaud's Syndrome or Raynaud's Phenomenon is a disorder that affects the blood vessels that carry blood from your heart to different parts of your body.[1][2] It is classified aa a nervous system disease,[3] and can be a comorbid illness presenting with several other chronic illnesses, including systemic sclerosis, chronic fatigue syndrome, fibromyalgia, lupus, some vascular diseases, and autoimmune diseases such as rheumatoid arthritis or Sjögren's syndrome.[2][4]
Types
- Primary Raynaud's (PRP) or Raynaud's disease is more common and less severe.
- Secondary Raynaud's (SRP) or Raynaud's phenomenon is caused by an underlying disease, condition or other factor. [1]
Causes
The cause of primary Raynaud's is unknown. It is more common and tends to be less severe than secondary Raynaud's.
Secondary Raynaud's is caused by an underlying disease, condition, or other factor and is often called Raynaud's phenomenon.[1] Possible causes are:
- Diseases and conditions that directly damage the arteries or damage the nerves that control the arteries in the hands and feet
- Repetitive actions that damage the nerves that control the arteries in the hands and feet, including carpal tunnel syndrome or repetitive strain injury
- Injuries or surgeries to the hands or feet.
- Exposure to certain chemicals
- Medicines that narrow the arteries or affect blood pressure, eg. Certain medicines, those for migraines, cancer, high blood pressure, birth control, and some over the counter cold or allergy medications.[1]
Risk factors
The risk factors for primary (Raynaud's disease) and secondary (Raynaud's phenomenon) are different.[1]
Primary
- Female sex.
- Age. Primary Raynaud's usually develops before the age of 30.
- Family history of Primary Raynaud's.
- Living in a cold climate, which can trigger Raynaud's attacks.[1]
Secondary
- Age. Secondary Raynaud's usually develops after the age of 30.
- Certain diseases and conditions. For example, diseases that directly damage the arteries or damage the nerves that control the arteries in the hands and feet may cause secondary Raynaud's. Fibromyalgia is more common in people with Raynaud's syndrome.[4]
- Injuries or surgeries to the hands or feet.
- Exposure to certain workplace chemicals, such as vinyl chloride (used in the plastics industry).
- Repetitive actions with the hands, such as typing or using vibrating tools.
- Certain medicines, such as those for migraines, cancer, high blood pressure, cold, or allergy medications.
- Smoking.
- Living in a cold climate.[1]
Triggers and symptoms
Cold temperatures can bring on an attack. "During an attack, little or no blood flows to affected body parts. As a result, the skin may turn white and then blue for a short time. As blood flow returns, the affected areas may turn red and throb, tingle, burn, or feel numb."[1]
Tests and diagnosis
"To distinguish between primary and secondary Raynaud's, your doctor may perform an in-office test called nail fold capillaroscopy. During the test, the doctor examines your nail fold — the skin at the base of your fingernail — under a microscope. Tiny blood vessels (capillaries) near the nail fold that are enlarged or deformed may indicate an underlying disease. However, some secondary diseases can't be detected by this test."[5]
To determine if an immune system disease is the underlying cause for Raynaud's there are blood tests, including the Antinuclear antibodies test (ANA) and Erythrocyte sedimentation rate (ESR).[5] There is no single test for Raynaud's syndrome itself.[5]
See also
Learn more
- Reynauld's disease - Symptoms and causes - Mayo Clinic
- Frequently Asked Questions[6] - The Raynaud's Association
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 "Raynaud's | Health Topics". Retrieved January 4, 2022.
- ↑ 2.0 2.1 https://www.rcpjournals.org/content/clinmedicine/20/6/580
- ↑ "ICD-10 Version:2016". World Health Organization. 2016. Retrieved May 7, 2019.
- ↑ 4.0 4.1 Pauling, John D.; Hughes, Michael; Pope, Janet E. (December 1, 2019). "Raynaud's phenomenon—an update on diagnosis, classification and management". Clinical Rheumatology. 38 (12): 3317–3330. doi:10.1007/s10067-019-04745-5. ISSN 1434-9949.
- ↑ 5.0 5.1 5.2 "Raynaud's disease - Diagnosis and treatment". Mayo Clinic. Retrieved October 11, 2018.
- ↑ "Frequently Asked Questions". The Raynaud's Association. Retrieved October 11, 2018.

