Poliovirus
Poliovirus is an enterovirus. It is the cause of the paralytic disease known as poliomyelitis."[1]
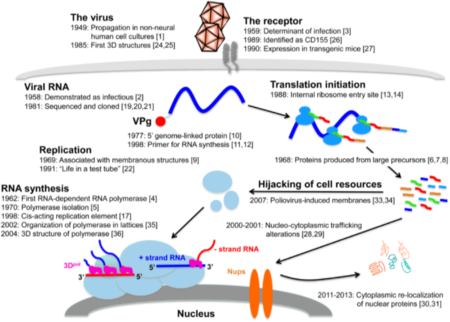
Source: Lévêque N, Semler BL (2015) A 21st Century Perspective of Poliovirus Replication. PLoS Pathog 11(6): e1004825. doi:10.1371/journal.ppat.1004825
© 2015 Lévêque, Semler CC-BY 4.0.
Metabolic effects[edit | edit source]
A study of poliovirus found that polio infection rapidly decreases (45% decrease) cellular oxygen consumption (and thus energy production through cellular respiration) by inhibiting succinate dehydrogenase (55% decrease in activity) and blocking mitochondrial electron transport at or between complexes I and III.[2]
Relationship to myalgic encephalomyelitis[edit | edit source]
Prior to the poliovirus vaccine, several outbreaks of what later came to be called myalgic encephalomyelitis coincided with confirmed outbreaks of poliomyelitis including the 1934 Los Angeles outbreak, the 1948 Akureyri, Iceland outbreak, and 1949 outbreak in Adelaide, Australia. Many outbreaks were initially misinterpreted as clusters of poliomyelitis or abortive poliomyelitis, hence one of ME's earliest names, atypical polio. It is not known whether there is a direct relationship between polio outbreaks and ME or if outbreaks of ME were more likely to be reported when public health authorities were already mobilized for an earlier crisis.
No serological evidence of polio was ever found in these outbreaks and the ultimate pattern of the outbreaks differed in significant ways, chief among them, the tendency to affect adults rather than children, and to result in higher morbidity than poliomyelitis but no mortality.[3] Findings in several outbreaks seemed to suggest that symptoms were caused by an enterovirus distinct from but related to polio including findings of mild, diffuse peripheral nervous system damage in monkeys infected with the virus; a stronger response to polio vaccination in children who had been in epidemic areas; and seasonal patterns of infection resembling polio.[3]
Cross-immunity[edit | edit source]
It is theorized that exposure to one enterovirus may confer partial immunity or improved immune response to another enteroviruses. One study compared schoolchildren in Estonia, who were inoculated with the Sabin, live attenuated virus polio vaccine, to Finnish schoolchildren, who were inoculated with the Salk, inactivated vaccine.[4] Estonian children had stronger T cell responses to coxsackievirus B4 and poliovirus type 1, and stronger expression of IFN-γ when exposed to poliovirus challenge as compared to Finnish children. Finnish children have weaker cellular immunity against enteroviruses at the age of 9 months compared with Estonian children at the same age. (Finland has a rate of type 1 diabetes three times the rate of Estonia. Coxsackie B4 has been associated with Type 1 diabetes.) An unintended consequence of widespread polio vaccination may have been impaired immunity to other enteroviruses, such as Coxsackie and echoviruses.
There is indirect evidence of cross-immunity between poliovirus and the unidentified virus or viruses in epidemic myalgic encephalomyelitis outbreaks. After the 1948-1949 Akureyri outbreak in Iceland, children in areas that had been affected responded to poliomyelitis vaccination with higher antibody titres, as if these children had already been exposed to an agent immunologically similar to poliomyelitis virus.[3][5] During the 1949-1953 outbreak in Adelaide, cases of classic poliomyelitis dropped by 43%.[6]
Post-polio syndrome[edit | edit source]
See also[edit | edit source]
References[edit | edit source]
- ↑ Poliovirus - Virology Blog
- ↑ Koundouris, A (May 2000). "Poliovirus Induces an Early Impairment of Mitochondrial Function by Inhibiting Succinate Dehydrogenase Activity". Biochemical and Biophysical Research Communications. 271: 610–4.
- ↑ 3.0 3.1 3.2 Parish, JG (1978). "Early outbreaks of 'epidemic neuromyasthenia'". Postgraduate Medical Journal. 54: 711–7.
- ↑ Juhela, S (July 1999). "Comparison of enterovirus-specific cellular immunity in two populations of young children vaccinated with inactivated or live poliovirus vaccines". Clinical & Experimental Immunology. 117: 100–105.
- ↑ Sigurdsson, B (February 15, 1958). "Response to poliomyelitis vaccination". The Lancet. 1: 370–1.
- ↑ "Poliomyelitis in 1953" Bulletin of the World Health Organization. 1955;12(4):595-649.

