There are no approved pharmacological treatments for ME anywhere in the world, except in Argentina, which has approved the immunomodulator Ampligen for severe ME/CFS as of August 23, 2016.[13]
ME has occurred in both epidemic and sporadic form since at least the 1930s, although it has likely been occurring much longer but was not formally named. The first recorded outbreak of epidemic myalgic encephalomyelitis was in 1934 in Los Angeles and was thought to be an outbreak of atypical polio. After the outbreak in Akureyri, Iceland in 1946, the disease came to be called 'Akureyri Disease' or Icelandic disease through much of the 1940s and 1950s. It was named ME after London's Royal Free Hospital outbreak in 1955. Other names included benign myalgic encephalomyelitis and epidemic neuromyasthenia.
After the Incline Village outbreak in Nevada in 1984, the disease came to be called and redefined as chronic fatigue syndrome (CFS). The most recent putative outbreak was in Arizona in 1996.
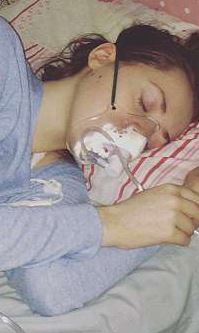
Merryn Crofts was
bedbound and unable to eat. Merryn weighed six stone (84 lbs) at her death; her autopsy revealed inflammation of the
ganglia. It is suspected that in the later years of her illness Merryn also suffered from
EDS and
MCAD. Her death certificate is the 2nd in the
UK to attribute a death to ME
The name ME[18] was coined by Dr. Melvin Ramsay following the 1955 Royal Free Hospital outbreak[19] and is a portmanteau of several of the key signs and symptoms of the disease: myalgic (muscle pain), encephalo (brain), myel (spinal cord), itis (inflammation).[20] The central nervous system (brain and spinal cord) are inflamed.[21]
Several other names have been used or proposed throughout the history of the disease, including atypical polio, Icelandic disease, benign ME, epidemic neuromyasthenia, CFS, and systemic exertion intolerance disease (SEID). This has lead to much confusion as a variety of names have been used at different times to describe discrete outbreaks as well as a larger and potentially more heterogenous population of sporadic cases, defined by a wide variety of case definitions.
A survey by The MEAction Network in 2016 found that the majority of patients prefer the name ME to other names including chronic fatigue syndrome.[22]
Myalgic encephalomyelitis (ME) was the original name for chronic fatigue syndrome (CFS); the names are used interchangeably or with the acronym ME/CFS.[21]
Following after an incubation period of 4 to 7 days, the prodromal phase generally involve a flu-like illness with low-grade fever. In the majority but not all cases, an infection or infectious process is evident.[23] Two to seven days later, a chronic phase commences, characterized by a measurable diffuse change in the function of the CNS. It is this second phase, persistent phase that most characterizes ME.[24][1]
In some patients, the initial presentation involved a severe, incapacitating prolonged illness. In theirs, an apparent remission was followed by relapses brought on by exertion, menstrual period, or cold. In other patients there is no discernible triggering event.
Symptoms can range from mild to very severe and can include:
Symptom presentation and severity can vary considerably day to day and even hour to hour.[1] Overexertion can exacerbate all symptoms, and Post Exertional Malaise often delayed by 24 hours or more.[25] [1] The US National Institutes of Health (NIH) notes that sensitivity to noise, light and chemicals may force patients to withdraw from society.[26]
The severity of a patient's symptoms often depends on the time period since the disease was contacted and rate of progression of each patient. The rate of progression can be accelerated by physical or cognitive activity beyond a patient's limits over long periods, which typically entails anaerobic activity [27]
A core symptom, post-exertional malaise, is intolerance to previously trivial effort such as walking to the mailbox, running an errand or grocery shopping, taking a shower or brushing teeth, and deterioration of health from persistent or repeated exertion.[5][6][7][8][9][10][28]

Alem Matthees is an
Australian ME patient that filed an FOI request for data from the
PACE trial. At a
great cost to his health, Alem appealed the denial of the data and won. This data proved the results published in
The Lancet were untrue. Alem's health suffered significantly in part from the efforts required for the FOI request and tribunal
Although there is no definitive
biomarker, several signs and findings have been frequently observed in clinical settings:
There are several proposed criteria for diagnosing ME including the
International Consensus Criteria (
ICC) and the
Canadian Consensus Criteria (
CCC). The original criteria developed by
Melvin Ramsay, the
Ramsay definition, is not used for diagnosing ME today.
Several, overly broad criteria have been proposed and are in use. These criteria likely capture some patients with the disease characterized in the medical literature on epidemic ME, exclude others, and also include patients with a wide range of other undiagnosed conditions including cancer, depression, and a range of autoimmune diseases. The United Kingdom's Oxford criteria is the broadest and likely least discerning definition. (The US Institute of Medicine report called for its complete retirement.)[29] The US Centers for Disease Control's (CDC) Fukuda criteria, in use since 1994, is also overly broad.
The signs and symptoms of ME can be similar to other medical problems, "such as cancer, multiple sclerosis, lupus, brucellosis, or another condition."[1] Additional testing may be needed to help distinguish ME from these other problems.
ME relapses are often a result of over-activity, but can occur without warning with no obvious inciting factors. Exposure to increased sensory information in light, sound, and movement can provoke a sensory storm.
Infections, such as the common cold, influenza and gastroenteritis, also increase the risk for a relapse. Heat and cold can transiently increase symptoms.
Pregnancy can directly affect the susceptibility for relapse. Later pregnancy appears to offer a natural protection against relapses, and there are anecdotal reports of postpartum remission. However, pregnancy does not seem to influence long-term disability.
About 25% of patients become severe or very severely ill with ME.
Kerr et al proposed 7 different subsets for 'CFS' as it is defined today:[30][31]

Whitney Dafoe is an American photographer who has a
very severe form of ME. Whitney can no longer speak or handle contact with anyone but his parents. His father is
Ron Davis, a world-renowned geneticist who is working to solve his son's disease
- Subtype 2 This is one of the more severe subtypes. Effects are musculoskeletal, pain and anxiety/depression.
- Subtype 3 This subtype has the mildest symptoms.
- Subtype 4 This subtype is dominated by cognitive issues.
- Subtype 5 Effects are musculoskeletal and gastrointestinal.
- Subtype 6 This subtype is dominated by post-exertional malaise (extreme crash after exercise or exertion.)
- Subtype 7 This is one of the more severe subtypes. Effects are pain, infections, musculoskeletal, sleep-related, neurological, gastrointestinal, neurocognitive and anxiety/depression.[30]
ME is a multi-system disease. Numerous biological abnormalities have been found in multiple bodily system, however no common, central cause or mechanism has yet been elucidated.

Sophia Mirza was a
very severely ill ME patient who lived in the UK. Sophia's death came not long after a forced entry into her mother's home and being sectioned and taken to a mental hospital in 2003. An independent Neuropathologist found Sophia's spine contained a massive infection. Her death certificate was the first in the UK to attribute a death to
CFS Radiological research on ME has shown
hypoperfusion of the
brain stem and an abnormal response to exertion, but research on
CFS is often inconsistent and must be interpreted with caution. For example, some research stated that a reduced volume of
grey matter may be a result of a lack of activity and is reversible with
cognitive behavioral therapy (
CBT).
According to a strictly immunological explanation of CFS, the inflammatory processes triggered by T cells create leaks in the blood-brain barrier (a capillary system that should prevent entrance of T-cells in the nervous system). These leaks, in turn, cause a number of other damaging effects such as swelling, activation of macrophages, and more activation of cytokines and other destructive proteins such as Rnase-L. Channelopathy, a reduced ability to move metabolites in and out of cells has been implicated in this process. This may also be applicable to ME.
Some evidence shows viral infection of muscle and brain in at least a proportion of sufferers. This triggers inflammatory processes, stimulating other immune cells and soluble factors like cytokines and antibodies. A model for late ME has been proposed analogously to post-polio syndrome in which repaired nerve tissue forms inappropriately [The Late Effects of ME: Can they be distinguished from the post-polio syndrome?].
Hemodynamic abnormalities are widely found, including serum and RBC hypovolemia, neurally mediated hypotension, (NMH) and cerebral hypoperfusion. Vascular and endothelial abnormalities have been published by MERUK. However, none of these studies used research criteria for ME so the results may not be applicable to ME.
Some cardiologic features such as cardiac insufficiency, inverted T-waves and myofiber disarray have been reported in CFS and recently added to by findings of reduced Q-value. This has led clinician and researcher Dr Paul Cheney to posit that CFS is form of partially compensated cardiomyopathy in which orthostatic intolerance and rapid fatiguability are secondary protective mechanisms. Due to the heterogeneity of the population, a single cause is unlikely, but one-third of people with ME have abnormalities when tested with Holter monitors.

Florence Nightingale was a British citizen and pioneer of modern nursing. Nightingale was stationed in Crimea when she developed "Crimean fever" (a bacterial infection now known as
brucellosis) and never recovered. She remained
mostly bedbound the rest of her life. Although ME and
CFS were not defined in her lifetime, many current physicians and medical historians believe she developed ME/
CFS as a result of a chronic brucellosis infection
A Norwegian CFS/ME study shows that the disease affects all ages, with two peak ages of 10-19 years and 30-39 years; it is more common in women than in men.[32] Research by the Open Medicine Foundation cited in its paper, Metabolic features of chronic fatigue syndrome which studied severe CFS, found that the disease is different in men and women but this is not related to testosterone or estrogen. Michael VanElzakker notes there are male and female differences in neuropathic pain. A study of UK and Dutch cohorts found "younger children had a more equal gender balance compared to adolescents and adults."[33]
Risk Factors and Potential Causes[edit | edit source]
Although risk factors for myalgic encephalomyelitis have been identified, no single definitive virus has been found in all cases, which has led to the claim that ME is a common end path of a variety of infectious insults.[34][35][36][37] It is still possible ME involves some combination of both environmental and genetic factors. Various theories try to combine the known data into plausible explanations.[38][39] Several theories suggest that ME is an inappropriate immune response to an infection, a theory bolstered by the observation that there is sometimes a family history of autoimmune disease.[40] There is also a shift from the Th1 type of helper T cells, which fight infection, to the Th2 type, which are more active in allergy and more likely to attack the body.[41][42]
Other theories describe ME as an immune response to a chronic infection. The association between ME and the Coxsackie B, HHV-6, and HHV-7 viruses[43][44] [45] suggests a potential viral contribution in at least some individuals. Evidence from epidemic myalgic encephalomyelitis strongly point to an enterovirus, however, in most outbreaks, no virus was successfully isolated.
Others believe ME may sometimes result from a chronic infection with spirochetal bacteria, such as lyme disease. Another bacterium that has been implicated in ME is chlamydia pneumoniae.[46][47] Protein findings relating to several infections have seen found in the oligoclonal bands ME of patients.[48]
The vagus nerve infection hypothesis (VNIH) accounts for why so many different infectious onsets could be responsible. The vagus nerve runs from the brain stem and throughout the body and has an impact on many body systems.
Given the uncertainty regarding the cause, ME and CFS patients are barred from donating blood or organs in the United Kingdom, United States and New Zealand while symptoms persist.[49][50][51]

Karina Hansen became
ill as an adult teenager and is
severely ill with ME. She was forcibly institutionalized for 3 1/2 years as the
Denmark healthcare system designates ME as
psychosomatic. Karina is now home with her family where she received cards from well-wishers from around the world. Karina's Danish High Court case and return home were featured in the documentary film
Unrest There is no cure for ME and no country has approved any pharmacological treatment for the disease except, Argentina which has approved Ampligen for the treatment of severe ME/CFS.[13] However the effectiveness of Ampligen is under dispute.[52] Other off label medications have been used with varying effectiveness in some patients.[53][54]
Treatments for sleep problems, headaches and pain are utilized by some doctors for some patients although these are treating symptoms and not ME itself.
Success of treating symptoms of ME is not well researched or documented.
An immune system modulator drug called Rituximab has failed in a phase III clinical trial.[55]
ME has been found world-wide, in at least 75 epidemics documented in published papers from the 1930s to the 1980s.[56] Epidemics often occur in enclosed communities such as schools and hospitals.
As observed in many autoimmune disorders, ME is more common in females than males; the mean sex ratio is approximately 2-3 females for every male.[57] In children the sex ratio is approximately equal.[58]
Clinicians have observed several predisposing conditions, co-morbidities, overlapping conditions,[59] and increased risks for secondary diseases in patients with ME. However, as no large-scale epidemiological studies, genetic studies, or family studies have been done, there is little that can be said definitively about the rate or underlying biological reasons for these potentially related conditions. Overlapping diagnostic criteria and the lack of a biomarker in many of these conditions add to the confusion and diagnostic uncertainty. Moreover, certain conditions such as postural orthostatic tachycardia syndrome (POTS) and idiopathic intracranial hypertension (IH/IIH) are symptoms that can occur in or be co-morbid with numerous conditions, including ME.
The following are some syndromes and diseases that have been associated with or misdiagnosed as ME:
Due to lack of
funding by governments around the world there has been little biological research into
ME/CFS. There are studies which do reveal
neurological involvement,
metabolic features, and other abnormalities.
Generally accepted criteria for diagnosing ME/CFS and ME[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 "Myalgic Encephalomyelitis - NORD (National Organization for Rare Disorders)". NORD (National Organization for Rare Disorders). Retrieved September 7, 2018.
- ↑ Petrison, Lisa (April 4, 2016). "Myalgic Encephalomyelitis (ME) and Chronic Fatigue Syndrome (CFS) Medical Abnormalities Research Citations" (PDF). paradigmchange.me.
- ↑ "History of chronic fatigue syndrome". Wikipedia. July 22, 2018.
- ↑ "Myalgic Encephalomyelitis - NORD (National Organization for Rare Disorders)". NORD (National Organization for Rare Disorders). Retrieved September 8, 2018.
- ↑ 5.0 5.1 "Pathways to Prevention (P2P) Advancing the Research on Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)". Office of Disease Prevention. Retrieved September 7, 2018.
- ↑ 6.0 6.1 Research Descriptions of M.E. - ME Action UK
- ↑ 7.0 7.1 Ramsey, Melvin (1986). "The Clinical Features of Myalgic Encephalomyelitis". www.cfids-me.org. Retrieved September 7, 2018.
- ↑ 8.0 8.1 Dellwo, Adrienne (August 1, 2018). "What is Post-Exertional Malaise? Learn About a Key ME/CFS Symptom". Verywell Health. Retrieved September 7, 2018.
- ↑ 9.0 9.1 "Think You Might Have Chronic Fatigue Syndrome? Here are The Symptoms". WebMD. Retrieved September 7, 2018.
- ↑ 10.0 10.1 Spotila, Jennifer (2010). "Post-Exertional Malaise in Chronic Fatigue Syndrome" (PDF). solvecfs.org. The CFIDS Association of America.
- ↑ "Postexertion 'Crash,' not Fatigue per se, Marks Syndrome" (Login Needed). medscape.com.
- ↑ Howes, S (July 7, 2015). "Progressive Myalgic Encephalomyelitis (ME) or A New Disease? A Case Report" (PDF). meassocation.org. Physical Medicine and Rehabilitation - International – via Austin Publishers Group.
- ↑ 13.0 13.1 Inc., Hemispherx Biopharma, (August 23, 2016). "Hemispherx Biopharma Announces Major Breakthrough: Approval for Commercial Sale of Rintatolimod (U.S. Tradename: Ampligen®) to Treat Severe Cases of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS) in the Argentine Republic". GlobeNewswire News Room. Retrieved August 12, 2018. CS1 maint: extra punctuation (link)
- ↑ "myalgic". TheFreeDictionary.com. Retrieved August 12, 2018.
- ↑ "encephalo-". TheFreeDictionary.com. Retrieved August 12, 2018.
- ↑ "myel-". TheFreeDictionary.com. Retrieved August 12, 2018.
- ↑ "Itis". TheFreeDictionary.com. Retrieved August 12, 2018.
- ↑ Dellwo, Adrienne (July 23, 2018). "Myalgic Encephalomyelitis: Chronic Fatigue Syndrome's Other Name". Verywell Health. Retrieved August 12, 2018.
- ↑ "An Outbreak of Encephalomyelitis in the Royal Free Hospital Group, London, in 1955". British Medical Journal. 2 (5050): 895–904. October 19, 1957. ISSN 0007-1447. PMID 13472002.
- ↑ The Terminology of ME & CFS By Professor Malcolm Hooper
- ↑ 21.0 21.1 Dellwo, Adrienne (November 24, 2018). "Myalgic Encephalomyelitis or Chronic Fatigue Syndrome". Verywell Health. Retrieved November 28, 2018.
- ↑ "#MEAction RFI Poll Report (Part 1 of 3) - #MEAction". #MEAction. August 7, 2016. Retrieved September 8, 2018.
- ↑ ME Definition - Nightingale - PDF pg. 6
- ↑ "Nightingale ME Definition En | Chronic Fatigue Syndrome | Infection". Scribd. p. 5. Retrieved September 8, 2018.
- ↑ Research, Invest in ME. "Invest in ME Research - Invest in ME Research Home Page". www.investinme.org. Retrieved September 8, 2018.
- ↑ "Pathways to Prevention (P2P) Advancing the Research on Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)". Office of Disease Prevention. Retrieved September 8, 2018.
- ↑ "Unrest - MEpedia". www.me-pedia.org. Retrieved August 12, 2018.
- ↑ "What is Post-Exertional Malaise? Learn About a Key ME/CFS Symptom". Verywell Health. Retrieved September 7, 2018.
- ↑ Swift, Penny. "US NIH Report Calls for UK Definition of ME/CFS to be Scrapped". theargusreport.com. Retrieved September 8, 2018.
- ↑ 30.0 30.1 Kerr, JR; Burke, R; Petty, R; Gough, J; Fear, D; Mattey, D L; Axford, J S; Dalgleish, A G; Nutt, D J (May 30, 2008). "Seven genomic subtypes of chronic fatigue phenotypes analysis of gene networks and clinical syndrome/myalgic encephalomyelitis: a detailed" (PDF). me-ireland.com. JCP Online. doi:10.1136/jcp.2007.053553.
- ↑ Kerr, J. R.; Burke, B.; Petty, R.; Gough, J.; Fear, D.; Mattey, D. L.; Axford, J. S.; Dalgleish, A. G.; Nutt, D. J. (June 1, 2008). "Seven genomic subtypes of chronic fatigue syndrome/myalgic encephalomyelitis: a detailed analysis of gene networks and clinical phenotypes". Journal of Clinical Pathology. 61 (6): 730–739. doi:10.1136/jcp.2007.053553. ISSN 0021-9746. PMID 18057078.
- ↑ Bakken, Inger Johanne; Tveito, Kari; Gunnes, Nina; Ghaderi, Sara; Stoltenberg, Camilla; Trogstad, Lill; H åberg, Siri Eldevik; Magnus, Per (October 1, 2014). "Two age peaks in the incidence of chronic fatigue syndrome/myalgic encephalomyelitis: a population-based registry study from Norway 2008-2012". BMC Medicine. 12 (1). doi:10.1186/s12916-014-0167-5. ISSN 1741-7015. PMID 25274261.
- ↑ Collin, Simon M.; Nuevo, Roberto; van de Putte, Elise M.; Nijhof, Sanne L.; Crawley, Esther (October 28, 2015). "Chronic fatigue syndrome (CFS) or myalgic encephalomyelitis (ME) is different in children compared to in adults: a study of UK and Dutch clinical cohorts". BMJ open. 5 (10): e008830. doi:10.1136/bmjopen-2015-008830. ISSN 2044-6055. PMID 26510728.
- ↑ Evans, Meredyth (August 23, 2015). "Onset Patterns of Chronic Fatigue Syndrome and Myalgic Encephalomyelitis: A Mixed Method Approach". via.library.depaul.edu.
- ↑ "Vagus nerve infection hypothesis - MEpedia". me-pedia.org. Retrieved September 8, 2018.
- ↑ "Case Presentation - Chronic Fatigue Syndrome". www.clevelandclinicmeded.com. Retrieved September 8, 2018.
- ↑ Magnus, Per; Gunnes, Nina; Tveito, Kari; Bakken, Inger Johanne; Ghaderi, Sara; Stoltenberg, Camilla; Hornig, Mady; Lipkin, W. Ian; Trogstad, Lill (November 17, 2015). "Chronic fatigue syndrome/myalgic encephalomyelitis (CFS/ME) is associated with pandemic influenza infection, but not with an adjuvanted pandemic influenza vaccine". Vaccine. 33 (46): 6173–6177. doi:10.1016/j.vaccine.2015.10.018. ISSN 1873-2518. PMID 26475444.
- ↑ Underhill, R. A. (2015). "Myalgic encephalomyelitis, chronic fatigue syndrome: An infectious disease". Medical Hypotheses. 85 (6): 765–773. doi:10.1016/j.mehy.2015.10.011. ISSN 1532-2777. PMID 26604026.
- ↑ Schlauch, K A; Khaiboullina, S F; De Meirleir, K L; Rawat, S; Petereit, J; Rizvanov, A A; Blatt, N; Mijatovic, T; Kulick, D (2016). "Genome-wide association analysis identifies genetic variations in subjects with myalgic encephalomyelitis/chronic fatigue syndrome". Translational Psychiatry. 6 (2): e730–e730. doi:10.1038/tp.2015.208. ISSN 2158-3188.
- ↑ "Klimas ME CFS Genes Study". www.facebook.com. November 23, 2015. Retrieved September 8, 2018.
- ↑ "Cytokine expression provides clues to the pathophysiology of Gulf War illness and myalgic encephalomyelitis". Cytokine. 72 (1): 1–8. March 1, 2015. doi:10.1016/j.cyto.2014.11.019. ISSN 1043-4666.
- ↑ Hardcastle, S.L.; Brenu, E.W.; Staines, D.R.; Marshall-Gradisni, S. (2014). "Chronic Fatigue Syndrome/Myalgic Encephalomyelitis and the Potential Role of T Cells" (PDF). m-hikari.com.
- ↑ Bell, E. J.; McCartney, R. A.; Riding, M. H. (1988). "Coxsackie B viruses and myalgic encephalomyelitis". Journal of the Royal Society of Medicine. 81 (6): 329–331. doi:10.1177/014107688808100609. ISSN 0141-0768. PMID 2841461.
- ↑ "Ramsay Research Team 5 – The Potential Role of HHV-6 in ME/CFS - Solve ME/CFS Initiative". Solve ME/CFS Initiative. VOLKMEDIA. December 16, 2016. Retrieved September 8, 2018.
- ↑ Chapenko, Svetlana; Krumina, Angelika; Logina, Inara; Rasa, Santa; Chistjakovs, Maksims; Sultanova, Alina; Viksna, Ludmila; Murovska, Modra (2012). "Association of active human herpesvirus-6, -7 and parvovirus b19 infection with clinical outcomes in patients with myalgic encephalomyelitis/chronic fatigue syndrome". Advances in Virology. 2012: 205085. doi:10.1155/2012/205085. ISSN 1687-8647. PMID 22927850.
- ↑ . John E.Tovey. "Chlamydia pneumoniae infection a treatable cause of Chronic Fatigue Syndrome". The BMJ. September 5, 2018.CS1 maint: others (link)
- ↑ "New ME/CFS Study at Stanford: Dr. Montoya to test for scores of Infections - Prohealth". Prohealth. June 4, 2010. Retrieved September 8, 2018.
- ↑ "Role of Chronic Bacterial and Viral Infections in Neurodegenerative, Neurobehavioral, Psychiatric, Autoimmune and Fatiguing Illnesses: Part 1 | British Journal of Medical Practitioners". www.bjmp.org. 2009. Retrieved September 8, 2018.
- ↑ "People with ME/CFS to be permanently excluded from giving blood in the UK from 1 November this year – Department of Health announcement". www.meassociation.org.uk. August 2010. Retrieved September 8, 2018.
- ↑ Stein, Rob (December 3, 2010). "Chronic fatigue patients barred from blood donation". ISSN 0190-8286. Retrieved September 8, 2018.
- ↑ "Detailed eligibility criteria". www.nzblood.co.nz. Retrieved September 8, 2018.
- ↑ George, John (December 2, 2009). "FDA rejects Hemispherx's chronic fatigue drug Ampligen". www.bizjournals.com. Retrieved August 12, 2018.
- ↑ "Valganciclovir - MEpedia". www.me-pedia.org. Retrieved August 12, 2018.
- ↑ "Oxymatrine - MEpedia". www.me-pedia.org. Retrieved August 12, 2018.
- ↑ Johnson, Cort (November 26, 2017). "Norwegian Rituximab Chronic Fatigue Syndrome (ME/CFS) Trial Fails - Simmaron Research". Simmaron Research. Retrieved September 7, 2018.
- ↑ Bassett, Jodi (September 2010). "M.E.: The medical facts". The Hummingbirds' Foundation for M.E. Retrieved September 8, 2018.
- ↑ Bakken, Inger Johanne; Tveito, Kari; Gunnes, Nina; Ghaderi, Sara; Stoltenberg, Camilla; Trogstad, Lill; H åberg, Siri Eldevik; Magnus, Per (October 1, 2014). "Two age peaks in the incidence of chronic fatigue syndrome/myalgic encephalomyelitis: a population-based registry study from Norway 2008-2012". BMC Medicine. 12 (1). doi:10.1186/s12916-014-0167-5. ISSN 1741-7015. PMID 25274261.
- ↑ Collin, Simon M.; Nuevo, Roberto; van de Putte, Elise M.; Nijhof, Sanne L.; Crawley, Esther (October 28, 2015). "Chronic fatigue syndrome (CFS) or myalgic encephalomyelitis (ME) is different in children compared to in adults: a study of UK and Dutch clinical cohorts". BMJ open. 5 (10): e008830. doi:10.1136/bmjopen-2015-008830. ISSN 2044-6055. PMID 26510728.
- ↑ "Overlapping Conditions – American ME and CFS Society". ammes.org. Retrieved August 12, 2018.
- ↑ Carruthers, Bruce M.; Jain, Anil Kumar; De Meirleir, Kenny L.; Peterson, Daniel L.; Klimas, Nancy G.; Lerner, A. Martin; Bested, Alison C.; Flor-Henry, Pierre; Joshi, Pradip; Powles, A C Peter; Sherkey, Jeffrey A.; van de Sande, Marjorie I. (2003), "Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Clinical Working Case Definition, Diagnostic and Treatment Protocols" (PDF), Journal of Chronic Fatigue Syndrome, 11 (2): 7-115, doi:10.1300/J092v11n01_02
- ↑ Carruthers, Bruce M.; van de Sande, Marjorie I.; De Meirleir, Kenny L.; Klimas, Nancy G.; Broderick, Gordon; Mitchell, Terry; Staines, Donald; Powles, A. C. Peter; Speight, Nigel; Vallings, Rosamund; Bateman, Lucinda; Baumgarten-Austrheim, Barbara; Bell, David; Carlo-Stella, Nicoletta; Chia, John; Darragh, Austin; Jo, Daehyun; Lewis, Donald; Light, Alan; Marshall-Gradisnik, Sonya; Mena, Ismael; Mikovits, Judy; Miwa, Kunihisa; Murovska, Modra; Pall, Martin; Stevens, Staci (August 22, 2011). "Myalgic encephalomyelitis: International Consensus Criteria". Journal of Internal Medicine. 270 (4): 327–338. doi:10.1111/j.1365-2796.2011.02428.x. ISSN 0954-6820. PMC 3427890. PMID 21777306.
- ↑ Clayton, Ellen Wright; Alegría, Margarita; Bateman, Lucinda; Chu, Lily; Cleeland, Charles; Davis, Ronald; Diamond, Betty; Ganiats, Theodore; Keller, Betsy; Klimas, Nancy; Lerner, A Martin; Mulrow, Cynthia; Natelson, Benjamin; Rowe, Peter; Shelanski, Michael (2015). "Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome - Redefining an Illness" (PDF). nationacademies.org.
















