- This page was created by volunteers like you!
- Help us make it even better. To learn more about contributing to MEpedia, click here.
- Join the movement
- Visit #MEAction to find support or take action. Donate today to help us improve and expand this project.
Pituitary gland
The pituitary gland, or hypophysis, is a pea-sized gland of the endocrine system, situated at the base of the brain. As part of the HPA axis, it is regulated by the hypothalamus to produce, store, and secrete various hormones, which target other endocrine glands. The pituitary gland is sometimes referred to as the “master gland” as it regulates the function of the other endocrine glands.[1]
Structure and Function
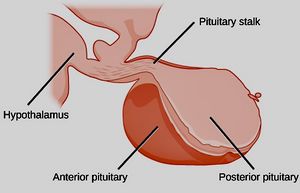
Image: Modified from Gray’s Anatomy by OpenStax (2018) with minor cropping and color changes/filters by MEpedia. License: CC-BY-4.0.[2]
The pituitary gland sits at the base of the brain, underneath the hypothalamus. It is surrounded by a protective bony cavity called the sella turcica. The pituitary is divided into three distinct lobes: posterior, anterior, and intermediate.[1]
Posterior
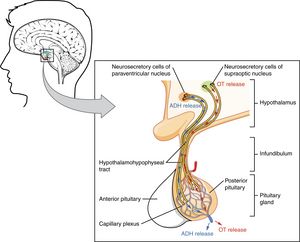
Image: The Pituitary Gland and Hypothalamus. Fig. 17.8 Posterior Pituitary. License: CC-BY-4.0.[3]
The posterior pituitary develops as an extension of the hypothalamus (distinct from the anterior pituitary). The posterior pituitary is largely made up of the terminals of nerve cells of the hypothalamus, as neurons in the hypothalamus project directly to the posterior pituitary. Hormones produced by the hypothalamus are stored in the terminals of hypothalamic neurons in the posterior pituitary, and are released by nerve excitation. The two major hormones stored and secreted by the posterior pituitary include:
- Antidiuretic hormone (ADH, also known as vasopressin)
- Oxytocin[4]
Anterior
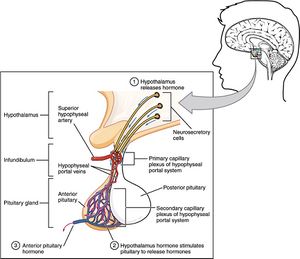
Image: The Pituitary Gland and Hypothalamus. Fig. 17.9 Anterior Pituitary. License: CC-BY-4.0.[3]
The anterior pituitary is structurally distinct from the posterior pituitary. It makes up 80% of the pituitary gland, and is made up of different types of endocrine cells. These cells are classified by the hormones they synthesize and release, and are regulated by the hypothalamus via releasing and inhibiting hormones. The six major hormones of the anterior pituitary are:
- Growth hormone (GH)
- Adrenocorticotropic hormone (ACTH)
- Thyroid-stimulating hormone (TSH)
- Follicular-stimulating hormone (FSH)
- Luteinizing hormone (LH)
- Prolactin[4][1]
Intermediate
The intermediate lobe is present in many lower vertebrates, but is almost absent in humans. The intermediate pituitary synthesizes and secretes:
Function of Pituitary Hormones
| Hormone | Target Organ | Role |
| Growth hormone (GH) | Muscular, skeletal, and fat tissue | Regulates growth and physical development by stimulating muscle growth and reducing fat tissue |
| Adrenocorticotropic hormone (ACTH) | Adrenal glands | Stimulates the adrenal glands to produce cortisol and other hormones |
| Thyroid-stimulating hormone (TSH) | Thyroid gland | Stimulates the thyroid to produce thyroid hormone |
| Follicular-stimulating hormone (FSH) | Ovaries or testes | Stimulates the ovaries to produce eggs/the testes to produce sperm, and the sex organs to produce sex hormones |
| Luteinizing hormone (LH) | Ovaries or testes | Stimulates the ovaries to produce eggs/the testes to produce sperm, and the sex organs to produce sex hormones |
| Prolactin | Mammary glands | Stimulates the mammary glands to produce milk |
| Antidiuretic hormone (ADH, also known as vasopressin) | Kidneys | Regulates amount of water absorbed and excreted by the kidneys |
| Oxytocin | Uterus and mammary glands | Causes uterus contraction during childbirth, stimulates contractions of the milk ducts in breast for breastfeeding |
| Melanocyte-stimulating hormone (MSH) | Skin and hair | Stimulates the production of melanin in skin and hair, suppresses appetite, contributes to sexual arousal.[1] |
Dysfunction and Disease
Dysfunction of the pituitary gland can result in overproduction or underproduction of pituitary hormones, thus having major consequences in bodily function. Conditions of pituitary malfunction include:
- Acromegaly -- overproduction of GH
- Cushing's disease -- overproduction of ACTH
- GH deficiency -- underproduction of GH
- Syndrome of inappropriate antidiuretic hormone -- overproduction of antidiuretic hormone
- Diabetes insipidus -- underproduction of antidiuretic hormone
- Sheehan syndrome -- underproduction of any pituitary hormone
- Pickardt-Falhbusch Syndrome -- underproduction of any pituitary hormone aside from prolactin
- Hyperpituitarism (usually pituitary adenoma) -- overproduction of any pituitary hormone
- Hypopituitarism -- underproduction of any pituitary hormone
- Hypophysitis -- inflammation of the pituitary gland
- Autoimmune hypophysitis -- inflammation of the pituitary gland due to autoimmunity
- Pituitary adenoma -- noncancerous tumor of the pituitary gland[citation needed]
ME/CFS
Dysfunction of the endocrine system, with a focus on hypothalamic-pituitary-adrenal axis (HPA axis) hypofunction, has been reported in individuals with ME/CFS.[5][6][7][8]. It has been suggested that HPA axis hypofunction in ME/CFS is caused by chronic activation of the inflammatory and oxidative and nitrosative stress pathways[8]. However, this area of research continues to lack studies with direct measures of pituitary function.
Some patients report that there seems to be a period of pituitary/HPA axis hyperfunction in the earlier stage of ME/CFS, whereas later in disease progression there's a switch to hypofunction. This could perhaps explain some of the wide variation across studies (e.g.,[9][10][11]).
Patients with ME have also reported other problems with the pituitary, such as empty sella syndrome and pituitary adenoma. These may be of note to guide future research.[citation needed]
See also
Learn more
- Endocrine Glands - OpenStax Biology 2e
- The Pituitary Gland and Hypothalamus - OpenStax Anatomy and Physiology
- The hypothalamus and pituitary gland - Khan academy
References
- ↑ 1.0 1.1 1.2 1.3 "Overview of the Pituitary Gland - Hormonal and Metabolic Disorders". Merck Manuals Consumer Version. Retrieved October 25, 2018.
- ↑ Clark MA, Douglas M, Choi J (March 28, 2018). "37.5 Endocrine Glands". Biology 2e. Houston, Texas: OpenStax.
- ↑ 3.0 3.1 Betts, JG; Young, KA; Wise, JA; Johnson, E; Poe, B; Kruse, DH; Korol, O; Johnson, JE; Womble, M; DeSaix, P (April 25, 2013). "17.3 The Pituitary Gland and Hypothalamus". Anatomy and Physiology. OpenStax. Houston, Texas. Retrieved November 9, 2021.
- ↑ 4.0 4.1 Nussey, Stephen; Whitehead, Saffron (2001). The pituitary gland. BIOS Scientific Publishers.
- ↑ Nijhof, Sanne L.; Rutten, Juliette M. T.M.; Uiterwaal, Cuno S. P.M.; Bleijenberg, Gijs; Kimpen, Jan L.L.; Putte, Elise M. van de (April 2014). "The role of hypocortisolism in chronic fatigue syndrome". Psychoneuroendocrinology. 42: 199–206. doi:10.1016/j.psyneuen.2014.01.017. ISSN 1873-3360. PMID 24636516.
- ↑ Papadopoulos, Andrew S.; Cleare, Anthony J. (September 27, 2011). "Hypothalamic-pituitary-adrenal axis dysfunction in chronic fatigue syndrome". Nature Reviews. Endocrinology. 8 (1): 22–32. doi:10.1038/nrendo.2011.153. ISSN 1759-5037. PMID 21946893.
- ↑ Heim, Christine; Nater, Urs M.; Maloney, Elizabeth; Boneva, Roumiana; Jones, James F.; Reeves, William C. (January 2009). "Childhood trauma and risk for chronic fatigue syndrome: association with neuroendocrine dysfunction". Archives of General Psychiatry. 66 (1): 72–80. doi:10.1001/archgenpsychiatry.2008.508. ISSN 1538-3636. PMID 19124690.
- ↑ 8.0 8.1 Morris, Gerwyn; Anderson, George; Maes, Michael (October 20, 2016). "Hypothalamic-Pituitary-Adrenal Hypofunction in Myalgic Encephalomyelitis (ME)/Chronic Fatigue Syndrome (CFS) as a Consequence of Activated Immune-Inflammatory and Oxidative and Nitrosative Pathways". Molecular Neurobiology. 54 (9): 6806–6819. doi:10.1007/s12035-016-0170-2. ISSN 0893-7648.
- ↑ DEMITRACK, MARK A.; DALE, JANET K.; STRAUS, STEPHEN E.; LAUE, LOUISA; LISTWAK, SAM J.; KRUESI, MARKUS J.P.; CHROUSOS, GEORGE P.; GOLD, PHILIP W. (December 1991). "Evidence for Impaired Activation of the Hypothalamic-Pituitary-Adrenal Axis in Patients with Chronic Fatigue Syndrome". The Journal of Clinical Endocrinology & Metabolism. 73 (6): 1224–1234. doi:10.1210/jcem-73-6-1224. ISSN 0021-972X.
- ↑ Di Giorgio, Annabella; Hudson, Marina; Jerjes, Walid; Cleare, Anthony J. (May 2005). "24-hour pituitary and adrenal hormone profiles in chronic fatigue syndrome". Psychosomatic Medicine. 67 (3): 433–440. doi:10.1097/01.psy.0000161206.55324.8a. ISSN 1534-7796. PMID 15911907.
- ↑ "Basal circadian and pulsatile ACTH and cortisol secretion in patients with fibromyalgia and/or chronic fatigue syndrome". Brain, Behavior, and Immunity. 18 (4): 314–325. July 1, 2004. doi:10.1016/j.bbi.2003.12.011. ISSN 0889-1591.

