Immunoglobulin G
Immunoglobulin G or IgG or immune gamma globulin is a the most common class of antibody in human blood, making up 80% of the antibodies, and is also found in tissue spaces.[1] IgG antibodies bind to phagocytes, have γ (gamma) heavy chains and can cross the placenta.[1] The IgG class consists of IgG1, IgG2, IgG3 and IgG4.[2]
Function[edit | edit source]
IgG is the only antibody that can cross the placenta, giving unborn and new born babies protection against contagious diseases and other infections.[1]
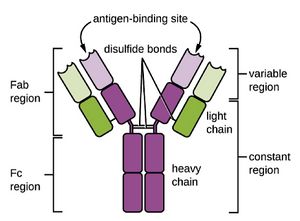
Source: Parker, Nina; Schneegurt, Mark; Tu, Anh-Hue Thi; Lister, Philip; Forster, Brian M. (November 1, 2016). "18.1 Overview of Specific Adaptive Immunity". Microbiology. OpenStax. Houston, Texas.
IgG1[edit | edit source]
The most common IgG antibody.[2]
IgG2[edit | edit source]
The most common IgG antibody.[2]
IgG3[edit | edit source]
IgG3 or immunoglobulin G3 level along with other factors was found to be predictive of the likelihood of developing Long COVID after SARS-CoV-2 infection by Cervia et al. (2022).[3] IgG3 deficiencies have been found in some ME/CFS patients.[4]
IgG4[edit | edit source]
IgG4 deficiencies have been found in some ME/CFS patients, but IgG4 subclass deficiency without other IgG deficiencies is not considered a primary immunodeficiency.[2][4]
ME/CFS[edit | edit source]
IgG3 and IgG4 deficiencies were found in a significant number of ME/CFS patients by Lutz et al. (2021), who reported that these were the most common unclassified antibody deficiencies in the 17.6% of ME/CFS patients with unclassified antibody deficiencies.[4]
IVIG or intravenous immunoglobulin or gamma globulin therapy, an immunoglobulin treatment that typically includes IgG, has been investigated for ME/CFS, with positive results shown for some patients.[5]
Fibromyalgia[edit | edit source]
In 2021, Goebel et al. published research showing that fibromyalgia may be an immune system disease mediated by IgG; in an animal study on mice they found that the mice developed pain and cold intolerance symptoms consistent with fibromyalgia after receiving IgG from the blood of patients with fibromyalgia.[6]
Long COVID[edit | edit source]
Cervia et al. (2022) found that both IgG3 and IgM, when combined with other factors including age, presence of five symptoms (fever, fatigue, cough, shortness of breath, gastrointestinal symptoms during COVID-19 infection), acted as biomarkers to predict who would develop Long COVID after SARS-CoV-2 infection.[3]
News and articles[edit | edit source]
"Andersson and his colleagues harvested blood from 44 people with fibromyalgia and injected purified antibodies from each of them into different mice. The mice rapidly became more sensitive to pressure and cold, and displayed reduced grip strength in their paws. Animals injected with antibodies from healthy people were unaffected."[7]
Prof Camilla Svensson from the Karolinska Institute in Sweden, who was also involved in the study, said:
"Antibodies from people with fibromyalgia living in two different countries, the UK and Sweden, gave similar results, which adds enormous strength to our findings."[7]
Notable studies[edit | edit source]
- 1998, IgG subclass deficiencies in chronic fatigue syndrome[8] - [ (Abstract)]
- 1990, A double-blind, placebo-controlled trial of intravenous immunoglobulin therapy in patients with chronic fatigue syndrome[5] - (Abstract)
- 2021, Passive transfer of fibromyalgia symptoms from patients to mice[6] - (Full text)
- 2021, Evaluation of Immune Dysregulation in an Austrian Patient Cohort Suffering from Myalgic Encephalomyelitis/Chronic Fatigue Syndrome[4] - (Full text)
- 2021, Clinical characteristics with inflammation profiling of Long-COVID and association with one-year recovery following hospitalisation in the UK: a prospective observational study[9] - (Full text)
- 2022, Immunoglobulin signature predicts risk of post-acute COVID-19 syndrome[3] - (Full text)
Learn more[edit | edit source]
- Overview of specific adaptive autoimmunity - OpenStax
- The Immune Response against Pathogens - OpenStax
See also[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Parker, Nina; Schneegurt, Mark; Tu, Anh-Hue Thi; Lister, Philip; Forster, Brian M. (November 1, 2016). "18.1 Overview of Specific Adaptive Immunity". Microbiology. OpenStax. Houston, Texas. Retrieved July 9, 2021.
- ↑ 2.0 2.1 2.2 2.3 "IgG Subclass Deficiency". Immune Deficiency Foundation. Retrieved January 26, 2022.
- ↑ 3.0 3.1 3.2 Cervia, Carlo; Zurbuchen, Yves; Taeschler, Patrick; Ballouz, Tala; Menges, Dominik; Hasler, Sara; Adamo, Sarah; Raeber, Miro E.; Bächli, Esther; Rudiger, Alain; Stüssi-Helbling, Melina (January 25, 2022). "Immunoglobulin signature predicts risk of post-acute COVID-19 syndrome". Nature Communications. 13 (1): 446. doi:10.1038/s41467-021-27797-1. ISSN 2041-1723.
- ↑ 4.0 4.1 4.2 4.3 Lutz, Lena; Rohrhofer, Johanna; Zehetmayer, Sonja; Stingl, Michael; Untersmayr, Eva (September 14, 2021). "Evaluation of Immune Dysregulation in an Austrian Patient Cohort Suffering from Myalgic Encephalomyelitis/Chronic Fatigue Syndrome". Biomolecules. 11 (9): 1359. doi:10.3390/biom11091359. ISSN 2218-273X. PMC 8465819. PMID 34572574.
- ↑ 5.0 5.1 Lloyd, A.; Hickie, I.; Wakefield, D.; Boughton, C.; Dwyer, J. (November 1990). "A double-blind, placebo-controlled trial of intravenous immunoglobulin therapy in patients with chronic fatigue syndrome". The American Journal of Medicine. 89 (5): 561–568. doi:10.1016/0002-9343(90)90173-b. ISSN 0002-9343. PMID 2146875.
- ↑ 6.0 6.1 Goebel, Andreas; Krock, Emerson; Gentry, Clive; Israel, Mathilde R.; Jurczak, Alexandra; Urbina, Carlos Morado; Sandor, Katalin; Vastani, Nisha; Maurer, Margot (July 7, 2021). "Passive transfer of fibromyalgia symptoms from patients to mice". The Journal of Clinical Investigation. 131 (13). doi:10.1172/JCI144201. ISSN 0021-9738.
- ↑ 7.0 7.1 "Fibromyalgia may be a condition of the immune system not the brain – study". the Guardian. July 1, 2021. Retrieved July 8, 2021.
- ↑ Cite error: Invalid
<ref>tag; no text was provided for refs named:1988 - ↑ Writing Group (on behalf of the PHOSP-COVID Collaboration Group); Evans, Rachael A.; Leavy, Olivia C.; Richardson, Matthew; Elneima, Omer; McAuley, Hamish J.C.; Shikotra, Aarti; Singapuri, Amisha; Sereno, Marco; Saunders, Ruth M.; Harris, Victoria Claire (December 20, 2021). "Clinical characteristics with inflammation profiling of Long-COVID and association with one-year recovery following hospitalisation in the UK: a prospective observational study". Medrxiv: 2021.12.13.21267471. doi:10.1101/2021.12.13.21267471.

