Postural orthostatic tachycardia syndrome
Postural orthostatic tachycardia syndrome (POTS, or postural tachycardia syndrome) is a condition in which a change from the supine position (lying horizontally) to an upright position causes an abnormally large increase in heart rate, called tachycardia. It is a form of orthostatic intolerance (OI), a type of dysautonomia, which means a dysregulation of the autonomic nervous system (ANS). The autonomic nervous system controls those functions of the body that are considered automatic and involuntary, such as heart rate, blood pressure, respiration, digestion, and arousal. Other symptoms of an orthostatic nature — occurring in response to upright posture — typically accompany the tachycardia.[1] These include, but are not limited to headaches, fatigue, sweating, nausea; fainting and dizziness. The female to male ratio of patients with POTS is 4:1.[2][3]
Onset[edit | edit source]
Onset may be linked to infection including viruses like EBV or enteroviruses, trauma, surgery or stress.[4][5]
Signs and symptoms[edit | edit source]
The main symptom of POTS is an abnormal increase in heart rate upon standing. The specific diagnostic criteria for POTS is an increase in heart rate from the lying to upright position of greater than 30 beats per minute, or a heart rate of greater than 120 beats per minute within 10 minutes of standing. There needs to be an absence of significant orthostatic hypotension (magnitude of blood pressure drop ≥ 20/10 mm Hg) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8920526/. Patients with POTS usually present with other symptoms, commonly occurring in the upright position. These include:
- Hypovolemia (low blood volume)
- High levels of plasma norepinephrine when standing
- Dizziness/lightheadedness and syncope (fainting)
- Headaches and migraines
- Cognitive impairment / brain fog
- Heart palpitations
- Chest pain
- Shortness of breath
- Sleep abnormalities
- Neuropathic pain, Coldness or pain in the extremities
- Small fiber polyneuropathy (in 50% of patients)
- Fatigue
- Exercise intolerance
- Nausea
- Tremulousness (shaking)
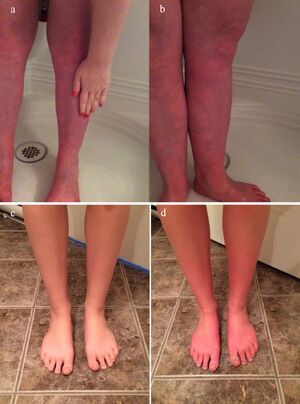
- Acrocyanosis-- reddish purple discoloration in the legs, due to poor circulation in the extremities, which returns to normal upon returning to a reclined position
- Sensory sensitivity
- Abdominal pain, gastroparesis, or rapid gastric emptying
- Elevated sympathetic tone[5][6][7][8]
Common stimuli in daily life, such as modest exertion, food ingestion and heat, can exacerbate symptoms.[9]
Potential mechanisms[edit | edit source]
Autoimmunity is thought to play a role in many cases of POTS: adrenergic[10], muscarinic[11] and other autoantibodies[12][13][14] have been found. A small study of POTS in children found that 24.39% of patients had acetylcholine receptor autoantibodies.[15]A small study of adult patients found elevated α1, β1 and β2 adrenergic receptor autoantibodies.[16]
Lax vasculature has been though to play a role in the development of POTS in people with Ehlers-Danlos Syndrome, a connective tissue disorder.[17]
Testing[edit | edit source]
Assessing orthostatic blood pressure can be done in a physician's office by measuring the patient's blood pressure while lying down, sitting, and standing at standardized time increments. Dr. Lucinda Bateman uses a modified orthostatic blood pressure assessment called the NASA 10-minute Lean Test, a variant of a test used by NASA researchers to test for orthostatic intolerance following space flight. The NASA 10-minute Lean Test is less taxing on the patient and can be done in any physician's office. Instructions are available for printout for both healthcare providers and patients.[18]
If the results of the standard orthostatic blood pressure assessment are inconclusive, a tilt table test can be used for diagnosis.[19]
Treatment[edit | edit source]
A 2012 study Diagnosis and management of postural orthostatic tachycardia syndrome: A brief review[20] concluded:
- "The pathophysiology of POTS is complex and the result of a number of separate mechanisms producing a common pattern of symptoms. The large number of clinical manifestations that characterize this disorder and the wide range of medications available, plus the clear evidence that certain medications and treatment strategies work in some, but not all POTS patients, demonstrates that POTS is a range of disorders requiring comprehensive investigation and characterisation to guide selection of the most appropriate treatment. The recent consensus statement will help to direct further research into the underlying conditions that lead to POTS."
- When the cause of POTS is able to be identified and treated in certain individuals, their POTS symptoms may subside. However, there is currently no cure for POTS on the broader level. The following treatments have been identified to improve symptoms and quality of life:
- Increasing fluid intake (2-3 liters a day)
- Increasing salt intake
- Raising the head of the bed to conserve blood volume (less blood is turned into urine by the kidneys when reclining at an angle)
- Abdominal compression garments[21]
- Diet
- Reclined exercise, such as rowing, biking, swimming (contraindicated in patients with co-morbid myalgic encephalomyelitis)
- Sodium chloride 0.9% (Normal saline)
- Medications:
- Beta-blockers
- Fludrocortisone
- Ivabradine
- Erythropoietin
- Pyridostigmine bromide (Mestinon)
- Vasoconstrictors
- NSAIDs
- Others such as methyldopa and antidepressants[8][20]
A small randomized crossover design trial found that patients with postural orthostatic tachychardia improved with Mestinon.[22]
Conditions associated with POTS[edit | edit source]
POTS is not only comorbid with a range of diseases, but its phenotype also resembles that of other disorders (e.g., ME, Ehlers-Danlos Syndrome).
ME/CFS[edit | edit source]
POTS can be a co-morbid condition in ME/CFS patients.[23][24] Estimates on the prevalence of POTS among ME/CFS patients varies widely, from 11% to 70%. In a 2008 study done in the UK by the Northern CFS/ME Clinical Network, using the Fukuda criteria, 27% of the study population had POTS compared with 9% in the control population.[25]
| Prevalence of POTS in ME/CFS population samples | ||
|---|---|---|
| Study: | number of
ME/CFS patients |
%
POTS |
| Stewart et al. 1999 | 25 | 70% |
| Schondorf et al. 1999 | 75 | 40% |
| Hoad et al. 2008 | 59 | 27% |
| Van Campen et al. 2018 | 627 | 25% |
| Dowsett & Ramsay, 1990[26] | 420 | 21% |
| Lewis et al. 2013 | 179 | 13% |
| Reynolds et al. 2014 | 306 | 11% |
| Roerink et al. 2017 | 419 | 5,7% |
A 2011 study of 58 POTS patients by the Vanderbilt Autonomic Dysfunction Center (Vanderbilt University School of Medicine, Nashville, TN, U.S.A.), reported that 64% of also met the Centers for Disease Control and Prevention (CDC) criteria for chronic fatigue syndrome.[27]
The SEID criteria requires either orthostatic intolerance (of which POTS is one type) or cognitive dysfunction for a diagnosis.[28] POTS is also a symptom of the Canadian Consensus Criteria (CCC) which diagnoses ME/CFS,[29] and the International Consensus Criteria (ICC) for diagnosing myalgic encephalomyelitis (ME).[30] However, the diagnosis of POTS alone does not automatically support a ME/CFS diagnosis and cannot be used as a diagnostic biomarker to determine ME/CFS. POTS can occur independent from ME/CFS, and, likewise, ME/CFS can occur without the symptomatology of POTS.
A 2016 study in the Netherlands by Roerink et al., found that patients with CFS who fulfilled the SEID criteria did not have a prevalence of POTS different from that in the overall ME/CFS population. In adults with ME/CFS, the prevalence of POTS was low, between 6% - 18% (depending on age), was not different from the rate in non-ME/CFS fatigued patients, and was not related to disease severity or treatment outcome.[31]
ME patients with POTS can experience impaired neurocognitive abilities (such as working memory, information processing) under increased orthostatic stress (i.e., standing, tilt table test).[32]
Other conditions associated with POTS[edit | edit source]
- Infections such as mononucleosis, Epstein-Barr virus, Lyme disease, extra-pulmonary Mycoplasma pneumonia, and Hepatitis C [37][38]
Notable research[edit | edit source]
- 2008, Postural orthostatic tachycardia syndrome is an under-recognized condition in chronic fatigue syndrome[25] (Full Text)
- 2012, Diagnosis and management of postural orthostatic tachycardia syndrome: A brief review[42] (Full Text)
- 2012, Increasing orthostatic stress impairs neurocognitive abilities in chronic fatigue syndrome with postural tachycardia syndrome[43] (Full Text)
- 2013, What is brain fog? An evaluation of the symptom in postural tachycardia syndrome[44] (Full Text)
- 2014, Postural Orthostatic Tachycardia With Chronic Fatigue After HPV Vaccination as Part of the “Autoimmune/Auto-inflammatory Syndrome Induced by Adjuvants”[45] (Full Text)
- 2014, Comorbidity of postural orthostatic tachycardia syndrome and chronic fatigue syndrome in an Australian cohort[46] (Full Text)
- 2015, An assessment of fatigue in patients with postural orthostatic tachycardia syndrome[47] (reprinted in 2017) (Abstract)
- 2016, Is Postural Orthostatic Tachycardia a Useful Diagnostic Marker in Chronic Fatigue Syndrome Patients?[48] (Abstract)
- 2016, Postural orthostatic tachycardia is not a useful diagnostic marker for chronic fatigue syndrome[49] (Abstract)
- 2018, Managing fatigue in postural tachycardia syndrome (PoTS): The Newcastle approach[50] (Abstract)
- 2018, Postural Orthostatic Tachycardia Syndrome: Prevalence, Pathophysiology, and Management[51] (Abstract)
- 2019, Postural Orthostatic Tachycardia Syndrome Is Associated With Elevated G‐Protein Coupled Receptor Autoantibodies[5] (Full text)
Learn more[edit | edit source]
- POTS UK website
- Sep 2010, Mangaging Orthostatic Intolerance[52]
- 2016, Recognizing postural orthostatic tachycardia syndrome[53]
- 2016, The Exercise Intolerance in POTS, ME/CFS and Fibromyalgia Explained?[54]
- 2019, Study may unlock new diagnostic tools for fainting disorder - possible biomarker for POTS and autoimmune evidence - University of Toledo
See also[edit | edit source]
References[edit | edit source]
- ↑ Mar, Philip L.; Raj, Satish R. (2014). "Neuronal and hormonal perturbations in postural tachycardia syndrome". Frontiers in Physiology. 5: 220. doi:10.3389/fphys.2014.00220. ISSN 1664-042X. PMID 24982638.
- ↑ "PoTS - Postural Tachycardia Syndrome". PoTS UK. Retrieved August 16, 2018.
- ↑ "PoTS - Postural Tachycardia Syndrome - What is POTS?". PoTS UK. Retrieved August 16, 2018.
- ↑ Grahame, Rodney; Kirbis, Mojca; Andrew P. Owens; Iodice, Valeria; Low, David A.; Mathias, Christopher J. (January 2012). "Postural tachycardia syndrome—current experience and concepts". Nature Reviews Neurology. 8 (1): 22–34. doi:10.1038/nrneurol.2011.187. ISSN 1759-4766.
- ↑ 5.0 5.1 5.2 Gunning, William T.; Kvale, Heather; Kramer, Paula M.; Karabin, Beverly L.; Grubb, Blair P. (September 17, 2019). "Postural Orthostatic Tachycardia Syndrome Is Associated With Elevated G‐Protein Coupled Receptor Autoantibodies". Journal of the American Heart Association. 8 (18): e013602. doi:10.1161/JAHA.119.013602.
- ↑ "Symptoms of Postural Orthostatic Tachycardia Syndrome (POTS)". Standing Up to POTS. July 9, 2018.
- ↑ Raj, Satish R (April 1, 2006). "The Postural Tachycardia Syndrome (POTS): Pathophysiology, Diagnosis & Management". Indian Pacing and Electrophysiology Journal. 6 (2): 84–99. ISSN 0972-6292. PMC 1501099. PMID 16943900.
- ↑ 8.0 8.1 8.2 "Dysautonomia International: Postural Orthostatic Tachycardia Syndrome". dysautonomiainternational.org. Retrieved October 25, 2018.
- ↑ 9.0 9.1 Grahame, Rodney; Kirbis, Mojca; Andrew P. Owens; Iodice, Valeria; Low, David A.; Mathias, Christopher J. (January 2012). "Postural tachycardia syndrome—current experience and concepts". Nature Reviews Neurology. 8 (1): 22–34. doi:10.1038/nrneurol.2011.187. ISSN 1759-4766.
- ↑ Kem, David C.; Melander, Olle; Sutton, Richard; Scofield, Robert Hal; Quadri, Syed M.S.; Murphy, Taylor A.; Liles, Campbell; Harris, Valerie M.; Koelsch, Kristi A. (July 1, 2017). "Antiadrenergic autoimmunity in postural tachycardia syndrome". EP Europace. 19 (7): 1211–1219. doi:10.1093/europace/euw154. ISSN 1099-5129.
- ↑ Yu, Xichun; Stavrakis, Stavros; Hill, Michael A.; Huang, Shijun; Reim, Sean; Li, Hongliang; Khan, Muneer; Hamlett, Sean; Cunningham, Madeleine W. (January 1, 2012). "Autoantibody activation of beta-adrenergic and muscarinic receptors contributes to an "autoimmune" orthostatic hypotension". Journal of the American Society of Hypertension. 6 (1): 40–47. doi:10.1016/j.jash.2011.10.003. ISSN 1933-1711.
- ↑ Thieben, Mark J.; Sandroni, Paola; Sletten, David M.; Benrud-Larson, Lisa M.; Fealey, Robert D.; Vernino, Steven; Low, Phillip A.; Lennon, Vanda A.; Shen, Win-Kuang (March 1, 2007). "Postural Orthostatic Tachycardia Syndrome: The Mayo Clinic Experience". Mayo Clinic Proceedings. 82 (3): 308–313. doi:10.4065/82.3.308. ISSN 0025-6196.
- ↑ Li Hongliang; Yu Xichun; Liles Campbell; Khan Muneer; Vanderlinde‐Wood Megan; Galloway Allison; Zillner Caitlin; Benbrook Alexandria; Reim Sean. "Autoimmune Basis for Postural Tachycardia Syndrome". Journal of the American Heart Association. 3 (1): e000755. doi:10.1161/JAHA.113.000755. PMC 3959717. PMID 24572257.
- ↑ Lennon, Vanda; Low, Phillip; Klein, Christopher; Singer, Wolfgang (April 6, 2015). "Autoantibodies in the Postural Tachycardia Syndrome (P1.272)". Neurology. 84 (14 Supplement): P1.272. ISSN 0028-3878.
- ↑ Li, Jiawei; Zhang, Qingyou; Liao, Ying; Zhang, Chunyu; Hao, Hongjun; Du, Junbao (August 3, 2014). "The Value of Acetylcholine Receptor Antibody in Children with Postural Tachycardia Syndrome". Pediatric Cardiology. 36 (1): 165–170. doi:10.1007/s00246-014-0981-8. ISSN 0172-0643.
- ↑ Li, Hongliang; Yu, Xichun; Liles, Campbell; Khan, Muneer; Vanderlinde‐Wood, Megan; Galloway, Allison; Zillner, Caitlin; Benbrook, Alexandria; Reim, Sean (January 27, 2014). "Autoimmune Basis for Postural Tachycardia Syndrome". Journal of the American Heart Association. 3 (1). doi:10.1161/jaha.113.000755. ISSN 2047-9980. PMC 3959717. PMID 24572257.
- ↑ Hakim, Alan; O'Callaghan, Chris; Wandele, Inge De; Stiles, Lauren; Pocinki, Alan; Rowe, Peter (2017). "Cardiovascular autonomic dysfunction in Ehlers–Danlos syndrome—Hypermobile type". American Journal of Medical Genetics Part C: Seminars in Medical Genetics. 175 (1): 168–174. doi:10.1002/ajmg.c.31543. ISSN 1552-4876.
- ↑ Bateman, Lucinda (September 27, 2016). "Simple Way to Assess Orthostatic Intolerance - Bateman Horne Center". Bateman Horne Center Newsletter. Retrieved August 16, 2018.
- ↑ "How Doctors Diagnose & Test for POTS". MyHeart. Retrieved August 16, 2018.
- ↑ 20.0 20.1 Abed, Howraa; Ball, Patrick A; Wang, Le-Xin (2012). "Diagnosis and management of postural orthostatic tachycardia syndrome: A brief review". Journal of Geriatric Cardiology : JGC. 9 (1): 61–67. doi:10.3724/SP.J.1263.2012.00061. ISSN 1671-5411. PMID 22783324.
- ↑ Miller, Amanda J.; Bourne, Kate M. (July 21, 2020). "Abdominal Compression as a Treatment for Postural Tachycardia Syndrome". Journal of the American Heart Association. 9 (14): e017610. doi:10.1161/JAHA.120.017610. ISSN 2047-9980. PMC 7660708. PMID 32673524.
- ↑ Raj, S.R. (May 31, 2005). "Acetylcholinesterase Inhibition Improves Tachycardia in Postural Tachycardia Syndrome". Circulation. 111 (21): 2734–2740. doi:10.1161/circulationaha.104.497594. ISSN 0009-7322.
- ↑ "POTS in ME/CFS". Freedom From ME - The Optimum Health Clinic on YouTube. August 2, 2014.
- ↑ "Overlapping Conditions – American ME and CFS Society". ammes.org. Retrieved August 12, 2018.
- ↑ 25.0 25.1 Hoad, A.; Spickett, G.; Elliott, J.; Newton, J. (2008). "Postural orthostatic tachycardia syndrome is an under-recognized condition in chronic fatigue syndrome". QJM: monthly journal of the Association of Physicians. 101 (12): 961–965. doi:10.1093/qjmed/hcn123. ISSN 1460-2393. PMID 18805903.
- ↑ Dowsett, E. G.; Ramsay, A.M.; McCartney, R.A.; Bell, E.J. (July 1990). "Myalgic encephalomyelitis--a persistent enteroviral infection?". Postgraduate Medical Journal. 66 (777): 526–530. ISSN 0032-5473. PMC 2429637. PMID 2170962.
- ↑ Okamoto, Luis E.; Raj, Satish R.; Peltier, Amanda; Gamboa, Alfredo; Shibao, Cyndya; Diedrich, André; Black, Bonnie K.; Robertson, David; Biaggioni, Italo (February 1, 2012). "Neurohumoral and haemodynamic profile in postural tachycardia and chronic fatigue syndromes". Clinical Science (London, England : 1979). 122 (Pt 4): 183–192. doi:10.1042/CS20110200. ISSN 0143-5221. PMID 21906029.
- ↑ Institute of Medicine (March 16, 2015). Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Redefining an Illness. Washington, DC: The National Academies Press. Box 4-3, p 114. doi:10.17226/19012 – via NAP.edu.
- ↑ "Canadian Consensus Criteria - MEpedia". me-pedia.org. Retrieved August 16, 2018.
- ↑ "International Consensus Criteria - MEpedia". me-pedia.org. Retrieved August 16, 2018.
- ↑ Roerink, M. E.; Lenders, J. W.M.; Schmits, I.C.; Pistorius, A.M.A.; Smit, J.W.; Knoop, H.; van der Meer, J.W.M. (October 2, 2016). "Postural orthostatic tachycardia is not a useful diagnostic marker for chronic fatigue syndrome". Journal of Internal Medicine. 281 (2): 179–188. doi:10.1111/joim.12564. ISSN 0954-6820.
- ↑ Ocon, Anthony J.; Messer, Zachary R.; Medow, Marvin S.; Stewart, Julian M. (March 2012). "Increasing orthostatic stress impairs neurocognitive functioning in chronic fatigue syndrome with postural tachycardia syndrome". Clinical Science (London, England : 1979). 122 (5): 227–238. doi:10.1042/CS20110241. ISSN 0143-5221. PMC 3368269. PMID 21919887.
- ↑ "Overlapping Conditions - American Myalgic Encephalomyelitis and Chronic Fatigue Syndrome Society". ammes.org. Retrieved August 12, 2018.
- ↑ Yun, Dong Joo; Choi, Han Na; Oh, Gun-Sei (2013). "A Case of Postural Orthostatic Tachycardia Syndrome Associated with Migraine and Fibromyalgia". The Korean Journal of Pain. 26 (3): 303–306. doi:10.3344/kjp.2013.26.3.303. ISSN 2005-9159. PMID 23862007.
- ↑ Weig, Spencer G.; Buckthal, Paul E.; Choi, Samuel K.; Zellem, Ronald T. (October 1, 1991). "Recurrent syncope as the presenting symptom of Arnold‐Chiari malformation". Neurology. 41 (10): 1673–1673. doi:10.1212/WNL.41.10.1673. ISSN 0028-3878. PMID 1922816.
- ↑ Prilipko, O.; Dehdashti, A.R.; Zaim, S.; Seeck, M. (July 1, 2005). "Orthostatic intolerance and syncope associated with Chiari type I malformation". Journal of Neurology, Neurosurgery & Psychiatry. 76 (7): 1034–1036. doi:10.1136/jnnp.2004.048330. ISSN 0022-3050. PMID 15965223.
- ↑ Kanjwal, Khalil; Karabin, Beverly; Kanjwal, Yousuf; Grubb, Blair P. (2011). "Postural orthostatic tachycardia syndrome following Lyme disease". Cardiology Journal. 18 (1): 63–66. ISSN 1897-5593. PMID 21305487.
- ↑ Kasmani, Rahil; Elkambergy, Hossam; Okoli, Kelechi (September 2009). "Postural Orthostatic Tachycardia Syndrome Associated With Mycoplasma pneumoniae". Infectious Diseases in Clinical Practice. 17 (5): 342–343. doi:10.1097/IPC.0b013e318191781b. ISSN 1056-9103.
- ↑ Kanjwal, Khalil; Karabin, Beverly; Kanjwal, Yousuf; Saeed, Bilal; Grubb, Blair P. (October 2010). "Autonomic dysfunction presenting as orthostatic intolerance in patients suffering from mitochondrial cytopathy". Clinical Cardiology. 33 (10): 626–629. doi:10.1002/clc.20805. ISSN 1932-8737. PMID 20960537.
- ↑ Raj, Satish R (April 1, 2006). "The Postural Tachycardia Syndrome (POTS): Pathophysiology, Diagnosis & Management". Indian Pacing and Electrophysiology Journal. 6 (2): 84–99. ISSN 0972-6292. PMC 1501099. PMID 16943900.
- ↑ Garland, Emily M; Celedonio, Jorge E; Raj, Satish R (September 2015). "Postural Tachycardia Syndrome: Beyond Orthostatic Intolerance". Current neurology and neuroscience reports. 15 (9): 60. doi:10.1007/s11910-015-0583-8. ISSN 1528-4042. PMC 4664448. PMID 26198889.
- ↑ Abed, Howraa; Ball, Patrick A; Wang, Le-Xin (2012). "Diagnosis and management of postural orthostatic tachycardia syndrome: A brief review". Journal of Geriatric Cardiology : JGC. 9 (1): 61–67. doi:10.3724/SP.J.1263.2012.00061. ISSN 1671-5411. PMID 22783324.
- ↑ Ocon, Anthony J.; Messer, Zachary R.; Medow, Marvin S.; Stewart, Julian M. (2012). "Increasing orthostatic stress impairs neurocognitive functioning in chronic fatigue syndrome with postural tachycardia syndrome". Clinical Science (London, England : 1979). 122 (5): 227–238. doi:10.1042/CS20110241. ISSN 0143-5221. PMC 3368269. PMID 21919887.
- ↑ Ross, Amanda J.; Medow, Marvin S.; Rowe, Peter C.; Stewart, Julian M. (September 3, 2013). "What is brain fog? An evaluation of the symptom in postural tachycardia syndrome". Clinical Autonomic Research. 23 (6): 305–311. doi:10.1007/s10286-013-0212-z. ISSN 0959-9851. PMID 23999934.
- ↑ Tomljenovic, Lucija; Colafrancesco, Serena; Perricone, Carlo; Shoenfeld, Yehuda (March 13, 2014). "Postural Orthostatic Tachycardia With Chronic Fatigue After HPV Vaccination as Part of the "Autoimmune/Auto-inflammatory Syndrome Induced by Adjuvants"". Journal of Investigative Medicine High Impact Case Reports. 2 (1). doi:10.1177/2324709614527812. ISSN 2324-7096. PMID 26425598.
- ↑ Reynolds, G. K.; Lewis, D.P.; Richardson, A.M.; Lidbury, B.A. (November 29, 2013). "Comorbidity of postural orthostatic tachycardia syndrome and chronic fatigue syndrome in an Australian cohort". Journal of Internal Medicine. 275 (4): 409–417. doi:10.1111/joim.12161. ISSN 0954-6820.
- ↑ Wise, Shelby; Ross, Amanda; Brown, Abigail; Evans, Meredyth; Jason, Leonard (November 4, 2015). "An assessment of fatigue in patients with postural orthostatic tachycardia syndrome". Journal of Health Psychology. 22 (6): 733–742. doi:10.1177/1359105315613624. ISSN 1359-1053.
- ↑ Roerink, M.E.; Lenders, J.W.M; Schmits, I.C.; Pistorius, A.; Knoop, H.; van der Meer, J.W.M. (2016). "Is Postural Orthostatic Tachycardia a Useful Diagnostic Marker in Chronic Fatigue Syndrome Patients?". Journal of Psychosomatic Research. 85: 78. doi:10.1016/j.jpsychores.2016.03.193. ISSN 0022-3999.
- ↑ Roerink, M. E.; Lenders, J. W.M.; Schmits, I.C.; Pistorius, A.M.A.; Smit, J.W.; Knoop, H.; van der Meer, J.W.M. (October 2, 2016). "Postural orthostatic tachycardia is not a useful diagnostic marker for chronic fatigue syndrome". Journal of Internal Medicine. 281 (2): 179–188. doi:10.1111/joim.12564. ISSN 0954-6820.
- ↑ Strassheim, Victoria; Welford, Jenny; Ballantine, Rob; Newton, Julia L. (December 2018). "Managing fatigue in postural tachycardia syndrome (PoTS): The Newcastle approach". Autonomic Neuroscience. 215: 56–61. doi:10.1016/j.autneu.2018.02.003.
- ↑ Zadourian, Adena; Doherty, Taylor A.; Swiatkiewicz, Iwona; Taub, Pam R. (June 15, 2018). "Postural Orthostatic Tachycardia Syndrome: Prevalence, Pathophysiology, and Management". Drugs. 78 (10): 983–994. doi:10.1007/s40265-018-0931-5. ISSN 0012-6667.
- ↑ "Managing Orthostatic Intolerance". SolveCFS on YouTube. September 1, 2010.
- ↑ Pavlik, Daniel; Agnew, Donna; Stiles, Lauren; Ditoro, Rachel (2016). "Recognizing postural orthostatic tachycardia syndrome". JAAPA: official journal of the American Academy of Physician Assistants. 29 (4): 17–23. doi:10.1097/01.JAA.0000481398.76099.09. ISSN 1547-1896. PMID 26967958.
- ↑ Johnson, Cort (July 4, 2016). "The Exercise Intolerance in POTS, ME/CFS and Fibromyalgia Explained? - Health Rising". Health Rising. Retrieved August 16, 2018.

